Diagnosis of obstructive sleep apnea (OSA) begins with a complete medical and sleep history and medical exam. This can include detailed questions about patterns, duration, quality of sleep; prevalence and frequency of snoring; daytime fatigue; and morning symptoms of sore throat or headache.
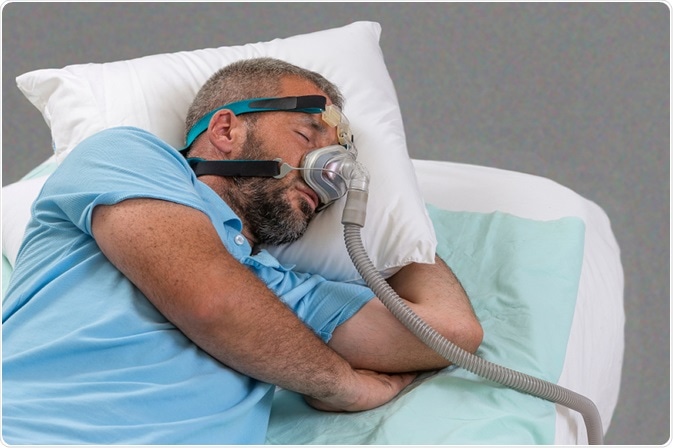
Man with sleeping apnea and CPAP machine. Image Credit: JPC-PROD / Shutterstock
Because the breathing reflex that arouses a person from sleep in order to resume proper breathing does not always awaken them to a fully conscious state, many OSA sufferers do not realize their sleep is interrupted.
In these cases, a partner or family member can provide useful information. It is also important to know if family members suffer from OSA because people with a family history are at increased risk for developing OSA. Careful evaluation of sleep history is critical in high-risk individuals such as obese or those who exhibit risk factors for cardiovascular disease and type 2 diabetes.
A medical history review is typically followed by a medical exam to identify potential anatomical causes for OSA including enlarged tonsils, adenoids, soft palate tissue, or uvula.
In some cases, a subsequent consultation with an otolaryngologist (a medical doctor specializing in the ear, nose, and throat) is necessary to rule out craniofacial abnormalities.
Polysomnography
The definitive test for diagnosing OSA is the polysomnogram, an overnight sleep test performed by a specialist in a sleep lab. Polysomnography measures breathing patterns, breathing rates, blood oxygen levels, blood pressure, and muscle and brain activity during sleep.
Throughout the test period, episodes of apnea and hypopnea are counted per hour to diagnose OSA and determine its severity.
In some cases when OSA is diagnosed quickly or is strongly suspected based on results of the medical or family history, the sleep specialist will use the second half of the testing period to study the effects of continuous positive airway pressure (CPAP) therapy, which is the primary treatment option for OSA. This is called a split-night study.
CPAP uses a close-fitting facial mask during sleep to blow air at a constant pressure into the mouth and nose in order to keep airways open. During a split-night study, the optimal CPAP airway pressure and response to therapy will be determined.
In some cases, sleep testing can be performed at home using a portable monitor. Similar to polysomnography performed in the sleep lab, a portable sleep monitor measures breathing rates, heart rates, and blood oxygen levels.
Home-based monitoring can be beneficial for patients whose access to a polysomnography facility may be limited due to budgetary restrictions or geographical location.
What to Expect | Home Sleep Apnea Testing
Although polysomnography remains the gold standard for OSA diagnosis, the US-based Centre for Medicare and Medicaid Services (CMS) concluded that home-based monitoring could effectively identify patients who would benefit from CPAP therapy.
Measuring Severity of Obstructive Sleep Apnea
The severity of OSA is determined using the apnea-hypopnea index (AHI). This severity scale evaluates sleep disruption throughout the night by measuring the number of apneas (complete pauses) and hypopneas (partial pauses) that occur per hour during sleep.
AHI scores below 5 are considered normal. A patient with an AHI score of 5-15 is considered to have mild OSA, while a score of 15-30 indicates moderate OSA. AHI scores of >30 are indicative of severe OSA.
Measuring AHI is important for guiding treatment decisions, as those with a higher AHI score may be provided with more aggressive treatment options.
AHI determination is also important for evaluating subsequent risk for cardiovascular disease and other medical complications and establishing a baseline for evaluating the effectiveness of treatment.
Further Reading
Last Updated: Feb 24, 2023