Injuries to the maxillofacial region are fairly common in emergency medicine. This area is of particular importance, because it is dangerously close to the most important organ in the body – the brain. Moreover, the maxillofacial expanse, or put simply, our face, is one of the most imperative elements in our everyday psychosocial wellbeing.
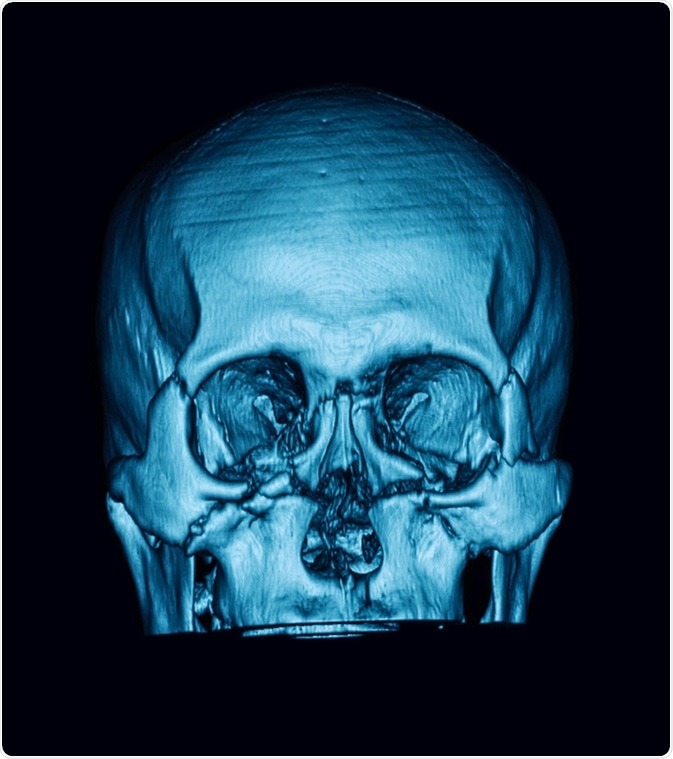
Computed tomography (3DCT scan) of facial bone, showing multiple maxillofacial fractures. Image Credit: Suttha Burawonk /Shutterstock
Any impairment in this region could have devastating psychological impacts. It may be colloquially referred to as the ‘organ of emotion’ and captures our ability to provide social cues that are essential for our survival in a society that is heavily dependent on our abilities to communicate with one another.
The maxillofacial region may be divided into three parts of fairly equal proportions – the upper, mid and lower face. It is home to an array of motor-sensory systems that are imperative for functions, such as vision, olfaction and audition, as well as vestibular, somatosensory, and gustatory purposes. Not only does it house these critical functions, but also it is intimately associated with some very vital structures that are present in the head and neck. These include the upper parts of our respiratory and digestive systems as well as a plethora of neurovascular bundles.
Etiopathogenesis
Depending on locale, the etiology of these types of injuries may vary. The most common cause of maxillofacial injuries in countries categorized as ‘developing’ is motor vehicle accident (MVA). In contrast, ‘developed’ countries report violent assault as the most common cause, which is then followed by MVA. Falls and accidents during other activities, such as skiing, cycling and skating, are also part of the etiology. These injuries can be classified as soft tissue if, for instance, only the skin is involved. On the other hand, they are regarded as bony if fractures are involved, or special if structures such as the eyes and facial nerves are involved.
In order for a maxillofacial injury to occur, force in the form of kinetic energy is required. The severity of the injury is directly proportional to the amount of force applied. However, different parts of the maxillofacial expanse may require different amounts of force in order for an impact to cause resultant injury. Areas such as the mandible, maxilla and supraorbital rim are more resistant to forces and as such require higher energy impacts before damage can occur. Contrariwise, lower energy forces easily damage the bones of the nasal bridge or zygomatic arch.
Clinical Presentation
The clinical presentation is largely dependent on exactly where in the maxillofacial region the injury has occurred. The upper face encompasses the area between the hairline and the glabella (i.e. the prominence located between the eyebrows). The structures that can be damaged in this zone of the face are the frontal bone and sinus. Aside from obvious lacerations or contusions and complaints of facial pain, patients with frontal bone and/or frontal sinus fractures may present with hematoma, subcutaneous emphysema and paresthesia of the supratrochlear and supraorbital nerves. Moreover, these patients may have a visibly depressed area on the forehead.
The mid-face extends from the glabella to the bottom of the columella (i.e. the external termination of the nasal septum). Structures in this region that can be damaged include the bones of the orbit, nose and maxilla, as well as the zygomaticomaxillary (ZMC) and nasoethmoidal (NEC) complexes. Damage to the orbital region can cause dysfunctional eye movements as well as ecchymosis, edema and crepitus. Nasal injury may present with obvious deviation and bleeding. NEC injuries characteristically may demonstrate an increased medial canthi distance between the eyelids, whereas ZMC damage may show up as malar eminence depression.
Patients with maxillary fractures may present with increased mobility between the hard palate and alveolar process of the maxilla if they have a Le Fort I fracture. Those with a Le Fort II fracture may bleed from the nose and have subconjunctival hemorrhage, while those with Le Fort III will have more severe facial edema and findings. The lower face extends from the bottom of the columella to the base of the chin and structures of interest in this area are the mandible and dentoalveolar divisions. These patients may present with pain in the jaw and malocclusion.
Management
The advanced trauma life support (ATLS) protocol is followed in these patients. Airways, breathing and circulation are assessed and measures are taken to ensure that they are maintained. The patient’s mental status is then assessed with the help of the Glasgow coma scale and a neurological examination is also conducted. All areas of concern are exposed for physical exploration. The golden standard imaging modality for maxillofacial injuries is the CT scan; however, patients with low energy mandibular fractures may be initially screened with a panoramic x-ray.
In general, fluids and oxygen, as well as any blood product transfusions are given on a necessity basis. Pain is managed accordingly with analgesics and open wound fractures require treatment with a course of antibiotics, and where applicable, a tetanus shot is administered. Once the patient is stabilized and there are no urgent medical concerns, maxillofacial surgery may be done and is required in most instances. Depending on the severity of the fractures, closed or open reduction and fixation with screws and/ or plates will be necessary.
References
Further Reading
Last Updated: Feb 27, 2019