In recent decades, the life expectancy of people with HIV has greatly improved, leading to an evolution in their needs and priorities. Now, a new definition of long-term success (LTS) in HIV care is needed to help address the multifaceted needs of all people with HIV.
NewsMedical spoke to Lisa Sterman, Global Executive Director, Global HIV Medical Affairs, Gilead Sciences, about the recently published LTS framework, recently highlighted at the opening ceremony of the 19th European AIDS Conference, which takes a person-centric approach to the HIV treatment journey.1,2 From reducing HIV-related stigma to better long-term integration of treatment and holistic care of comorbidities and mental health into people’s lives, the LTS framework aims to shift the focus from surviving to thriving with HIV
How did the LTS framework come about?
Since HIV was first identified in the 1980s, there has been a huge effort in finding effective treatments to reduce mortality and slow transmission.
Today, the efficacy of HIV medication (for those who have access and can take them) has meant that HIV viral suppression and survival are no longer the primary goals for people with HIV. There is now a significant focus on well-being and health-related quality of life (HRQoL), which considers aspects of physical, mental, and social health. As people with HIV enjoy longer lifespans, their expectations of partnering with their HIV care providers have changed.
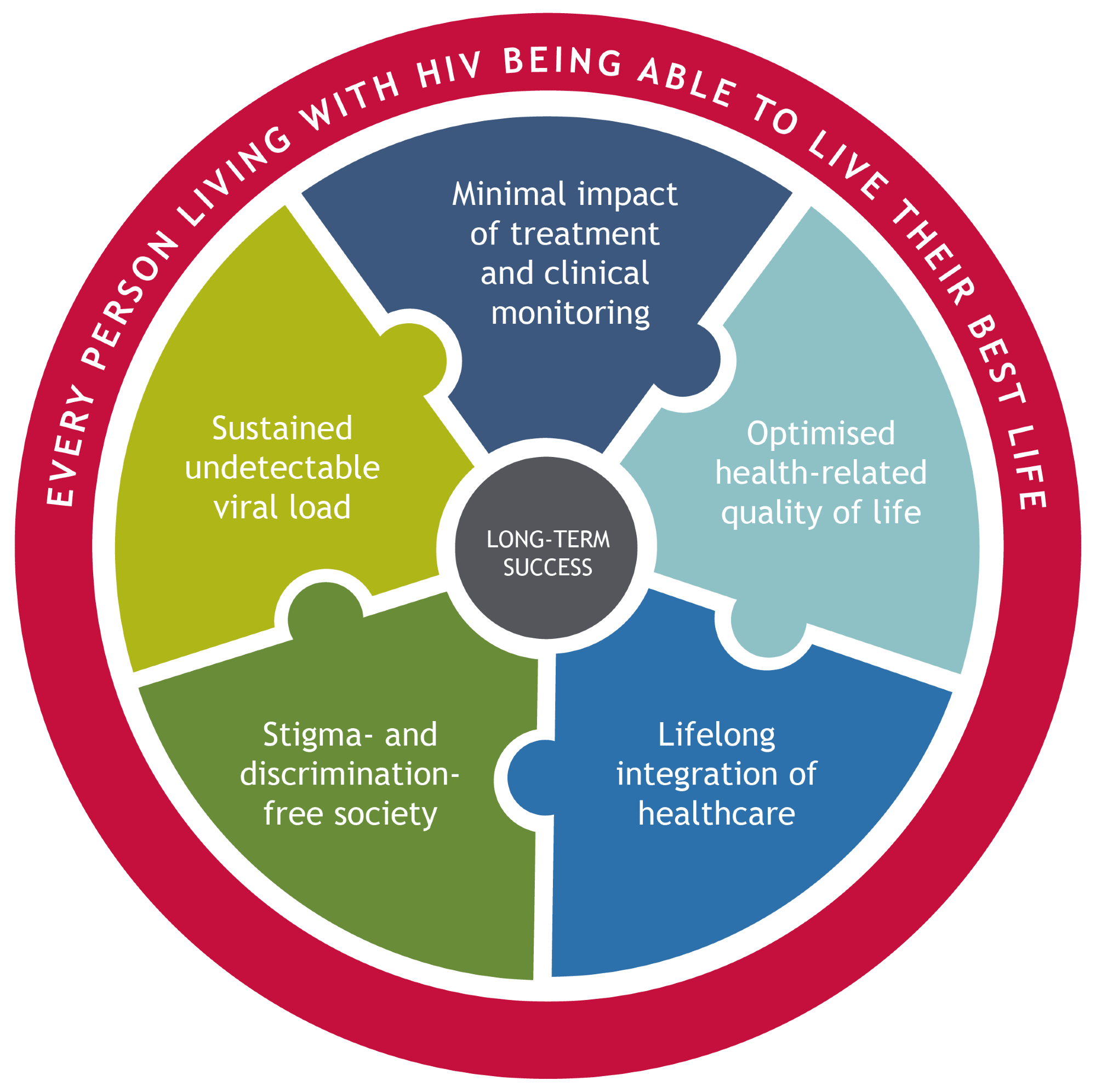
Image Credit: Gilead Sciences, Inc.
It's become apparent that the way we approach HIV care needs to evolve to meet these changing goals. That’s why Gilead collaborated directly with people with HIV, global healthcare experts, and healthcare professionals (HCPs) to help redefine LTS and craft a new, person-centric framework that can deliver LTS in HIV care. This framework includes five key outcome pillars which represent the modern reality of HIV management. In addition to viral suppression, factors such as reducing HIV-related stigma and the integration of healthcare and HRQoL across an individual’s lifespan are now equally important in the conversation.
What are the five key outcome pillars?
The five pillars that form the foundation of this new framework are sustained undetectable viral load, the minimal impact of treatment and clinical monitoring, optimized HRQoL, lifelong integration of healthcare, and freedom from stigma and discrimination.
All these pillars share a mutual goal: to improve the overall QoL for people with HIV. Ensuring that an undetectable viral load is an achievable and realistic aim remains an essential factor in long-term HIV care; however, this framework also acknowledges the impact that treatment and clinical monitoring can have on people’s lives and discusses ways in which that impact can be minimized to accommodate their needs. The topic of optimized HRQoL and how this is measured is also considered, as well as how lifelong integration of healthcare can be key to improving the HIV care journey. It is also important to address the stigma and discrimination that still, unfortunately, exists within this area by creating safe spaces to discuss personal as well as structural impact and barriers to delivering optimal care.
By addressing all these factors, and looking at the framework holistically, it is hoped that we can create an environment where people with HIV feel empowered and supported and are able to live their best lives.
There is still a lot of stigma around HIV compared with other chronic conditions. Why is this?
The stigma associated with HIV is complex and multifaceted. This discrimination first took root many years ago, when the first instances of the condition were reported among gay, bisexual, and other men who have sex with men, as well as in people who inject drugs. Society and healthcare systems in many countries did not have socially and culturally sensitive approaches to these populations at that time. Even today, with social and humanitarian advances, there remains considerable misunderstanding of HIV and who is most vulnerable to infection. Sadly, this can mean people with HIV are uncomfortable talking about their HIV status or are worried about feeling judged by their friends, families, communities, or HCPs. This internalized stigma can lead to a reluctance to talk to HCPs or seek treatment. Further, and perhaps more concerning, is the ongoing external stigma due to historic fearmongering, misunderstanding of the condition, and ongoing prejudices towards certain communities, which are all barriers to optimizing care.

Image Credit: Rawpixel.com/Shutterstock.com
How can we reduce this stigma and normalize discussions about HIV?
We can start by normalizing conversations around HIV as we have with other health conditions, such as diabetes, high blood pressure, or even more recently, COVID-19. Discussions about HIV can and should be integrated into more healthcare visits, going beyond those who may be perceived as “vulnerable” to encompass broader populations and held openly and without prejudice, as in other health conditions.
This begins with educating and training everyone involved in the care journey. This has been shown to work — interventions aimed at educating HCPs about HIV have shown positive results in reducing stigmatizing attitudes and behaviors among HCPs and staff in a clinical setting.3,4
We also cannot underestimate the role that communities play in reducing stigma. We must ensure that there are de-medicalized environments and social settings where discussions about HIV are open and honest so people can feel free to talk about their experiences within their communities, whether it is at their local hair salon or with their community leaders. It is so important that there is a wider understanding of what living with HIV really means today and that it is accepted like any other medical condition.
This de-stigmatization of HIV is also central to improving the mental health of people with HIV, as mental health challenges can stem from societal pressures as well as internalized self-judgments. Creating spaces where open and honest conversations can be freely held, whether between friends and family or with HCPs, can help build trust and lighten the burden for everyone, ultimately improving mental as well as physical wellbeing.
Reducing stigma and improving mental health are factors in boosting HRQoL. What are the other factors, and how can we implement them?
For the foreseeable future, being engaged in HIV treatment is a lifelong endeavor and has unavoidable impacts on the lives of those living with and those affected by the virus. People from remote rural areas and with socioeconomic challenges can be more heavily impacted and find it difficult to access quality care. Adapting HIV care services, whether through greater use of telehealth and e-visits or lengthening times between consultations to reduce travel time, or aiding local community support services providing health checks, counseling, and specialist referrals to facilitate quality care.

Image Credit: Yuganov Konstantin/Shutterstock.com
Additionally, better integration of care, facilitated by seamless communication between multidisciplinary care teams, can offer people more consistency and control over their care. This can also have a significant impact on improving HRQoL.
But how do we measure HRQoL, especially when everyone has different needs and priorities? There are patient-reported outcome measures (PROMs) developed specifically for use in HIV care that can help identify particular cultural and demographic needs, providing tailored goals for improving people’s experience. Indeed, using reported PROMs has been shown to empower people with HIV and improve individual–HCP interaction.5
You mentioned that the LTS framework was person-centric. What does this mean? How is it different to a holistic approach?
In holistic care, an individual’s physical, psychological, spiritual, and emotional needs are treated as part of a “whole system” approach, creating an overall picture of a person’s care.
Person-centric care, on the other hand, takes a more individualistic approach to care, with HCPs focusing on the differing needs of the individual and what their specific priorities and healthcare goals might be. It also extends beyond the boundaries of medical care to look at other factors, such as the long-term quality of an individual’s life and how their treatment (not just for HIV but for any other concomitant conditions) can be comfortably integrated into their lifestyle.
Ultimately, a person-centric approach means being sensitive to individual needs and ensuring that attention is focused more on the individual person instead of the virus. The treatment journey should be a personal, supportive, and empowering one for each individual person.
How does this person-centric approach to HIV care address unmet needs?
When people are treated as individuals, their trust in the care system can grow, empowering them to make informed decisions about their treatment needs and desires more openly and uncovering any barriers to optimal care. This forms the basis for successful shared decision-making, where people can work seamlessly with their HCPs and healthcare communities to co-create a management plan that works best for them.
How do you envision the LTS framework influencing the future of HIV care?
We are standing at the edge of a technological and social–cultural shift in HIV care, both in medicine and society, that will continue to improve the lives of people with HIV.
Medicine is consistently looking towards the inspiration that drives innovation. In this case, I believe this new framework will open doors to informing the importance of treatment selection for long-term success among current options and the future innovations needed to best support people with HIV – essentially a vital compass for our research efforts.

Image Credit: PENpicks Studio/Shutterstock.com
Society, in general, may move more slowly towards change, so it is the responsibility of the healthcare field to reject the stigma and discrimination that has previously been directed toward the people we serve — people with HIV and those who would benefit from HIV prevention efforts. Allowing all people, regardless of their medical condition, or social or cultural impacts, to live healthy, dignified, and full lives will take thoughtful commitment on our part as both healthcare providers and members of society. However, I am optimistic that this new framework is a significant step towards empowering people with HIV to live their best lives. This is a pivotal moment, but it is just the beginning; we must continue to listen, learn, and adapt and evolve the framework to truly create a future of HIV care that works best for all.
Dr. Lisa Sterman
Dr. Lisa Sterman began her career in HIV as a volunteer on San Francisco General Hospital’s infamous AIDS Unit, Ward 5A, in 1987. She received her BA and MPH from University of California, Berkeley, and MD from Emory University. During her career, she worked to help set up the first HIV data base at the Veteran’s Administration in San Francisco from 1988-1990 and worked in private practice as an HIV specialist and Internist and teaching faculty in San Francisco from 1997-2021.
She has authored and co-authored many articles in the professional and lay press on HIV topics, having been a national and international lecturer on HIV and HIV prevention topics and served on the Board of Directors for the San Francisco AIDS Foundation from 2011-2017, currently serving on the organization’s Community Board of Directors. Dr. Sterman joined Gilead Sciences in June, 2021 as Global Executive Director of HIV prevention for Medical Affairs. She is committed to ending the HIV epidemic for everyone, everywhere.
About Gilead Sciences, Inc.
Gilead Sciences, Inc. is a biopharmaceutical company that has pursued and achieved breakthroughs in medicine for more than three decades, with the goal of creating a healthier world for all people. The company is committed to advancing innovative medicines to prevent and treat life-threatening diseases, including HIV, viral hepatitis, COVID-19, and cancer. Gilead operates in more than 35 countries worldwide, with headquarters in Foster City, California.
For more than 30 years, Gilead has been a leading innovator in the field of HIV, driving advances in treatment, prevention, testing and linkage to care, and cure research. Today, millions of people living with HIV globally receive antiretroviral therapy provided by Gilead or one of the company’s manufacturing partners.

References:
- Lazarus JV, Wohl DA, Cascio M, et al. Long-term success for people with HIV: A framework to guide practice. HIV Med. 2023;24(Suppl. 2):8–19.
- Fuster-RuizdeApodaca MJ, Wohl DA, Cascio M, et al. Why we need to re-define long-term success for people living with HIV. HIV Med. 2023;24(Suppl. 2):3-7. doi:10.1111/hiv.13461
- Machowska A, Bamboria BL, Bercan C, et al. Impact of 'HIV-related stigma-reduction workshops' on knowledge and attitude of healthcare providers and students in Central India: a pre-test and post-test intervention study. BMJ Open 2020;10:e033612.
- Shah SM, Heylen E, Srinivasan K, et al. Reducing HIV stigma among nursing students: a brief intervention. West J Nurs Res 2014;36:1323–1337.
- Bristowe K, Murtagh FEM, Clift P, et al. The development and cognitive testing of the positive outcomes HIV PROM: a brief novel patient-reported outcome measure for adults living with HIV. Health Qual Life Outcomes 2020;18:214.