A new study by an international team of researchers and published on the preprint server medRxiv* in July 2020 describes a model to estimate the actual undercounting of COVID-19 cases and the global prevalence.
As of today, there are well over 12.23 million confirmed cases of COVID-19 and over 554,000 deaths worldwide. To control the rampant spread of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), many countries have resorted to nonpharmaceutical interventions (NPIs) such as imposing lockdowns, self-isolation and quarantine measures, as well as closures of workplaces and schools, and other public places like stores and supermarkets. Social gatherings have been placed under a ban, while face masks and physical distancing when out of the home have become the norm in many countries.
However, the high infectivity of the virus, along with the long incubation period, allows a high percentage of transmission to occur in the asymptomatic period. Thus, many infections remain undetected, with only a fraction of the true number being reported.
The current study aimed at using data on reported cases and deaths as well as estimates of disease severity to estimate how many cases are under-reported over time. Using data from countries with more than ten deaths, the researchers paint a picture of the epidemic in all countries and compare the cumulative incidence estimates against the actual seroprevalence where it is available. Finally, they derive the adjusted case number graphs for the ten countries with the highest confirmed and adjusted case numbers and then estimate the global prevalence.
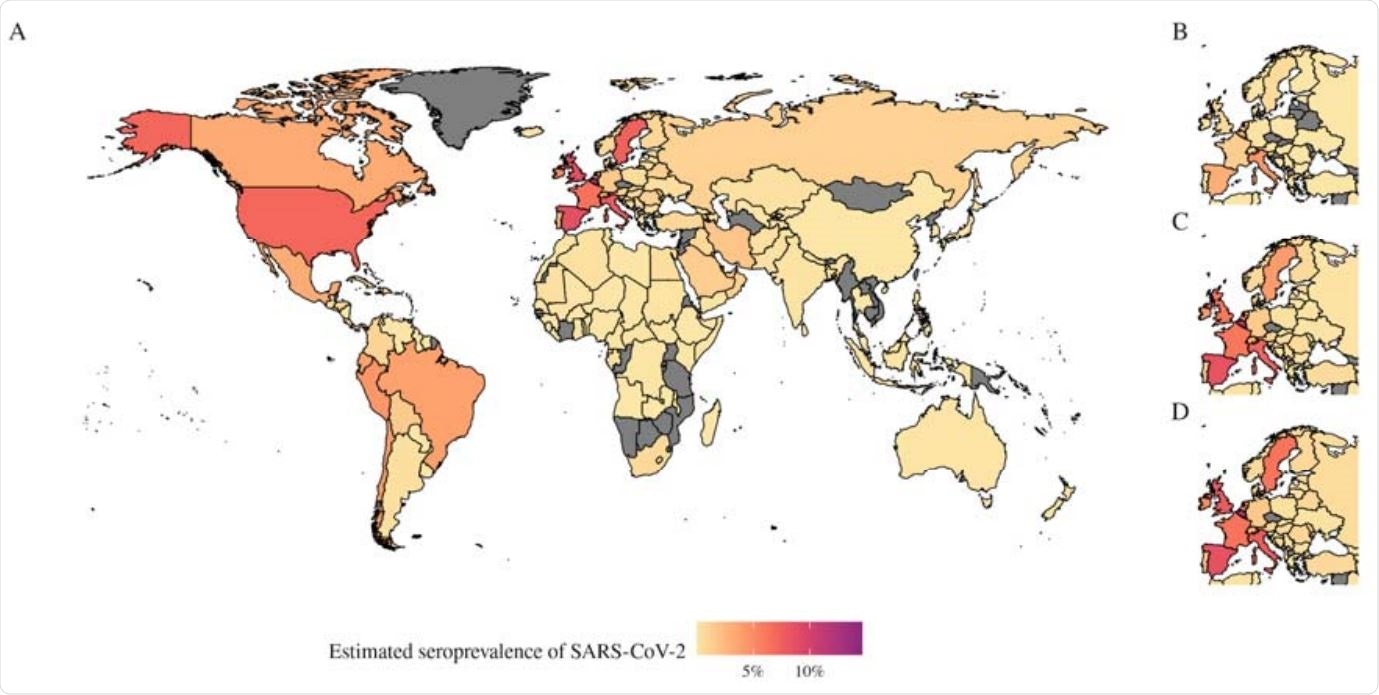
Map of estimated seroprevalence in different countries over time. A) Estimated seroprevalence of SARS-CoV-2 globally as of 7th June 2020, for all countries we have estimates for. B–D) The estimated seroprevalence of SARS-Cov-2 in Europe on B) 31st March, C) 30th April and D) 31st May.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Variation in Proportion of Detected Symptomatic Cases
There was a significant variation in the proportion of symptomatic to asymptomatic cases over time, from 2.4% in Bangladesh to 99.6% in Chile. In Europe, the median percentage of symptomatic cases that were detected varied from 4.81% in France to 85.5% in Cyprus.
When testing is ramped up, there could be an increasing proportion of detected symptomatic cases. However, when the researchers compared the estimated proportion of detected cases with the number of tests performed per new case per day, the moving average over a 7-day period showed that countries that tested at a high level did not have high levels of case detection.
For instance, while the UK was performing 80 tests to detect one new case, in one two-week period in March, it picked up only 3-10% of cases at this time. In other words, testing alone does not ensure that most cases will be detected.
Poor Detection at Epidemic Peak
From the time trends recorded, they found that during March, April and May, European countries detected anywhere between about 5% to 86% of cases, 6% to 100%, and 11% to 86%, respectively. To achieve this, the number of tests per new case detected was about 3 to 76, 3 to 832, and 12 to 1,334, respectively.
Countries, where the total number of confirmed and adjusted cases was highest, had a much larger and higher symptomatic cases graph, at 1.4 to 18 times as large as the reported case peak. Where the peak clearly occurred before the end of May 2020, the subsequent decline was also steeper than that shown by the confirmed case curves. Thus, at the peak of the epidemic in many countries, far fewer cases were being ascertained than actually existed.
Model Estimates Agree with Seroprevalence Studies
On comparing the estimated proportion of infected individuals with seroprevalence studies, they were found to agree well except in the case of Denmark, where the observed seroprevalence was underestimated.
When the estimation method was extended to all countries with case and death reports over time, they obtained a map of seroprevalence estimates by July 16, 2020, showing that most infections were focused in the US and Europe. The model estimates that about 0.02% to 15% of different populations have been infected in Europe, while for Africa and Latin America, between 0 and 3.5% have been infected as of this date.
The model also suggests that the early spread of the pandemic in Europe involved a prevalence that was one order of magnitude higher than the number of confirmed cases.
Limitations
The study was based on a baseline case fatality rate of 1.4% and the assumption that 10% to 70% of infections were asymptomatic. Secondly, the study assumes the accurate reporting of all COVID-19 deaths. However, the model estimates agree with available serologic data.
Applications and Implications
The researchers say this type of model could indicate whether a substantial proportion of cases is being reported, and hence help to trace the success of possible containment measures. This also helps to trace the progress of the pandemic. For instance, it is known that most UK infections from February to early March 2020 were imported from Italy, Spain, and France, which agrees with the model estimates, showing that more than 6.5% of the population of each of these countries was infected by the end of March 2020.
However, it is important to understand the true extent of unreported infections in a country to take proper measures to control the spread. This would include planning the speed and extent of NPIs. It would also facilitate the understanding of the actual measure of spread. If the proportion of reported to actual infections drops with the spread of the epidemic, the proportion of confirmed cases will be falsely low. In the declining phase, on the other hand, if more cases are detected, this phase may not be recognized.
Thus, the study shows, “Reported case counts will therefore likely underestimate the rate of outbreak growth initially and underestimate the decline in the later stages of an epidemic.”
Therefore, under-ascertainment of the number of cases could lead to unnecessary slowness in taking NPIs, under the false belief that cases are declining due to the measures already in place. On the other hand, if the decline is not charted, NPIs could be held in place for longer than really needed.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources