The most common symptom of pericarditis is chest pain, and this is something with which most patients present themselves at a clinic.
Diagnosis and confirmation of pericarditis happens in a series of steps: knowing the medical history of the patient, medical examination, recommendation of tests, and confirmation based on the test results.
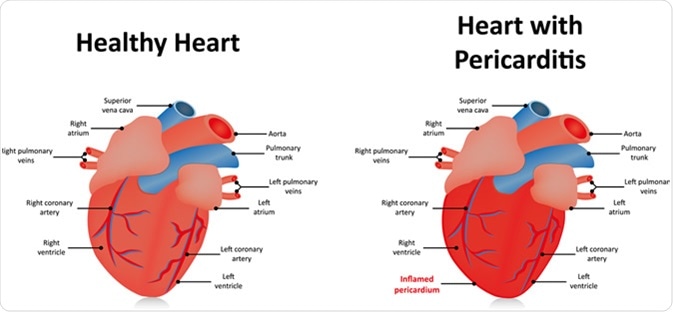
Pericarditis. Image Credit: Joshya / Shutterstock
Medical History
If records of the medical history of a patient are available, these are carefully noted. The attending doctor asks a series of questions to learn the medical background of the patient. Questions that are routinely asked include the following:
- Whether the patient had a fever or any other illness recently;
- Whether the patient had (or had received treatment for) any kind of infection in the recent past;
- Whether the patient had ever suffered myocardial infarction (heart attack);
- Whether the patient had any form of injury in the chest region;
- Whether the patient had any other medical condition that may be (even remotely) connected to the current pain experienced;
- Whether the pain increases or decreases with change in position (for example, a decrease in pain while in a sitting position).
Answers to questions such as these can often give a clue as to whether pericarditis could be the cause of the chest pain.
Physical Examination
When a patient has chest pain, the doctor quite naturally checks the chest of the patient with a stethoscope to listen for the sounds arising from the heart region. The pericardial rub is a specific sound caused by the rubbing of the pericardium against the outer layer of the heart. The doctor may be able to distinguish this from other sounds within the chest cavity.
This, again, can only be taken as another clue that may point to pericarditis.
Pericardial Effusion - Mayo Clinic
Diagnostic Tests
The following are some of the tests recommended by a doctor, the details being governed by the specifics of the patient under consideration.
Electrocardiography (ECG): A careful electrographic study of the patient’s heart will help in differentiating pericarditis from myocardial infarction. It is quite important that myocardial infarction be ruled out, as its treatment is quite different from that of pericarditis. During this test, the electrodes in the ECG are placed on the chest skin for measuring the electrical function of the heart. Distinctive changes in the electrical activity of the heart can be easily detected by the ECG in people with pericarditis.
Chest X-ray: This is a type of radiation test. If the patient has pericardial effusion, the volume of the pericardial fluid within the pericardial cavity may be quite high. In this case the X-rays are passed through the body and the energy that comes from the rays is absorbed by the different parts of the body at different rates. The rays picked up by the body are converted into an image using a detector, so that one can see the affected part (here an enlarged heart). If the patient has a constrictive type of pericarditis, this may show up as some kind of calcification around the heart region.
Doppler electrocardiography: This is also known as Echocardiogram or Transthoracic echocardiogram (TTE). This test uses high-frequency sound waves to create composite pictures of the patient’s heart, indicating its size, shape, and functioning. Such images help the doctor to diagnose complications of pericarditis, such as large effusions, cardiac tamponade, or constrictive pericarditis. Two-dimensional echocardiography is said to be the diagnosis of choice for such medical conditions.
Cardiac CT: A computed tomography (CT) scan uses X-rays to create detailed images of any part of the body. These can produce more detailed images of a patient’s heart than conventional X-rays; however, a CT scan is not recommended unless a person shows some symptoms (gathered from the earlier tests). It is used to rule out other medical conditions, including pulmonary embolus (clot in the lung) or aortic dissection (tearing of the aorta). The cardiac CT scan is also used to confirm the thickening of the pericardium due to constrictive pericarditis.
How a 5 minute Heart CT can Help Predict a Heart Attack
Cardiac MRI: Magnetic resonance imaging (MRI) is a sophisticated technique that uses a magnetic field and radio waves to create various sectional images of any part of the body. A cardiac MRI would provide cross-sectional images of the patient’s heart at various points, and can reveal changes in the pericardium such as effusion, thickening, or inflammation.
Laboratory blood tests: A variety of blood tests, such as general complete blood count (CBC), erythrocyte sedimentation rate (ESR), or specific cardiac enzyme tests or levels of specific serum components, may provide further clarifications (serum troponin test) or may complement the findings for the tests mentioned earlier.
In some cases, a needle helps to drain any fluid around the heart, so that the fluid can be tested to confirm the disease.
Together, all of these, help in the confirmation of the specific type of pericarditis, after which a treatment regimen may be worked out for individual patients.
Further Reading
Last Updated: Dec 29, 2022