The team’s molecular surveillance study, which included samples from more than 3,000 patients, detected SARS-CoV-2 RNA in specimens collected during the week ending 25th January.
The samples were respiratory pathogen-negative (RPN)-specimens taken from patients being evaluated for flu-like illness and respiratory symptoms during the first ten weeks of 2020.
Emilia Sordillo and colleagues say the findings indicate that SARS-CoV-2 infections were present among a small number of people seeking care at the Mount Sinai Health System (MSHS) several weeks prior to the surge of cases that flooded the NYC health system.
The researchers advise that systematically screening people with unexplained respiratory illness for the presence of emerging viruses must become an essential component of approaches aiming to stop local infections from becoming uncontrollable outbreaks.
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
NYC quickly emerged as an early COVID-19 epicenter
Following the initial identification of SARS-CoV-2 in Wuhan, China, in December 2019, the virus spread to other Asian countries, Europe and North America, within a matter of weeks.
In the United States, the first infection identified on 20th January 2020 was followed by sporadic cases of infection throughout the country.
Following the first SARS-CoV-2 diagnosis in NYC on 29th February, the city quickly emerged as an early epicenter of COVID-19.
“However, prior to mid-March, 2020, COVID-19 case detection was limited by restricted availability of diagnostic testing and overlap in symptom presentation with other respiratory and viral illnesses,” writes Sordillo and colleagues. “Thus, direct molecular evidence of SARS-CoV-2 in NYC prior to the first reported case is lacking.”
What did the researchers do?
To systematically delineate the emergence of SARS-CoV-2 in NYC, the researchers applied a sample pooling strategy to screen RPN nasopharyngeal samples from 3,040 individuals who presented with respiratory symptoms or influenza-like illness at the MSHS during the first ten weeks of 2020.
This yielded 304 RPN pools that were then screened for SARS-CoV-2 RNA using nucleic-acid amplification testing (NAAT).
This assay tested for the presence of the SARS-CoV-2-specific ORF1ab gene (target 1) and the pan-Sarbecovirus envelope (E)-gene (target 2).
Results were categorized as positive for SARS-CoV-2 RNA if target 1 or both targets were detected, “presumptive positive” if only target 2 was detected, and negative if neither target was detected.
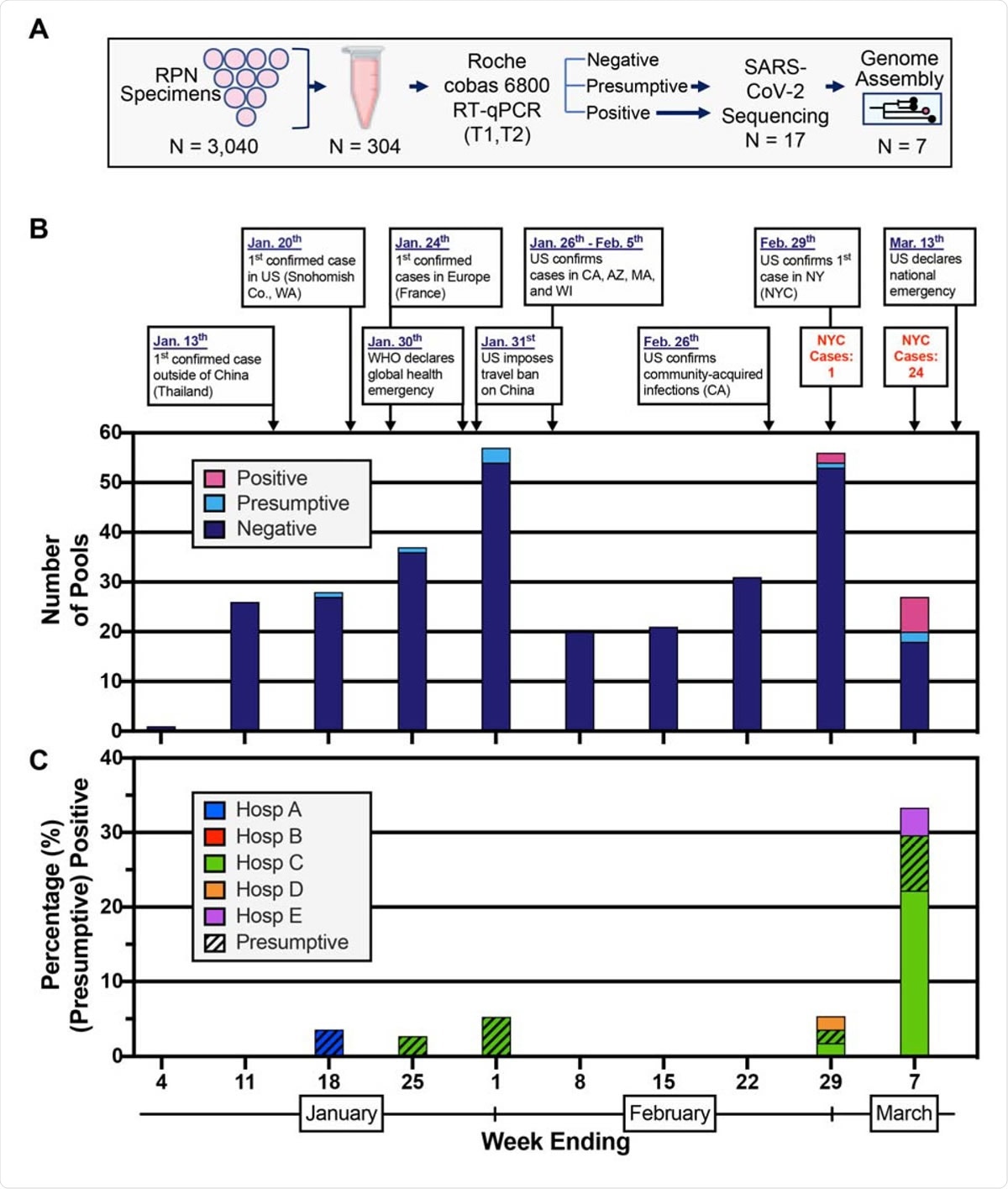
Detection of SARS-CoV-2 nucleic acids in nasopharyngeal specimens collected in the first ten weeks of 2020. (A) Schematic representation of the study design. Nasopharyngeal swab specimens that tested negative for respiratory pathogens (RPN) were pooled. Each pool consisted of 10 specimens from the same week from one of five hospital sites. Nucleic acid amplification testing (NAAT) was performed and RNA was processed for SARS-CoV-2 genome assembly. (B) Select events and responses to the evolving SARS-CoV-2 pandemic are annotated over the timeframe surveyed. Confirmed cases in NYC for the last two weeks are noted. Absolute counts of pools that tested positive, presumptive positive, and negative by RT-PCR are depicted by week collected. (C) Distribution of positive (solid) and presumptive positive (hatched) pools across the five different hospital sites in NYC.
What did the study find?
Of the 304 RPN pools that were screened, nine (3%) tested positive for SARS-CoV-2 RNA, eight (2.6%) tested presumptive positive and 287 (94.4%) tested negative.
Five of the presumptive positive pools included samples collected during the weeks ending 18th January, 25th January, and 1st February.
None of the RPN pools comprising samples collected over the following three weeks yielded detectable SARS-CoV-2 RNA.
Viral RNA was detected in 5.4% of RPN pools comprising samples collected in the week ending 29th February and in 33.3% of pools containing samples collected during the week ending 7th March.
To validate the NAAT results, the team performed genome sequencing of viral RNA extracted from all positive and presumptive-positive RPN pools.
Three pools containing samples collected during the weeks ending 25th January and 1st February yielded scattered SARS-CoV-2 reads throughout the viral genome, thereby confirming the presence of SARS-CoV-2 RNA.
What are the study implications?
“Taken together, we provide clear evidence that SARS-CoV-2 infections were present in NYC at least 6 to 8 weeks prior to the surge of cases that flooded the NYC health system,” writes Sordillo and colleagues.
The team says the high number of SARS-CoV-2 positive RPN pools during the first week of March explains the “sudden” exponential increase in the number of severe COVID-19 cases that were admitted to MSHS hospitals from mid-March 2020.
“Systematic, unbiased surveillance of clinical specimens obtained from individuals presenting with unexplained or unusual clinical presentations of respiratory illness for the presence of emerging viral pathogens must be a key component of any future early-warning sentinel programs,” say the researchers.
“These systematic measures will need to become essential components of our new normal in order to prevent local infections and transmissions from blooming into uncontrolled outbreaks,” they conclude.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Sordillo E, et al. Before the Surge: Molecular Evidence of SARS-CoV-2 in New York City Prior to the First Report. medRxiv, 2021. doi: https://doi.org/10.1101/2021.02.08.21251303, https://www.medrxiv.org/content/10.1101/2021.02.08.21251303v1
- Peer reviewed and published scientific report.
Hernandez, Matthew M., Ana S. Gonzalez-Reiche, Hala Alshammary, Shelcie Fabre, Zenab Khan, Adriana van De Guchte, Ajay Obla, et al. 2021. “Molecular Evidence of SARS-CoV-2 in New York before the First Pandemic Wave.” Nature Communications 12 (1): 3463. https://doi.org/10.1038/s41467-021-23688-7. https://www.nature.com/articles/s41467-021-23688-7.