Researchers in the UK have warned that it will be essential to carry out community-based sampling in addition to symptomatic testing if the ongoing transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is going to be properly understood and controlled.
Both types of testing will be needed to accurately inform the test, trace, and isolate practices designed to monitor and control the coronavirus disease 2019 (COVID-19) pandemic, they say.
The team’s study found that since lockdown was eased in England at the end of May, the number of people who tested positive for SARS-CoV-2 did continue to fall.
On comparing two rounds of sample collection – one carried out during May and one in June/early July –the number of positive samples was significantly lower in the second round, although the decline in infection rate was not rapid.
However, the real-time assessment of community transmission antigens study (REACT) also showed that as the prevalence of infection continued to decline, there was an age-and occupation-associated shift in patterns of infection.
The results also suggested that people of Black and Asian ethnicities and people who lived in London were at an increased risk of being infected.
The researchers, from Imperial College London, Lancaster University and the University of Oxford, said the study highlights the importance of conducting community-based, as well as symptomatic testing.
A pre-print version of the paper is available in the server bioRxiv*, while the article undergoes peer review.
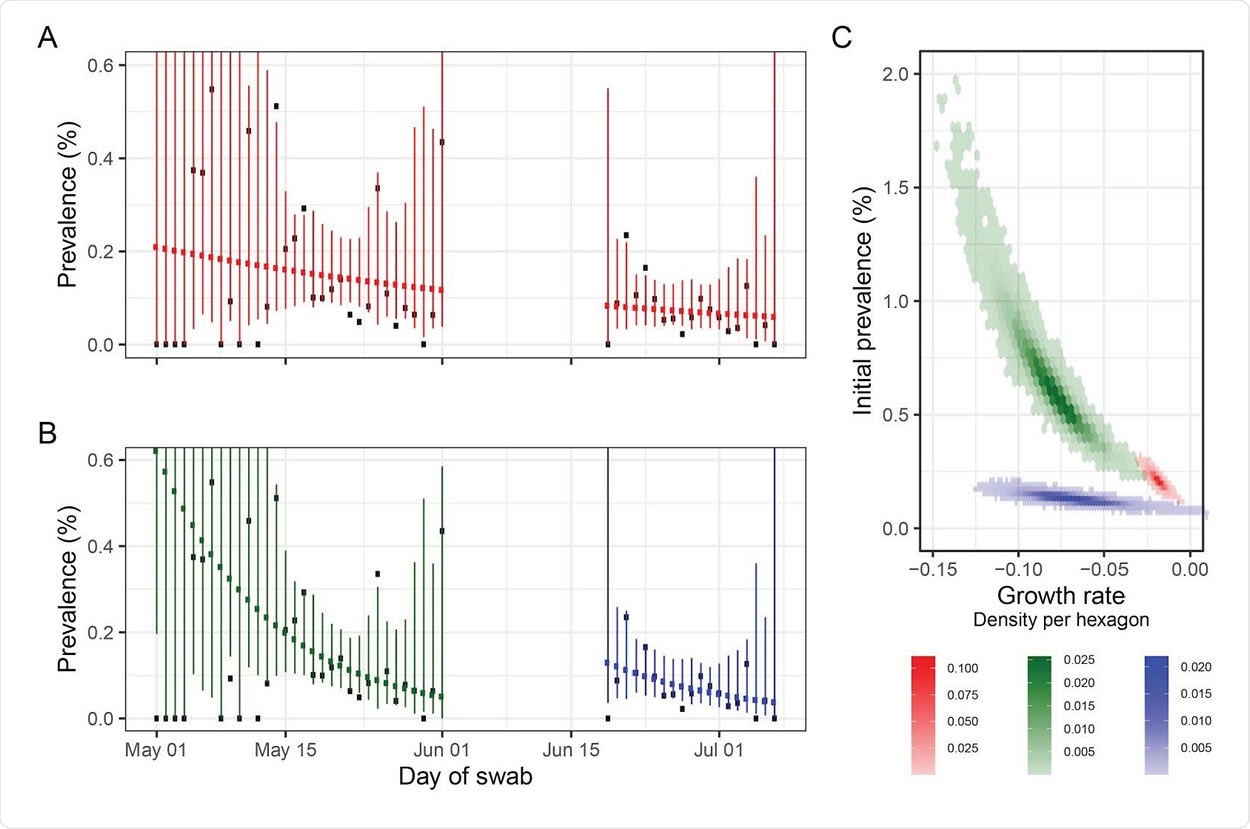
Swab positivity by day with fitted exponential decay models. A Observed daily prevalence of swab-positivity for rounds 1 and 2 with an exponential model of decay fit to both rounds as a single dataset. Red shows best fit for constant decay rate (points) with 95% prediction intervals (vertical lines). B as A, with models fit separately to rounds 1 and 2. C Bivariate posterior density for the three decay models shown in A: red, fit to rounds 1 and 2 (as shown in A); green, fit to only to round 1 (as shown in B, LHS); blue, single round fit to round 2 (as shown in B, RHS).

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
Implementation and relaxation of lockdown
Since the first cases of SARS-C0V-2 infection were first identified in Wuhan, China, late last year, the virus has infected approximately 19.73 million people and killed more than 728,000 worldwide.
Many governments responded to the rapid transmission rates by implementing lockdown measures and social distancing and isolation policies.
In some countries, such measures have successfully prevented the overloading of healthcare services and reduced rates of clinically-confirmed cases.
The full lockdown was imposed in the UK on 23rd March, which was followed by an initial peak in estimated infection rates and then a sustained decline in cases, hospital admissions, and mortality. The government started to ease lockdown in England at the end of May.
To accurately assess the effects of lockdown and its relaxation, surveillance needs to be independent of care-seeking and testing capacities, say Steven Riley (Imperial College London) and colleagues.
“Case-based surveillance is necessarily biased towards symptomatic individuals and sensitive to varying patterns of reporting in space and time,” writes the team.
Overcoming the limitations of case-based surveillance
The REACT study was designed to overcome these problems by acquiring data on nose and throat swab testing, as well as personal, demographic, and symptom data among a representative community-based sample that included asymptomatic people. The study was carried out across 315 lower tier local authority areas.
The first round of sample collection, which was conducted between 1st May and 1st June, identified 159 positive samples among 120,610 swabs tested. The second round, which was carried out in mid-June/early July, identified 123 positive samples among 159,199 swabs tested.
This suggested a downward trend in SARS-CoV-2 prevalence, from 0.13% to 0.077%, corresponding to an average halving time in the growth rate of 38 days and yielding a reproduction number (R) of 0.89.
Many asymptomatic people tested positive
The proportion of people who tested positive and were asymptomatic when samples were collected increased from 69% in the first round to 81% in the second round.
“The high proportion of swab-positive individuals not reporting recent symptoms in both rounds 1 and 2 would be missed by symptom-based surveillance and therefore are a potential source of ongoing transmission that would escape case-based interventions,” writes the team.
The situation improved for healthcare staff, care home workers and 18-24 year-olds
The number of healthcare staff and care home workers who tested swab-positive during round one was much higher than among other groups of workers. However, the odds of these workers being at an increased likelihood of infection over other groups was significantly reduced in round two.
“This result most likely reflects improvements in infection control in health care and care home settings,” suggests the team.
Age patterns of infection shifted between the rounds of sample collection, with the prevalence among 18 to 24 year-olds decreasing five-fold in round two, compared with round one.
Compared with people aged 35 to 44 years, people aged 18 to 24 were at a 96% greater likelihood of infection in round one and a 64% greater likelihood in round two.
Increased risk among Blacks, Asians and people living in London
The study also identified an increased risk of infection among people of Black and Asian ethnicities at the end of lockdown, which the authors say is consistent with other studies showing that these groups are at a higher risk for adverse outcomes.
Riley and the team say further studies are needed to establish the extent to which this increased risk of adverse health outcomes can be explained by differential rates of infection.
Of the nine English regions included in the study, the greatest risk for infection was observed for London.
“Although the epidemic was geographically diffuse at the time of our study, SARS-CoV-2 transmission first took off in London,” writes the team. “Therefore, higher prevalence in London at the end of lockdown suggests that regional rates of decline were similar.”
The researchers emphasize that the current primary control strategy in the UK is to test, trace and isolate cases and to carefully monitor the incidence of local cases so that any further restrictions on social interactions are applied at a local level.
“Community-based, as well as symptomatic testing, is essential to inform these strategies,” concludes the team.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.