Trichomonas vaginalis is a flagellated protozoan responsible for urogenital trichomoniasis in humans that shows a notable prevalence around the globe. One of the most striking features of this parasite is its highly variable biological behavior, so clinical manifestations of trichomoniasis may range from the absence of symptoms (in a majority of cases) to more severe clinical presentations.
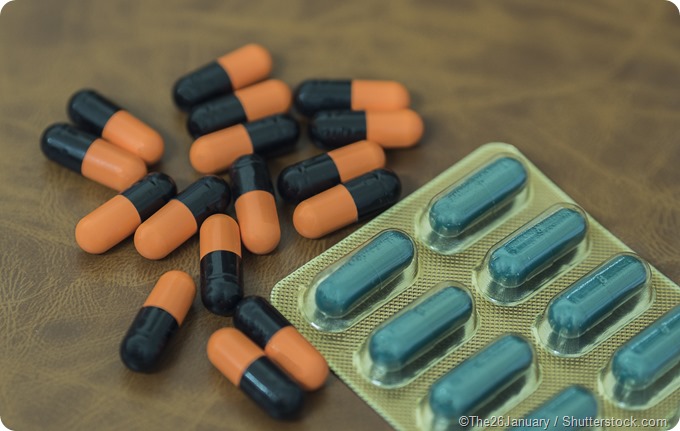
Before the use of an antibiotic, which is a synthetic nitroimidazole drug with antiprotozoal and antibacterial activities was introduced in clinical practice in 1959, the only way to treat trichomoniasis was local vaginal therapy with predominantly palliative effect in the affected women. Today this antibiotic first used in 1959 is still the drug of choice for this condition.
Treatment options for trichomoniasis
As already mentioned, the current mainstay of treatment against Trichomonas vaginalis (and trichomoniasis) is an antibiotic. Current guidelines from the World Health Organization (WHO) and the US Centers for Disease Control and Prevention (CDC) for the treatment include 2 grams in a single dose as a recommended regimen, or 400-500 milligrams twice a day for seven days as an alternative regimen.
Despite its effectiveness, the mode of action of the antibiotic is still not completely understood. It appears that the drug is readily absorbed into cells, which is followed by DNA binding via intermediate metabolites and protein synthesis inhibition, ultimately resulting in cell death.
During the course of treatment (and 24 hours after the last dose) patients with trichomoniasis should avoid alcohol consumption. Furthermore, pregnant women without any symptoms are advised to postpone the treatment until after 37 weeks of gestation, while symptomatic women are usually treated with 2 grams of antibiotic in a single dose.
Nevertheless, the topical application of certain drugs (most notably clotrimazole) has been employed to augment the antiprotozoal activity of systemic antibiotic, but also to achieve potential synergistic activity against strains of the parasite that are resistant to the antibiotic.
Antimicrobial susceptibility testing
As the majority of organisms are still susceptible to the prescribed treatment, antimicrobial sensitivity testing is not routinely pursued. In addition, there are no standardized methods or proficiency testing currently at our disposal. Nevertheless, women with clinically resistant Trichomonas vaginalis are increasingly observed, introducing the need for this additional laboratory work.
Susceptibility testing of Trichomonas vaginalis can be done in shell vials or in microtiter wells in order to determine minimal inhibitory concentration (also known as MIC) of the tested antibiotic. Still, it must be emphasized that no correlation with clinical resistance can be made if anaerobic conditions are used in the susceptibility testing, i.e. the organism must be grown aerobically.
The development of resistance
According to the US Centers for Disease Control and Prevention (CDC), between two and five percent of patients with trichomoniasis may harbor parasite that shows low-level antibiotic resistance; conversely, high-level resistance of Trichomonas vaginalis is rarely found. Still, at the end of 20th century there was a 17-fold growth in resistance incidence of this organism.
Generally, the first type of resistance to appear is the aerobic resistance in patients non-responsive to treatment. This is followed by the development of the anaerobic resistance with progressive loss of hydrogenosomal proteins that are associated with drug-activating pathways.
As the incidence of drug resistance in Trichomonas vaginalis isolates is still on the rise, future studies are needed in order to accurately evaluate the correlation of in vitro drug susceptibility with treatment outcomes in patients with trichomoniasis. This may be guided by the Trichomonas Genome Project which was recently inaugurated to find a full range of prospective new drug targets and, subsequently, new drugs.
Further Reading
Last Updated: Dec 29, 2022