Faced with a global epidemic of HIV, the World Health Organization advised back in 2015 that a new health policy, summed up as “Treat All”, be adopted in all health facilities around the world that deal with HIV patients. This recommendation to immediately treat any and all patients proved to have HIV infection has been put into practice almost immediately in a vast majority of testing and treatment centers, unlike many other policies, and has become standard-of-care practice.
The Treat All or Test and Treat policy guideline for people living with HIV (PLHIV) envisages that 90% of these individuals be diagnosed, 90% of diagnosed cases be treated with combination ART, and 90% of treated patients successfully achieve suppression of viral load by 2020. The aim of the program was to interrupt virus transmission, prevent HIV-related illness and death, and meet the goals of the 2014 United Nations Program on HIV/AIDS that aims to stop the HIV epidemic.
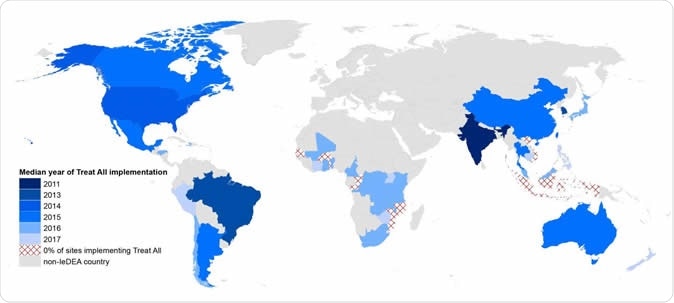
This is a map of the implementation of the WHO's 'Treat All' recommendation across the globe. Image Credit: CUNY ISPH
A high degree of compliance with this recommendation was shown by the current study published in the Journal of the International AIDS Society. It looked at a sample of over 200 healthcare centers in 41 countries that take part in the research initiative International epidemiology Databases to Evaluate AIDS (IeDEA) to evaluate the level of implementation of this policy. At 93% of all sites dealing with cases of HIV in adults, irrespective of region or location, the practice had switched to Treat All. In fact, in countries which had adopted this as a national guideline, 97% of sites implemented this policy.
The greatest divergence was in West Africa where only 63% of healthcare sites dealing with HIV had adopted this practice, and was linked to a failure of national policy switch in these states at the time of the study. Overall, even where Treat All has not become part of national policy, almost 70% of healthcare sites had already adopted this strategy about seven months, on average, before the current study.
National policy support followed the implementation of this guideline in about a third of cases, and in all cases there was typically less than one month of delay between the time that it became part of national policy and its adoption at ground level. Other guidelines on HIV treatment have been issued by the WHO and other bodies in the past, but none have been implemented so fast.
Even in low-income countries, most patients are put on HIV treatment on the same day as diagnosis. Overall, 77% of facilities are able to begin treatment with antiretroviral therapy (ART) within 14 days of confirmed diagnosis. While there are also similar differences in the use of routine pre-ART initiation counseling sessions for patients, these did not affect the time to the start of treatment.It appears that HIV treatment is broadly available everywhere, without noticeable gaps in service on the basis of geographic location, national economic level, urban or rural location, or type of health facility.
Lead author Ellen Brazier says, “These findings are promising, in terms of the ability to broadly improve access to earlier treatment in low-resource settings, which will improve health outcomes among people living with HIV and prevent new infections.”
The quick pace of implementation of the Treat All guidelines may be, in part, due to their simplicity as compared to earlier recommendations which required eligibility criteria for HIV treatment to be assessed for each patient in terms of immune status (both clinically-based stage classification and CD4+ count).
One relevant finding which could affect the long-term success of the strategy was that most low-resource communities could not support routine viral load monitoring after the initiation of HIV treatment. In low-income and lower-middle-income groups, only 40% and 52% of treatment centers, respectively, had facilities for routine viral load testing, as compared to rates of over 93% in higher-income countries. This disparity was also obvious in urban vs rural sites (81% vs 37%) and in higher-level centers vs health centers (82% vs 57%). Overall, one-third of treatment centers cannot routinely carry out viral load monitoring.
Senior study author Denis Nash noted that the limited scope of viral load monitoring is a serious issue. Nash points out, “Many of the sites that are initiating patients on antiretroviral therapy do not have adequate resources to monitor key patient outcomes through viral load testing, including treatment failure or the development of drug resistance. his is an issue that requires urgent attention, as it is critical to assess and optimize longer term HIV care outcomes in the Treat All era.”
Journal reference:
Postoperative complications in combined gynecologic, plastic, and breast surgery: An analysis from National Surgical Quality Improvement Program, Sarah E. Tevis MD Jennifer G. Steiman MD Heather B. Neuman MD Caprice C. Greenberg MD, MPH Lee G. Wilke MD, First published: 06 July 2019 https://doi.org/10.1111/tbj.13429, https://onlinelibrary.wiley.com/doi/abs/10.1111/tbj.13429