Researchers from the University of California San Diego School of Medicine have found cellular triggers within the immune cells that could be controlled in order to kill dormant HIV-1 reservoirs in individuals with HIV-1. This is a breakthrough in understanding of the cellular mechanisms controlling HIV multiplication within the body say the researchers adding that this could lead to development of drug therapies and targets that could kill HIV reservoirs in the body. The team published their study findings titled, “The Long Noncoding RNA HEAL Regulates HIV-1 Replication through Epigenetic Regulation of the HIV-1 Promoter,” in the latest issue of the journal mBio.
HIV, AIDS virus, 3D illustration Credit: Kateryna Kon / Shutterstock
Human immunodeficiency virus type 1 (HIV-1) affects 1.7 million new individuals annually (as per 2018 reports) and at present around 38 million people around the globe are living with HIV-1. Authors write that “eradication of persistent HIV-1 reservoirs remains the main barrier to achieving a cure for HIV-1/AIDS.”
Tariq Rana, PhD, professor of pediatrics and genetics at UC San Diego School of Medicine and lead author of the study said, “This is one of the key switches that the HIV field has been searching for three decades to find. The most exciting part of this discovery has not been seen before. By genetically modifying a long noncoding RNA, we prevent HIV recurrence in T cells and microglia upon cessation of antiretroviral treatment, suggesting that we have a potential therapeutic target to eradicate HIV and AIDS.”
The team explains that HIV spreads via body fluids and attacks the immune system leading to immunodeficiency or AIDS. Antiretroviral drugs or ART are given in combination to prevent the spread of the infection as well as multiplication of the HIV in the body. This keeps the patient from developing AIDS. The virus remains dormant in persons on medication but does not go away explain the researchers. Once the drug therapy is discontinued, the virus begins to multiply and brings back the disease. Authors write, “A major challenge in finding a cure for HIV-1/AIDS is the difficulty in identifying and eradicating persistent reservoirs of replication-competent provirus.”
The team found that the HIV affected macrophages or immune cells contained a long noncoding RNA (lncRNA) comprising of over 200 nucleotides. They genetically sequenced over 1145 lncRNAs. These RNA are special in the sense that they do not code for any proteins like other RNAs but act as switches to control other genes that regulate certain protein synthesis. The researchers found a particular lncRNA called the HIV-1 Enhanced LncRNA (HEAL) and found that it was raised in persons with HIV. HEAL regulates HIV replication in the immune cells including macrophages, T cells and microglia in the brain. Here the team looked at the effects on “HIV-1-infected primary monocyte-derived macrophages (MDMs)”.
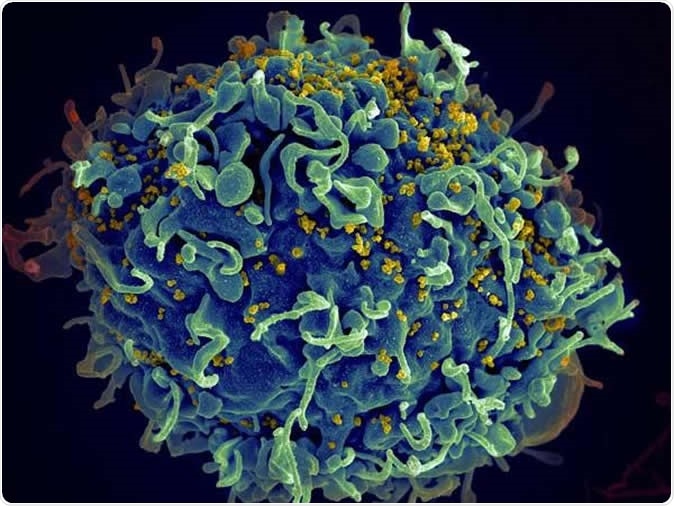
HIV infecting a human cell. Image Credit: NIH
The team explained that HEAL makes a complex with an RNA-binding protein called the FUS. This protein plays a role in HIV replication mediated by two mechanisms. The first mechanism is binding of the HEAL-FUS complex to an HIV promoter that enhances the activity of histone acetyltransferase p300 which in turn activates HIV replication. The second mechanism is that the HEAL-FUS complex works at the promoter region of the cyclin-dependent kinase 2 gene (CDK2) and enhances its expression.
As a next step the team worked on silencing the HEAL using biochemical, cellular or genetic means. They used RNA inhibition to silence the HEAL write the researchers. They also tried to edit out or delete HEAL using CRISPR-Cas9. Once HEAL was out of the picture, the team noted that HIV failed to recur even after antiretroviral drugs were stopped. The team wrote, “Importantly, HEAL is a broad enhancer of multiple HIV-1 strains because depletion of HEAL inhibited X4, R5, and dual-tropic HIV replications and the inhibition was rescued by HEAL overexpression.” The team explained that they are taking the experiments to the next level by moving from the petri dishes to animal studies.
Rana said, “Our results suggest that HEAL plays a critical role in HIV pathogenesis. Further studies are needed to explain the mechanism that leads to HEAL expression after an individual is infected by HIV, but this finding could be exploited as a therapeutic target.”
The authors concluded, “Despite our increased understanding of the functions of lncRNAs, their potential to develop HIV/AIDS cure strategies remains unexplored... HEAL forms a complex with the RNA-binding protein FUS to enhance transcriptional coactivator p300 recruitment to the HIV promoter.” They wrote that HEAL could be “a potential therapeutic target to cure HIV-1/AIDS.”
Journal reference:
The Long Noncoding RNA HEAL Regulates HIV-1 Replication through Epigenetic Regulation of the HIV-1 Promoter Ti-Chun Chao, Qiong Zhang, Zhonghan Li, Shashi Kant Tiwari, Yue Qin, Edwin Yau, Ana Sanchez, Gatikrushna Singh, Kungyen Chang, Marcus Kaul, Maile Ann Young Karris, Tariq M. Rana mBio Sep 2019, 10 (5) e02016-19; DOI: 10.1128/mBio.02016-19, https://mbio.asm.org/content/10/5/e02016-19