People who get the shingles vaccine may have a lower risk of being diagnosed and hospitalized with coronavirus disease 2019 (COVID-19), according to a new medRxiv* preprint study. In about 150,000 people over the age of 50, vaccination for shingles was associated with a 32% reduced risk of severe COVID-19 infection.
The study results are correlational, and more research is needed to identify whether it is the shingles vaccine itself or other factors driving the lowered risk of COVID-19.
The researchers suggest the shingles vaccine may boost innate immunity — increasing the body’s cytokine levels and prepping an antiviral response against potential infections. In addition, innate immunity may help weaken severe acute respiratory syndrome coronavirus 2’s (SARS-CoV-2) ability to replicate during early infection.
Alternatively, people who are vaccinated for shingles may already be health-conscious and more proactive in getting vaccinated.
The COVID-19 vaccines continue to be the best form of protection against SARS-CoV-2.
Demographic information of vaccinated versus unvaccinated individuals
About 149,244 people were vaccinated with at least one dose of the recombinant adjuvanted zoster vaccine. A control group consisted of 298,488 unvaccinated individuals for comparison. About 16.2% of individuals were 50 to 59 years old, and 12.8% were over 80.
There were 57.8% of female participants, with over half describing themselves as non-Hispanic White.
Vaccinated individuals were more likely to have frequent outpatient medical visits before the pandemic and were associated with hypertension and having other vaccinations.
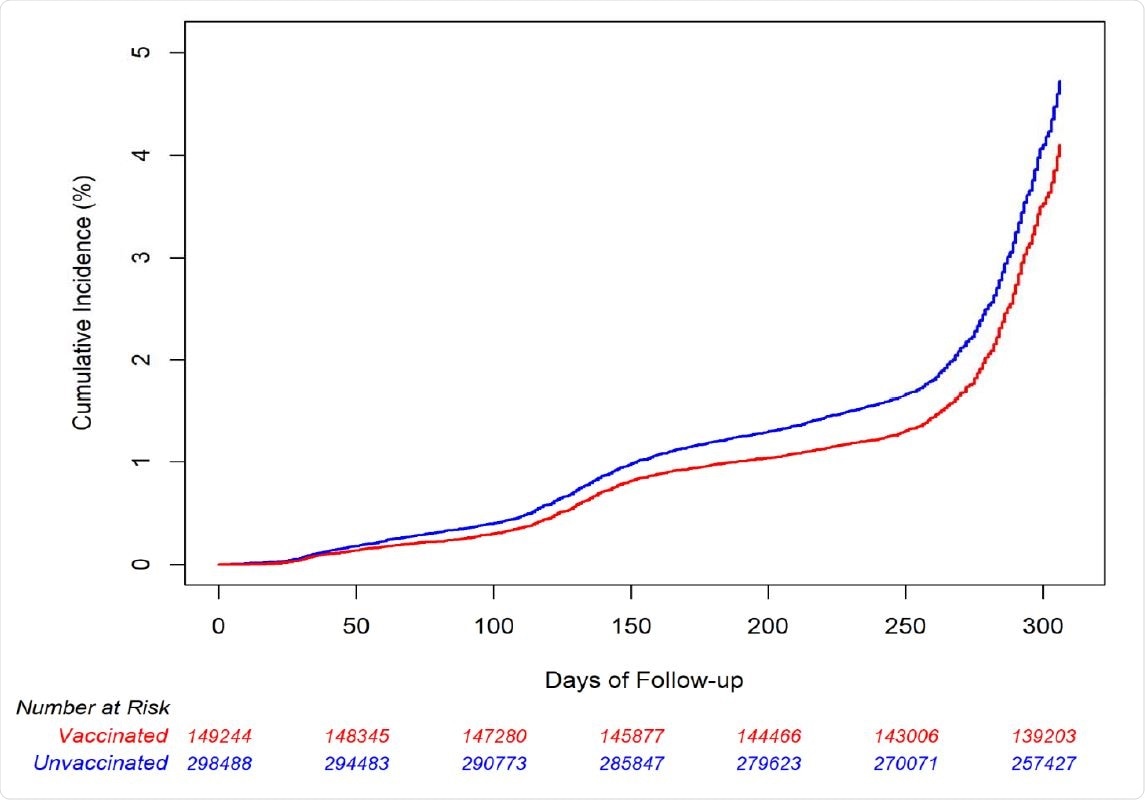
Cumulative incidence estimates of COVID-19 diagnosis by RZV (at least 1 dose) vaccination status
One dose of a shingles vaccine correlates with fewer COVID-19 diagnoses and hospitalization
Of the approximate 150,000 vaccinated individuals, there were 5,951 COVID-19 diagnoses and 1,066 COVID-19 related hospitalizations.
Individuals not vaccinated with at least one shingles vaccine dose reported more COVID-19 diagnoses. As a result, there were 13,028 COVID-19 cases, and 2,765 individuals required hospitalization for severe COVID-19 infection.
An additional analysis further confirmed lower incidences of COVID-19 and COVID-19 related hospitalization in vaccinated versus unvaccinated individuals.
One dose of the shingles vaccine correlated with a 16% reduced risk of a COVID-19 diagnosis. An association was also found between the shingles vaccine and a 32% lower rate for COVID-19 related hospitalization.
Two-dose vaccination for shingles is associated with a greater reduction in COVID-19 hospitalizations
Of the 94,895 individuals with two doses of the shingles vaccine, 3,403 were diagnosed with COVID-19 infection. Of those, 612 required hospitalization.
A cohort of 189,790 unvaccinated individuals was matched to individuals who received two vaccine doses. This group had 7,689 COVID-19 diagnoses and 1,676 COVID-19 related hospitalizations.
Results translated to a 19% reduced risk of COVID-19 infection in vaccinated individuals and a 36% reduced hospitalization rate.
Study limitations
Demographic and clinical data on individuals enrolled in the study was incomplete for several individuals. Some people failed to report BMI and smoking status, as these factors could increase a person’s risk of developing severe COVID-19 symptoms.
With any observational study, certain confounds cannot be controlled for in the study, including but not limited to health history, healthcare-seeking behavior, and more. However, the researchers attempted to minimize confounding effects by matching and comparing vaccinated individuals with unvaccinated individuals with shared attributes such as age, sex, race/ethnicity, zip code, and vaccination history.
“While this epidemiological study provides further evidence of the concept of trained innate immunity using the adjuvanted RZV vaccine, additional research is needed to identify and understand the underlying non-specific effects of RZV and other vaccines,” concludes the research team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Bruxvoort KJ, et al. (2021). Recombinant adjuvanted zoster vaccine and reduced risk of COVID-19 diagnosis and hospitalization in older adults. medRxiv. doi: https://doi.org/10.1101/2021.10.01.21264400, https://www.medrxiv.org/content/10.1101/2021.10.01.21264400v1
- Peer reviewed and published scientific report.
Bruxvoort, Katia J, Bradley Ackerson, Lina S Sy, Amit Bhavsar, Hung Fu Tseng, Ana Florea, Yi Luo, et al. 2021. “Recombinant Adjuvanted Zoster Vaccine and Reduced Risk of Coronavirus Disease 2019 Diagnosis and Hospitalization in Older Adults.” The Journal of Infectious Diseases 225 (11): 1915–22. https://doi.org/10.1093/infdis/jiab633. https://academic.oup.com/jid/article/225/11/1915/6486498.