A team of researchers has found that the microflora of bacteria within the gut of humans could be a contributor to the development of pulmonary arterial hypertension (PAH). The study titled, "Altered Gut Microbiome Profile in Patients With Pulmonary Arterial Hypertension," in the latest issue of the American Heart Association's journal Hypertension.
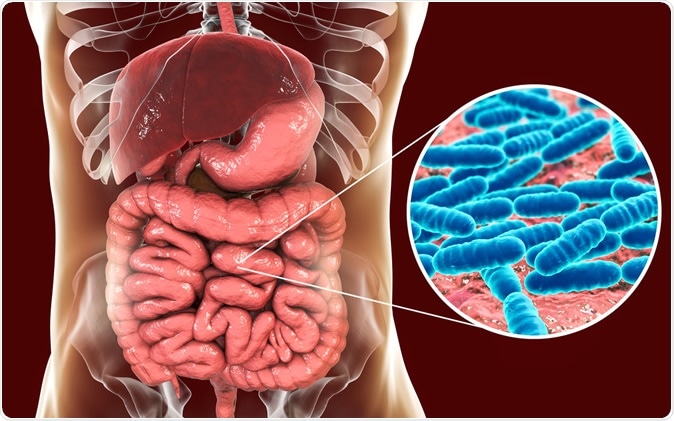
Normal flora of the small intestine, bacteria Lactobacillus, 3D illustration. Lactic acid bacteria. Image Credit: Kateryna Kon / Shutterstock
What is PAH?
According to the experts, PAH results when the arteries that supply blood to the lungs are constricted, and blood supply is impaired. This results in symptoms such as palpitations, shortness of breath, and tiredness. The pressure within the arteries of the lungs rises and this can result in failure of the right side of the heart. This is a progressive condition and can be debilitating and even life-threatening. This team of researchers found a connection between PAH and the normal flora of bacteria that are present in the intestines. This bacterial variety within the gut is called the microbial flora. This new study reveals that specific types of gut flora could be predictive of PAH by up to 83 percent.
What was found?
According to lead researcher Mohan Raizada, a professor in the department of physiology and functional genomics at the University of Florida College of Medicine in Gainesville, Fla., "We showed for the first time that specific bacteria in the gut are present in people with PAH. While current PAH treatments focus on the lungs, looking at the lung/gut axis could open the door to new therapies centered in the digestive system."
The study
For this study, the team included 18 patients who had been diagnosed with type 1 PAH. These patients had a pulmonary arterial pressure of 57.4 mm of Hg. They also included 13 participants who were healthy volunteers. The gut flora in all the participants was gathered and the genetic studies were used to compare the prevalence of different types of bacteria within the guts of the participants.
Results
Results revealed that in the persons with PAH, there was an increased synthesis of "arginine, proline, and ornithine" by the bacterial flora. The bacteria in the PAH patients also showed increased "trimethylamine/ trimethylamine N-oxide and purine metabolism" compared to the healthy control volunteers. These control healthy participants also had increased bacterial flora containing bacteria such as "Coprococcus, Butyrivibrio, Lachnospiraceae, Eubacterium, Akkermansia, and Bacteroides," which produced more of butyrate-and propionate. The team then used these pictures of the flora to predict if a participant would have PAH, and their algorithm was accurate 83 percent of times using the current analysis. Next, the team performed a virome analysis of the gut microbes and found that those with PAH had an increased population of Enterococcal phages and lower amounts of Lactococcal phages.
According to the researchers, this was the first study to look at the connection between PAH and gut microbes, and they explained that alteration of gut microbes has earlier been linked to different heart diseases and hypertension or high blood pressure as well.
Way forward
Raizada said, "We were very surprised to see such an association within a small group of study subjects. It usually requires hundreds of patients to achieve such significance." He explained that despite the fact the gut microbes change often and with diet, their finding shows that these bacteria associated with PAH seem to be constant to a great extent. He said, "We believe these particular bacteria are constant."
Raizada said that it was not clear why the gut bacteria influenced the blood pressure within the lung arteries. He said, "We do not know if and how gut bacteria and viruses make their way to the lungs. Some studies have pointed to an increased incidence in intestinal leakage among people with pulmonary hypertension, which may allow some intestinal bacteria to get into the bloodstream and circulate to the lungs where they can cause inflammation and lead to vascular changes."
As a next step, the team wishes to test their finding in large populations. They expect that with high levels of accuracy, detection of these characteristically abnormal gut microbes could help health care personnel diagnose the PAH early. At present, PAH diagnosis required invasive cardiac catheterization that may be needed when symptoms become overt. With a diagnosis based on gut microbes, the condition could be diagnosed earlier. The team also added that devising ways to correct the microbial flora to healthier microbiota could help treat the PAH or at least stop and slow down the progression of the condition. Raizada signed off, "There is still the question of whether the specific microbiota associated with PAH is the cause or the result of the disease; therefore, more research is needed."
This study was supported by the National Institutes of Health (NIH), National Center for Research Resources and the U.S. Department of Defense.
Source:
Journal reference:
Altered Gut Microbiome Profile in Patients With Pulmonary Arterial Hypertension Seungbum Kim, Katya Rigatto, Marcelo B. Gazzana, Marli M. Knorst, Elaine M. Richards, Carl J. Pepine, Mohan K. Raizada, https://www.ahajournals.org/doi/abs/10.1161/HYPERTENSIONAHA.119.14294