A new study in the American Journal of Psychiatry says deep brain stimulation is an effective treatment in depressed patients who do not respond to other forms of therapy. The study published on October 4, 2019, looked at the long-term effects on patients who had received electrical stimulation to the subcallosal cingulate area of the brain. The subcallosal cingulate area of the brain is also called Brodmann Area 25, and has been targeted by researchers as a possible focus for antidepressant stimulation.
Deep brain stimulation (DBS) is a neurosurgical procedure in which an implant is placed deep within the brain. This implant, called a neurostimulator, emits electrical signals at a selected high frequency to stimulate that particular part of the brain. DBS has been used to treat Parkinson’s disease, epilepsy, obsessive-compulsive disorder and essential tremor, four conditions for which it has gained US Food and Drug Administration (FDA) approval.
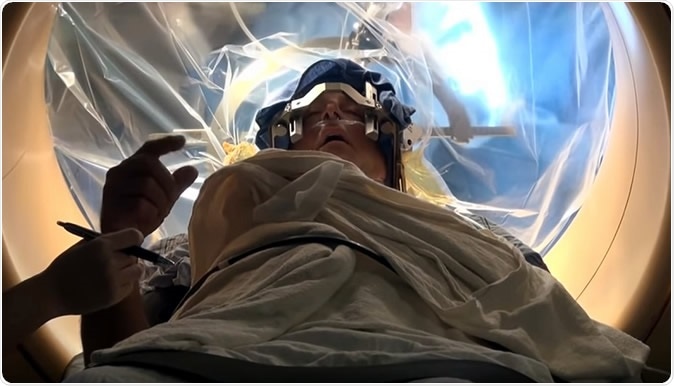
Deep Brain Stimulation. Image Credit: Mount Sinai Health System
In a series of small open-label trials of DBS in treatment-resistant depression, the results were generally favorable. However, when a larger randomized trial held at multiple centers failed to show statistically significant results at the predefined six-month assessment point, it was stopped ahead of time. The present study builds on the earlier findings from the first 28-patient open-label trial, showing significantly positive results with long-term follow-up of these patients.
Not only were the patients continuing to show improvement, the improvement lasted for years. In fact, the researchers say, the majority of participants had a strong and durable response to DBS focused on Area 25 that was observed for the more than 8 years of follow-up. This is amazing, given that patients with treatment-resistant depression have a high tendency to relapse. No unacceptable side effects were reported, and the procedure was well-tolerated in general.
In the first trial, all participants had either bipolar disorder type 2 (7 patients) or major depression (20 patients), and all had been experiencing their current episode of depression for 12 months or more. They had been treated with four or more different drugs, as well as psychotherapy and electroconvulsive (‘shock’) therapy. The entire group was treated at the Emory University School of Medicine with the same device implanted by the same surgeon. The first 17 had implants performed over the years 2007-2009, followed by a one-month lead-in period, when the device was switched off. The next 11 received the implant over the period 2011-2013 via fractography-guided surgery.
All patients saw a psychiatrist involved in the study once a week for 32 weeks, beginning with four or more weekly sessions before surgery. After 32 weeks, the frequency was brought down to once every six months from year 2-8. At the time of the report, there were 23 patients still on follow-up. The total duration of assessment came to 178 patient-years.
The researchers examined long-term outcomes assessed over 4-8 years in 28 patients, of whom half (14 patients) were studied for the full 8-year period or more. Another 11 patients remained under assessment for four years or more.
They found that more than half the patients responded to treatment (as per predefined criteria), while 75% of them had a positive treatment response for over 50% of the time that they remained in the study. About one in five showed a constant improvement from year 1 on. Over 30% of them went into and remained in remission (disappearance of any signs of depression). The researchers say, “Data presented through this study support the long-term safety and sustained efficacy of SCC DBS for treatment-resistant depression.” According to another researcher, Andrea Crowell, “For people suffering from inescapable depression, the possibility that DBS can lead to significant and sustained improvement in depressive symptoms over several years will be welcome news."
The importance of these findings in the current context lies in the fact that they come from a long-term study of patients who underwent a treatment for a condition that is notoriously hard to treat; a subsequent trial failed to show benefit and was halted early; but the true impact of the treatment came through only from a long-term assessment. Thus it adds to the sum of knowledge about the limitations of a typical clinical trial as well as showing that treatment-resistant depression can be improved significantly and in a sustained manner over several years.
Researcher Helen S. Mayberg says, “The ability of DBS to support long-term maintenance of an antidepressant response and prevention of relapse is a treatment advance that can mean the difference between getting on with your life or always looking over your shoulder for your next debilitating depressive episode.”
The researchers are looking forward to taking these findings forwards with a new prototype device called the Summit RC+S DBS system. This allows researchers to follow the brain activity from the site of the implant while DBS stimulation is proceeding. Researchers will also look at images of the brain, patient behavior and bodily parameters at scheduled points. This will, it is hoped, help to trace the path of recovery at multiple time levels, from days to months. Knowing more about brain events during DBS will also help optimize the use of these devices to achieve the best clinical response in this disease condition.
Journal reference:
Long-term outcomes of subcallosal cingulate deep brain stimulation for treatment-resistant depression. Andrea L. Crowell, Patricio Riva-Posse, Paul E. Holtzheimer, Steven J. Garlow, Mary E. Kelley, Robert E. Gross, Lydia Denison, Sinead Quinn, & Helen S. Mayberg. https://ajp.psychiatryonline.org/doi/abs/10.1176/appi.ajp.2019.18121427?journalCode=ajp