The painless condition in which a nail separates from the nail bed is referred to as Onycholysis. This can occur due to a number of factors such as injury for someone with long fingernails, or as the consequence of a skin infection. It is also possible for the nail to separate due to excessive filing or chemical treatments during manicures. The nail initially loosens before it completely separates from the nail bed.
There is little scope for it to be reattached, but if the condition clears up a fresh nail will grow from the root. The separation begins at the tip of the fingernail and works itself back towards the root. Occurrence is predominantly seen in women.
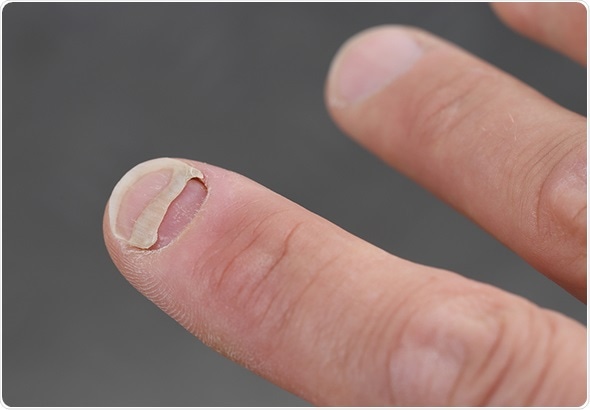
A Patient with nail detachment - Image Copyright: riopatuca via Shutterstock
Risk Factors for Onycholysis
Physical Trauma
Trauma may be caused by using blowdryers to dry nail paint. Filing the nails improperly may also loosen the nails and separate them from the nail bed with time. Tapping long nails on a keyboard or counter may also be a contributing reason for this nail condition. One would expect the deposition and lodging of debris between the lifted nail and the nail bed to results in the gradual spread of infection until the nail falls off.
Infections
People who have to spend a large portion of their day with hands immersed in water or using chemicals such as solvents and cleaners are likely to develop nail infections that could cause onycholysis. Infections can be fungal, yeast based, bacterial or viral in nature. There is no specific cause for this condition, but it can be triggered by any type of infection and affect the nails.
Drug Side Effect
A person may also develop this nail condition as a side effect of treatment drugs such as tetracyclines, psoralens, fluoroquinolone antibiotics, chlorpromazine, and even oral contraceptives. The drugs, especially if taken long term, may create an unwanted side effect on the nails by causing a loosening of the nail from the nail bed. If a secondary infection flares up in the nail bed, it can make the condition worse.
Present Diseases
If a person is suffering from an existing disease, onycholysis may be a symptom present. Skin diseases such as psoriasis, dermatitis, pemphigus vulgarism, and porphyria cutanea tarda may cause nails to degenerate in this manner. Other internal diseases such as Amyloid and multiple myeloma, anemia, diabetes mellitus, erythropoietic porphyria, hyperhidrosis, hyperthyroidism, hypothyroidism, impaired peripheral circulation, leprosy, pellagra, psoriatic arthritis, Reiter syndrome, sarcoidosis, scleroderma, and yellow nail syndrome may also show symptoms of this disorder. Some congenital or hereditary diseases may also have this effect on the nails.
Symptoms of Developing Onycholysis
The condition is quite easily visible as the nail begins to loosen from the nail bed. The pink part of the nail begins to reduce as the opaque part begins to grow from the fingertip towards the cuticle. When touched, the nail can move up away from the nail bed with ease. The nail may become white, green or yellow as the secondary infection begins to settle in under it. In some cases the skin under the edges of the nail may thicken. The nail bed itself may get deformed with dips and ridges. By the time the nail is actually ready to fall off there is very little pain if any as it separates. Pain is usually the indicator of active infection. The actual cause of the condition can vary the time it takes for the nail to come apart.
Preventing Onycholysis
Taking preliminary steps towards caring for your nails when the first signs of onycholysis show up, can help manage the condition better. Onycholysis caused by physical trauma can be avoided altogether and deterioration of the nail can be prevented even after its onset. Additional steps in the prevention of Onycholysis are as follows:
- Ideally nails should be kept short and the affected portion should be clipped away. The clipper should be used to trim the nail till the place it is reattached to the nail bed.
- The nail bed should be washed and dried regularly so as to flush out any infection that may gather in the nail bed.
- Contact with chemicals such as nail paint, solvents, detergents and enamel removers should be avoided.
- Vinyl or cotton gloves should be worn to protect the nails from deterioration if working constantly with chemical irritants.
- The cut nails should not be bandaged as bacterial infections may grow under the bandages and prove counter-productive.
- A drying agent like 3% Thymol in alcohol may also be prescribed by the treating health care practitioner and should be used each time the hands get washed.
- Medicine pills may be prescribed along with topical gels or creams to help treat the root cause of the condition. Medicines may be also required to control any secondary infection that flares up.
References
Further Reading
Last Updated: Feb 27, 2019