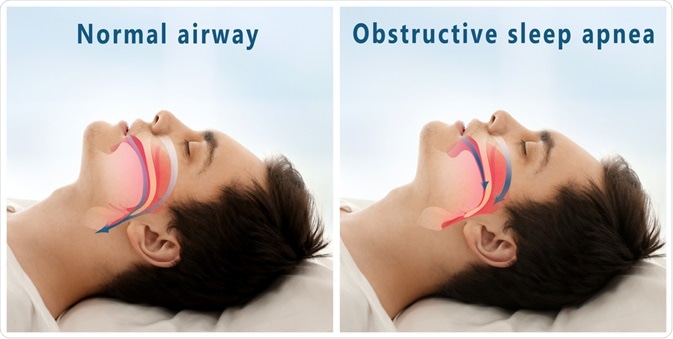
Obstructive sleep apnea (OSA) is a condition in which anatomic and neuromuscular factors interact to cause the pharyngeal airway to periodically collapse during sleep, leading to frequent awakenings, shallow breathing and irregular suspensions of breathing.
 Africa Studio | Shutterstock
Africa Studio | Shutterstock
OSA is associated with multiple adverse long-term health impacts, such as stroke, hypertension, and diabetes, besides depression and daytime sleepiness.
Treating sleep apnea
Classic treatments for OSA include weight loss, behavioral modifications, the use of a device to forcibly keep the jaw closed called a mandibular advancement device (MAD), the continuous positive airway pressure (CPAP) device, and maxillofacial surgery.
Some studies show that the tone of the genioglossus muscle which dilates the pharynx is higher in OSA patients during wakeful periods than in normal non-OSA controls. This may be caused by a dysfunctional neuromuscular condition following injury, due to hypoxia, systemic inflammation, or even heavy vibration during snoring.
When a non-OSA individual sleeps, the genioglossus activity on electromyography increases in a predictable way compared to the negative pressure inside the pharyngeal lumen. This is not the case with OSA patients. This deficit may be why Hypoglossal Nerve Stimulation (HGNS) appears to work to mitigate OSA.
In patients for whom CPAP is not feasible (e.g. due to intolerable side effects like high noise levels, airway pressure, mask-induced irritation, and mouth dryness), surgical treatment is often performed. Unfortunately, surgical results are not consistent, and many patients are not willing to have major maxillofacial surgery. This has encouraged the growth of neuromodulation device use.
In such situations, HGNS may be prescribed. A surprisingly high percentage (>40%) of patients with OSA do refuse to continue using CPAP. Many of them remove the mask at some point during their sleep, which increases their risk of sleep apnea and hypoxia. However, a high percentage of former CPAP users who could not tolerate the device are able to use neuromodulation devices.
Principles of HGNS
HGNS is an innovative treatment for OSA which uses neuromodulation via an implantable stimulatory device, resembling a pacemaker, which promotes airway patency throughout the night sleep and thus improves sleep in OSA patients.
The system consists of a sensor to detect alterations in the breathing pattern, with a lead that stimulates the hypoglossal nerve to activate the genioglossus muscle and thus open the pharyngeal airway. The stimulator is battery-powered and the system is controlled by a patch, either wearable or remote.
The HGNS system is designed to sense the pattern of breathing and whenever a collapse of the airway occurs, it is detected by a corresponding increase in the effort of breathing. The sensor may be worn at some point over or between the ribs for this purpose.
The detection of an OSA event is followed by the delivery of a mild stimulus to the tongue and the throat which promotes genioglossus stimulation, keeping the airway open. Clinical testing of an HGNS device has shown that it can reduce the apnea-hypopnea index (AHI) significantly, which is the chief marker of the severity of OSA. As a result, it reduces the incidence of oxygen desaturation and interruption of breathing.
Benefits of HGNS
Neuromodulation is a successful and safe way to improve the sleep patterns of patients with OSA and their spouses. In contrast to the high rate of CPAP intolerance, devices that offer HGNS are still in use after 12 months in 86 percent of patients, and 84% at 18 months.
HGNS is a form of treatment which can be titrated up or down, according to changes in the patient’s weight, age-related reduction in elasticity of the soft tissues, and other chronic changes. It is also capable of preventing airway collapse at multiple levels with just a single implant, because it stimulates tongue protrusion, alleviating antero-posterior collapse, but also retropalatal collapse is prevented as it keeps the muscle tone high, rather than allowing them to become limp during sleep.
Adverse effects
HGNS has no serious negative effects, with no reports of implant removal or anything more than temporary trauma to the hypoglossal nerve. It causes little discomfort after implant, especially when compared to the major sculpting of soft tissue and bone around the pharynx that is otherwise undertaken.
Minor issues that have been repored include stiffness and small cuts on the tongue, transient weakness of the tongue, some swelling after the implant, but most can be reduced still further by good surgical technique and careful stimulation settings, along with adjustments to the teeth and mouth guard use.
Neuromodulation devices offering HGNS are not suitable for obese patients, and are quite expensive. After their implant the patient cannot have an MRI scan taken, and they are relatively large in size.
Drug-induced sleep endoscopy (DISE) is mandatory before HGNS, as it does not work well with complete concentric collapse (CCC) patterns of OSA. DISE is however a costly procedure. HGNS and other neuromodulation procedures are also more expensive than CPAP, and current recommendations are to reserve it as a second-line option in patients who cannot be treated by other conventional OSA therapies.
Further Reading
Last Updated: Jan 15, 2019