In some parts of the world, new outbreaks of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) are occurring after weeks or months of no cases at all. Some instances are the recent occurrence of local cases in Vietnam, New Zealand, and Beijing. A recent study published on the preprint server bioRxiv* in August 2020 suggests that foodborne contamination may underlie these outbreaks and that this route of transmission should not be overlooked to contain the pandemic.
Almost two months of having zero new cases, a cluster of SARS-CoV-2 infected patients were detected in the Xinfadi wholesale market in Beijing. This was officially attributed to contaminated food imported from outside the region. Following this, measures have been put in place to prevent other outbreaks in China. The world at large, however, remains unaware of such a risk, and thus it is mostly ignored.
Reasons for Fresh Outbreaks
New outbreaks may occur due to unrecognized asymptomatic SARS-CoV-2, with continuing community transmission. Another mechanism might be travelers bringing in the virus, which then jumps from host to new host. This would mean that either an asymptomatic infected traveler was tested as false negative or that a confirmed infected traveler broke quarantine rules. This could lead to occult SARS-CoV-2 transmission.
However, the researchers calculate that this is an improbable scenario, given that the odds of the virus passing through 20 generations undetected is only one in a thousand, even if the reproduction number is 1, and with a continuing chain of transmission, and a detection rate of one in twenty infections. In such a situation, occult transmission seems unlikely to be the cause of the recent outbreaks.
Infection Clusters Linked to Foodstuffs
A third possibility is that contaminated foodstuffs transported between regions are carrying the SARS-CoV-2 virus. This is credible given that many SARS-CoV-2 infection clusters have occurred in meat and seafood processing plants all over the world. Examples include a poultry processing factory in the UK, a ready-to-eat meal production facility again in the UK, tuna canneries in Portugal and Ghana, and abattoirs in Australia and Germany. In fact, in the last case, more than 1,500 workers were tested positive for SARS-CoV-2 in a large abattoir in Gutersloh, Germany. This cluster of infections led to the implementation of lockdown in two districts housing over 600,000 people.
Thus, the question of the origin of the recrudescences seems to revolve around food processing plants where contaminated food is imported, transferring the infection to local inhabitants and seeding new chains of viral spread. The SARS-CoV-2 virus has been found on workers at the Xinfadi market, and on cutting boards where salmon imported from outside was sliced.
The officials responded by taking millions of swabs from market workers, people staying near the market, and other components of the Beijing food supply chain. This led to the detection of 335 cases of SARS-CoV-2 infections. Shrimp from Ecuador were also detected to be positive for the virus.
Subsequently, salmon from Europe was banned, as well as later on from any facility where SARS-CoV-2 outbreaks were known to have occurred. This included the US, Germany, and Brazil. Ecuadorean shrimp were also suspended.
Verifying Infectious Virus in Frozen Meat
Many scientists openly doubted this route of transmission, since earlier studies have reported no detectable SARS-CoV-2 on copper, cardboard and stainless steel/plastic surfaces, at a temperature of 21–23°C, when tested after 4 hours, 24 hours, and 3 days. The authors of the current study, therefore, looked at how long the virus could survive on frozen or refrigerated meat and salmon over a period of 3 weeks. This allowed them to test the potential for fresh outbreaks seeded by imported food containing the viable virus.
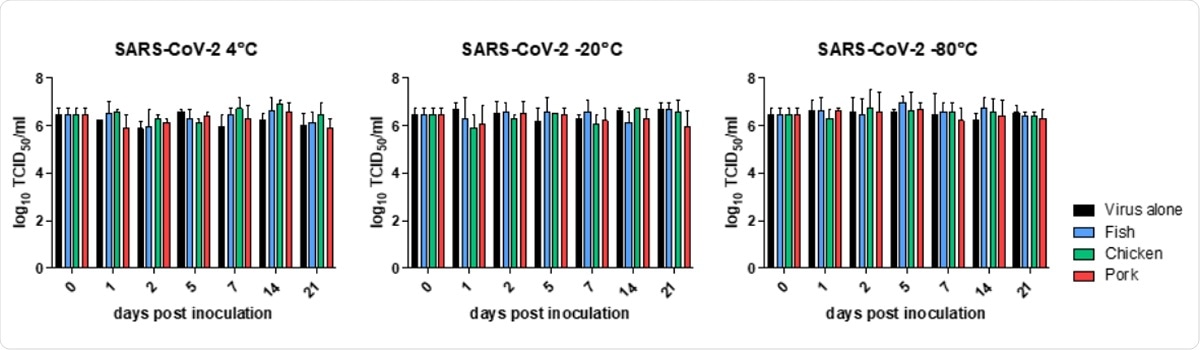
Quantification of the infectious virus over 21 days. Viral titers were determined by limiting dilution. Titres are expressed as mean ± SD log10 TCID50/mL. SARS-CoV-2 was stored alone or in the presence of fish, chicken or pork and tested under refrigeration (4°C); and frozen (-20°C and -80°C).
They tested 500 mm3 cubes of salmon, chicken, and pork bought from supermarkets in Singapore, to which the virus was added at a dose of 200 μl of 3 x 106 TCID50/ml. These were stored at 4˚C, –20˚C and –80˚C. They then tested for the virus at 1, 2, 5, 7, 14, and 21 days later. They found that the viral titer remained at the same level at all three temperatures, and all the samples remained infectious.
In accordance with the general thinking of today, the World Health Organization advises that foodborne or food packaging-associated COVID-19 spread is improbable. The researchers say, “While not a major infection route, the potential for movement of contaminated items to a region with no COVID-19 and initiate an outbreak is an important hypothesis.” This makes it imperative to assess the risk of such foodborne infection surviving the transport and storage process involved in the import trade.
Meat Trade and COVID-19
The high rate of infection among abattoir and meat processing plant workers, as evidenced by the increased number of infection clusters, may point to the risk factors like crowded workplaces, high noise levels making shouts necessary, and lack of adequate ventilation. The meat is handled manually, while automated lines typically handle salmon. In situations where salmon is also handled manually, the risk of contamination arises.
Such workers may also continue to work after being infected since they typically come from low economic strata, they are at higher risk of both catching the virus and passing it on in their crowded homes. They also travel by public transport, which is typically crowded.
The fact that most surfaces in such facilities are likely to be stainless steel, the low temperatures, and lack of sunlight, which contains ultraviolet rays, favor a longer life for the virus. Thus, environmental and individual factors all predispose to meat and fish contamination during the handling of raw meat and further processing.
The researchers explain that while butchering is typically at standard or room temperatures, the meat is then kept at a low temperature below 12oC to be cut up, and the meat is stored at 3–7°C as per food regulations.
Implications
The study shows that all types of meat in everyday use, namely, chicken, pork, and salmon, can carry the infectious virus throughout the transport and storage periods and conditions involved in the import and export of these foods. Notably, the tested temperatures cover that of standard refrigeration and standard freezing. The absence of conditions like drying and temperature variation, as regulated for such foods by law, favors virus survival. And in fact, they failed to detect any decrease in viral titer, signifying a loss of infectivity.
Thus, they conclude, “We believe it is possible that contaminated imported food can transfer the virus to workers as well as the environment. An infected food handler has the potential to become an index case of a new outbreak.”
Given the high volume of international food trade, it is quite possible that uncommon transmission events can occur and trigger outbreaks where the virus spread had been eradicated previously. To prevent such outbreaks, food hygiene must begin at the factory, including repeated and meticulous cleansing of the hands, work surfaces, and other food contact surfaces, materials, and utensils.
Worker conditions should be inspected. Staff should be trained and encouraged to absent themselves if they are ill, and checks should be carried out. Such worker leaves should be incentivized to promote worker and consumer safety. The use of personal protective equipment should be inspected until a habit is in place, while social distancing at all times should be taught and encouraged.
In the import market, cleaning of hands, utensils, and surfaces should be carried out regularly to prevent contamination of other foods. Consumers should be taught to wash their hands after touching any raw food and to cook the food properly to destroy the virus.
The current study and other reports of the detection of the virus on imported frozen chicken and shrimp packaging material should serve as a warning to food regulatory and public health authorities to set relevant guidelines in this new situation, where old norms may not be useful to avert a “non-traditional food safety risk.’

 *Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.