Keratoacanthoma is an abnormal growth on the surface of the skin. It is a small lesion that has a hard center, filled with the protein keratin. The little bump on the skin is flesh-colored and dome-shaped. It usually originates in the hair follicle and is considered a subtype of well-differentiated squamous cell carcinoma.
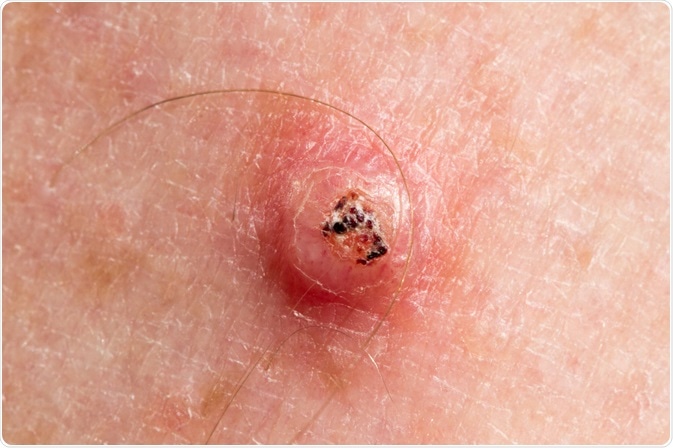
Image Credit: Peter Mullineux / Shutterstock.com
The skin condition of keratoacanthoma is mostly found in adults who have been exposed to the sun’s ultraviolet (UV) radiation on a frequent basis. The epidermal neoplasms generally occur on the exposed portions of the face, the hands, arms, torso, and legs. The skin damage caused by the sun’s rays is a factor in precipitating the condition.
Progress of keratoacanthoma
The skin will develop a small bump of 1-2 millimeters (mm) in size initially. The flesh-colored bump will then begin to expand over the next 6 to 8 weeks. It will resemble a dome shape and have a central core of hard keratin that pushes against the skin, drawing it taut. Once it has grown to its maximum size of 1-3 centimeters (cm), the bump becomes dormant and does not change for nearly 2 to 6 weeks.
Even if no treatment is carried out, the bump will begin to spontaneously heal within 2 to 12 months. The hard center of keratin will fall out as the skin that is stretched tight over it will thin out and break. The sides of the bump, which will look like a volcanic crater, will regress gradually. Eventually, the lesion will heal and flatten out completely. It will leave behind a scar at the location of the bump.
Diagnosis of keratoacanthoma
The diagnosis of keratoacanthoma is often difficult, as this lesion resembles numerous other skin conditions. The removal of the lesion is recommended, as the bump on the skin could also be squamous cell carcinoma (SCC). SCC is a much more aggressive form of skin cancer that can cause major disfigurement; therefore, it should not be left undetected.
As keratoacanthoma closely resembles this more dangerous illness, a biopsy is advised to ensure that there is no other danger to the health of the patient. There are many regional variations in the diagnosis of keratoacanthomas and SCC, as it is difficult to differentiate them even at a microscopic level.
Treatment of keratoacanthoma
The removal of the skin lesion is considered a complete treatment for keratoacanthomas if the dermatologist successfully removes the entire affected tissue. This removal can be done via excision, curettage and cautery, cryotherapy, or radiotherapy,
Excision
An excision involves cutting away the keratoacanthoma with a surgical instrument. The affected tissue is cut and the wound left behind is stitched up for faster healing. Dressing the surgical wound may need to be done at regular intervals until it has healed completely, which takes about one week on average.
Curettage and cautery
Curettage and cautery is an electrosurgery procedure where the flesh-colored bump is first scraped off using a spoon-like instrument known as curettage. Following this, heat is applied to the area of the skin to avoid infection and stop the bleeding. If required, a couple of stitches may also be used. Dressing of the wound may also be done.
Cryotherapy
Skin lesions in multiple keratoacanthomata are frozen using liquid nitrogen, carbon dioxide snow, or dimethyl ether and propane. This liquid is applied with a cotton-tipped applicator, which will cause the lesions to freeze and fall off the skin. This procedure is completely safe and relatively inexpensive to use as a treatment for keratoacanthoma.
Radiotherapy
While not usually recommended for a single lesion, should the patient be suffering from multiple keratoacanthomas, radiation may be suggested. Radiation in small bursts is applied to the targeted cancerous tissue. The energy that is transmitted destroys the cancerous cells. The strength of radiation used will differ on an individual basis.
Management of keratoacanthoma
The individual who develops keratoacanthoma once is at higher risk of developing it again. It is also likely to occur as multiple keratoacanthomata the second time, which is why the individual must regularly keep checking their skin for bumps. Patients can also reduce their probability of developing future keratoacanthomas by protecting their skin from sun damage and avoiding chemical carcinogens such as tobacco and cigarettes.
While there is no direct evidence to support the fact that keratoacanthoma is a genetic illness, it has been found to run in families. Multiple keratoacanthomas are much more likely to be found in family members related by blood, which is why family medical history must also be shared with the health care provider. There is no underlying factor that causes the skin lesion; therefore, it is difficult to predict who will be afflicted by this condition.
References
- http://www.aocd.org/?page=Keratoacanthoma
- http://www.bad.org.uk/shared/get-file.ashx?id=96&itemtype=document
- http://www.dovemed.com/diseases-conditions/keratoacanthoma/
- http://www.pathologyoutlines.com/topic/skintumornonmelanocytickeratoacanthoma.html
- https://patient.info/doctor/keratoacanthoma-pro
Further Reading
Last Updated: Apr 21, 2021