The UK is all set to launch its run into the future as the undisputed leader in the field of personalized and effective radiation therapy. The proposal is undergirded by a whopping £56 million, which will be used to set up and fund advanced radiation therapy research by a new collaborative setup, Cancer Research UK RadNet, over five years. This is the largest sum ever invested by this organization into radiotherapy research. The announcement is due to be made on November 3, 2019, at the National Cancer Research Institute (NCRI) conference in Glasgow, by the charity Cancer Research UK.
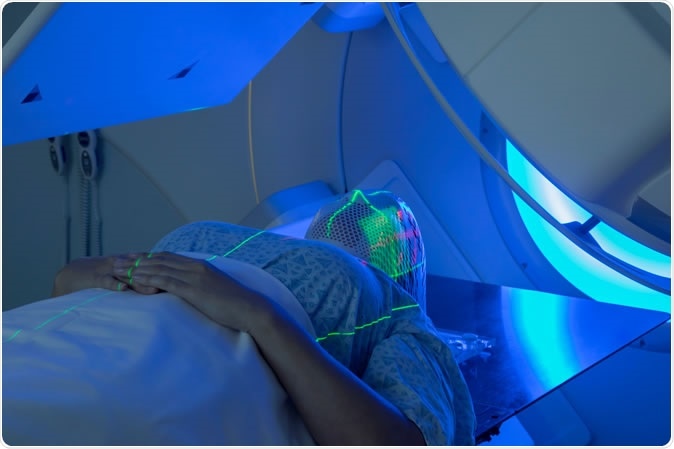
Woman receiving Radiation Therapy for Cancer Treatment - Image Credit: Mark Kostich / Shutterstock
The need
Radiation therapy is one of the two most frequently used cancer therapies, and is received by approximately 30% of cancer patients. Cancer Research UK has already invested into radiation therapy, dating back to the 1920s when the era of radiation had just dawned. In those days, radium was being used to kill malignant cells. Today’s practices have developed immensely since then, with X-rays being used in most institutions to treat cancer. Radiation introduces lethal mutations into cancer cells, causing them to die slowly or immediately. The UK’s National Health Service (NHS) treats more than 130,000 patients every year.
However, radiation therapy has its drawbacks. Older methods and machines could not effectively target tumor cells alone, making the side effects relatively more severe than with modern techniques. Nowadays, researchers are looking into ways to deliver radiation directly and only to tumor cells,
The solution
The aim of the funding is to push the boundaries of radiation therapy through the exploration of many promising technologies for the first time in the world, thus extending the reach and efficacy of this first-line cancer therapy. The whole point is to push radiation research in the UK to world-beating level, ensuring the best patient-oriented outcomes.
Says Cancer Research UK Trustee Adrian Cellin, “I've seen first-hand how successful radiotherapy can be for patients that I treat, but it’s been frustrating to see the UK lagging behind other countries when it comes to prioritizing research into this vital treatment. Cancer Research UK’s investment will overhaul radiotherapy research in the UK to bring the next generation of treatments to patients sooner.”
New areas of research
These will include:
- FLASH radiation therapy – this technique uses instantaneous high-dose radiation, lasting only a fraction of a second, to expose the tumor to a large dose of radiation over a very short time, thus sparing the healthy tissue around it and reducing sequelae related to tissue damage
- Proton beam therapy – this uses proton beams and not photons, because the former are heavier particles. This ensures that the protons crunch to a stop when they come into impact with the tumor target, following a precisely mapped path. This causes all the build-up energy to be released in one powerful blast, into the tumor itself. The first NHS facility to offer high-energy proton beam therapy is the Manchester-based Christie NHS Foundation Trust. UCL Hospitals NHS Foundation Trust is due to begin its operations in 2020. Meanwhile, the new network will continue to sponsor work on this technology to help doctors and patients exploit it to the greatest advantage.
- Increasing local oxygenation within the tumor – local hypoxia within and around the tumor is due to the rapid rate of tumor growth that outstrips the growth of the blood vessels. As a result, most tumors cannot maintain an adequate blood supply. The upside is that they tend to undergo necrosis as a result. The downside is that during this phase they are not as vulnerable to the harmful effects of radiation, which partly depend on the presence of oxygen. This is because radiation results in the production of free oxygen and nitrogen radicals which are extremely damaging to the DNA, but these require oxygen for their production. Therefore, hypoxic tumors must be identified and oxygenated to get the best results from radiotherapy.
- Stem cells in tumor relapse following radiation therapy – cancerous tumors often contain stem cells, or undifferentiated cells that are capable of developing in many directions because they have not begun to show the characteristics of a single cell type yet. These cells resist the effects of radiation, and thus linger in radiation-treated tumors. Like a few live coals in an apparently extinguished fire, they can thus give rise to a new tumor. Researchers will need to find out how they can specifically destroy cancerous stem cells and thus exploit the full potential of radiation to destroy a tumor.
- Developing new drugs and protocols to be used along with radiotherapy – immunotherapy, chemoradiotherapy and similar new approaches help the body to fight cancer using its own mechanisms and defenses. For instance, immunotherapy takes advantage of the immune system’s ability to fight a targeted enemy specifically and powerfully, by removing the tumor’s disguise, enhancing the immune defenses, and other immune mechanisms. Day by day, scientists are coming up with new insights into how cancer immunity can be made to work with greater efficacy. In addition, researchers want to understand how tumors manage to repair damaged DNA in many cases, following tumor radiation, so that they can interfere with the repair process by specific inhibitors that arrest various stages of the program.
- Artificial intelligence (AI) – this technology is making a deep impact on many fields of health, including cancer radiation. The new network will empower further research into the role of AI in the development of personalized therapy, based on the scan results of individual tumors. This should be capable of enhancing the accuracy of radiation delivery, minimizing unwanted damage to healthy tissue. It should also help to treat patients with deep-seated tumors, or those in which the tumor is so close to vital structures that conventional radiation would endanger the patient.
The network
Cancer Research UK RadNet brings together seven top-rated research centers across the UK, with the Royal Marsden NHS Foundation Trust. These include:
- University of Cambridge - £8 million for molecular-level studies of cancer cell response to radiation, mechanisms of resistance and how to overcome them, genetic engineering in chemoradiotherapy, trials of new radiation sensitizing drugs, new biomarkers of radiation outcomes, and AI to understand a cell’s response to radiation
- University of Glasgow - £3.5 million for research into new radiation protocols including those that use drugs, extending radiation therapy to hitherto unreachable or poor-prognosis areas, such as the head and neck, development of predictive biomarkers, and imaging-aided personalization
- University of Leeds - £3.5 million for research into the role of AI and imaging to achieve precise radiotherapy delivery, testing new chemoradiotherapy protocols, blood and imaging biomarkers for treatment response, with special regard to specific cancers
- University of Manchester - £16.5 million to probe newer combinations of advanced proton beam FLASH and MR-Linac therapy with immunotherapies and chemotherapy, personalization of therapy, biomarkers to predict therapy outcomes, and how radiation, tumor genes, and hypoxia predict certain outcomes such as bowel and lung immune injury and tumor response
- University of Oxford - £3.5 million to examine FLASH, effect of surrounding cells on the tumor, newer imaging- and AI-aided techniques, and alteration of tumor immunity with radiation therapy
- the Cancer Research UK City of London Centre (comprising University College of London, Queen Mary University of London, King’s College London, and the Francis Crick Institute) - £14 million for research into radiation resistance and newer radiation techniques, how the radiotherapy response is affected by immunity and the tumor microenvironment, how AI and imaging can help personalize radiation delivery, and pediatric radiation therapy
- the Institute of Cancer Research, London – £3.5million along with the Royal Marsden NHS Trust to look into molecular basis of radiation response, immune responses in radiation therapy and developing/testing new protocols
A sum of £13 million has been set aside to fund new research teams and more doctoral students, in the leading universities – Cambridge, Manchester and London. This will be seed capital to promote and secure the future of radiation therapy in the UK. Another £4 million is earmarked for joint research, conferences, and deputation-level postings between different scientific fields and centers to take advantage of the differing areas of expertise of a spectrum of scientists with knowledge of this field.