Sleep requirements change throughout life. As part of normal aging, sleep generally becomes briefer and fragmented, with older people often having multiple naps throughout the day. This may not be the pattern of sleep seen in patients with Alzheimer’s disease and other neurodegenerative conditions, however.
Lack of Sleep and Beta-Amyloid
Recent studies have shown that lack of sleep, for even one night, can significantly increase levels of beta-amyloid in the brain – one of the main toxic proteins that are linked to Alzheimer’s disease.
During sleep, the brain uses its own glymphatic system (the brain’s own drainage system) to wash out excessive levels of beta-amyloid and other metabolites that accumulate. This clearance rate is doubled in sleep compared to wakefulness, and is accelerated by the larger interstitial space in the brain during sleep. However, during sleeplessness and lack of overall sleep (even as little as one night), the brain is not able to clear out beta-amyloid levels effectively, and thus levels can build up over time.
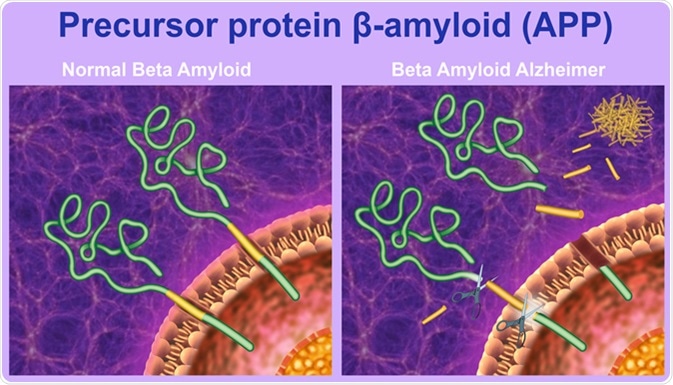
The proteolytic processing of the precursor protein beta-amyloid. Image Credit: Ilusmedical / Shutterstock
Furthermore, the elevations in beta-amyloid were shown to be accentuated in areas that are damaged in early Alzheimer’s pathology, such as the hippocampus and the thalamus (involved in memory, for example). Those who were sleep-deprived the most (who had the highest increases in beta-amyloid in the thalamus) also often experienced worse moods.
Some chronic sleep disorders can also increase the risk of Alzheimer’s disease. Obstructive sleep apnoea (OSA) is a strong risk factor for dementia, both vascular dementia and Alzheimer’s disease. A majority of patients with OSA are usually overweight and obese, and these may be risk factors common to both OSA and Alzheimer’s. However, studies have shown a marked increase in beta-amyloid levels in the brains of patients with OSA compared to those who do not have this condition, despite being overweight.
Sleep deprivation in early life may therefore be an important risk factor in the development of Alzheimer’s disease later in life. Therefore, people suffering from insomnia should seek medical advice as soon as possible in order to delay or lower the amyloid burden in the brain.
Sleep Disturbances in Alzheimer’s Disease
Most patients with Alzheimer’s develop sleep problems which worsen as the disease progresses. Some common sleep disturbances seen in patients with Alzheimer’s are:
- Loss of the ability to stay asleep, despite being able to get to sleep
- Increased sleep latency (duration required to get to sleep is longer)
- Increased agitation before bedtime and throughout the night
- Disorientation upon waking up (in the night, or in the morning)
- Sleepy during the day, whilst being alert during the night (circadian abnormalities)
- Periodic limb movement (PLM) is worsened in around 50% of Alzheimer’s patients
- Shorter duration of both slow-wave-sleep (SWS) and rapid-eye movement sleep (REM) despite the total number of sleep cycles remaining unchanged
It is important to note that not all large-scale studies have shown a significant correlation between sleep disruption and Alzheimer’s disease, either in the pre-clinical stage or after symptoms develop. Therefore, not all Alzheimer’s patients suffer from sleep problems, and likewise, not all people suffering from sleep issues in older age necessarily have Alzheimer’s. However, many studies have shown that sleep ability and quality is indeed disrupted in a vast number of cases of Alzheimer’s compared to healthy age-matched controls.
Sleep loss may contribute to Alzheimer's
It is now increasingly accepted that sleep loss may indeed be an important risk factor and symptom of Alzheimer’s disease. However, whether sleep loss contributes to Alzheimer’s progression, or whether Alzheimer’s causes sleep problems, is yet to be determined.
Further Reading
Last Updated: Jun 28, 2019