A team of researchers from Brazil, the United States, and the UK has conducted a study showing that herd immunity played a significant role in determining the size of the coronavirus disease 2019 (COVID-19) epidemic in Manaus, the capital city of the Brazilian state of Amazonas.
According to the study estimates, the transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) – the agent that causes COVID-19 – rapidly increased in Manaus between March and April, before slowly declining between May and September.
In June, the prevalence of SARS-CoV-2 seropositivity peaked at 52%, before then falling during July and August, as antibody levels against the virus started to wane.
After adjusting for this antibody waning, Ester Sabino (University of São Paulo) and colleagues estimated a final epidemic size of 66%.
The team says the unusually high infection rate, followed by a sustained drop in cases, suggests that population immunity played a significant role in determining the size of the epidemic in Manaus.
A pre-print version of the paper is available in the server medRxiv*, while the article undergoes peer review.
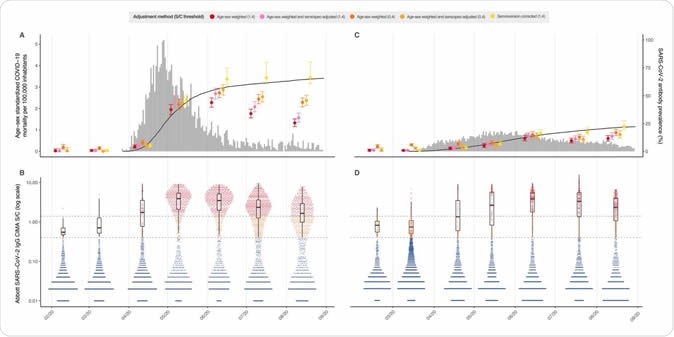
Monthly antibody prevalence and signal-to-cutoff (S/C) reading in Manaus and São Paulo. SARS-CoV-2 antibody prevalence estimates in Manaus (A) and São Paulo (C) with a range of corrections. Error bars are 95% confidence intervals. Grey bars are standardized daily mortality using confirmed COVID-19 deaths in the SIVEPGripe (https://covid.saude.gov.br/) notification system and standardized by the direct method using the total projected Brazilian population for 2020 as the reference. Black lines are the cumulative deaths rescaled so that the maximum is set to the maximum seroprevalence estimate for each city. Mortality data is plotted according to the date of death. Distribution of S/C values over the seven monthly samples are shown for Manaus (B) and São Paulo (D). Each point represents the S/C reading for a single donation sample. Upper dashed line - manufacturer’s threshold (1.4 S/C units); lower dashed line - alternative threshold (0.4 S/C units); black boxplots show the median, interquartile range and range of S/C values above 0.4 (i.e., excluding very low and likely true-negative values.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Importance of the herd immunity threshold
Currently, there is no consensus regarding the proportion of a population that must become infected with SARS-CoV-2 for herd immunity to be reached. This is the threshold above which each case of infection results in less than one secondary infection, and disease incidence starts to decline in the absence of other preventive measures.
Estimates of the herd immunity threshold can help to inform public health policies and decisions over whether to relax mitigation measures and reopen society.
“The herd immunity threshold, together with social distancing and other control measures, determine the final epidemic size,” say the researchers.
When conducted in a given location, serial cross-sectional seroprevalence studies can produce empirical evidence of the final epidemic size, say Sabino and team.
However, although seroprevalence studies have been carried out in Europe and North America, the relatively low estimates of cumulative infections (usually less than 20%) cannot be assumed to reflect herd immunity, given the widespread implementation of effective non-pharmaceutical control interventions.
By contrast, Brazil has seen one of the most rapidly-growing rates of COVID-19 in the world.
In Manaus, the capital of the Amazonas state, the first case of SARS-CoV-2 was identified on 13th March 2020. This was followed by an explosion in cases, and excess mortality in the city during the first week of May was 4.5 times higher than the year before.
This peak in the epidemic was followed by a sustained drop in cases and mortality, even though control measures were relaxed.
Although the ideal study design for determining SARS-CoV-2 infection would include a population-based sample, this approach is time-consuming and expensive, say Sabino and colleagues.
“Routine blood donations can serve as a logistically-tractable alternative,” they add.
What did the current study involve?
Now, the researchers have presented cross-sectional monthly estimates of SARS-CoV-2 prevalence among blood donors in Manaus for the first seven months of infection transmission in Brazil.
In February and March, seroprevalence was less than 1% in Manaus, but quickly increased to 4.8% in April, 44.2% in May, and 51.8% in June. This increasing seroprevalence was found to closely follow the curve of cumulative mortality.
Following the peak seroprevalence in June, the effect of antibody waning became apparent, with the proportion of blood donors testing seropositive falling to 40.0% in July and 30.1% in August.
Following adjustment for this antibody waning over July and August, the team estimated that 66% of the population in Manaus was infected with SARS-CoV-2 throughout the course of the epidemic.
“Herd immunity played a significant role in determining the size of the epidemic”
The non-pharmaceutical interventions implemented in Manaus in late March were similar to those introduced in other Brazilian cities. Furthermore, cell phone mobility data revealed a significant increase in physical distancing that started in mid-March and followed a similar pattern to the distancing seen in the city of São Paulo.
“Therefore, it remains unclear what accounted for such rapid transmission of SARS-CoV-2 in Manaus,” writes the team.
The researchers say potential contributing factors include poor socioeconomic conditions, with crowded households, and reliance on boat travel, where overcrowding can accelerate transmission.
“Although non-pharmaceutical interventions, plus a change in population behavior, may have helped to limit SARS-CoV-2 transmission in Manaus, the unusually high infection rate suggests that herd immunity played a significant role in determining the size of the epidemic,” concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Sabino E, et al. COVID-19 herd immunity in the Brazilian Amazon. medRxiv, 2020. doi: https://doi.org/10.1101/2020.09.16.20194787
- Peer reviewed and published scientific report.
Buss, Lewis F., Carlos A. Prete, Claudia M. M. Abrahim, Alfredo Mendrone, Tassila Salomon, Cesar de Almeida-Neto, Rafael F. O. França, et al. 2020. “Three-Quarters Attack Rate of SARS-CoV-2 in the Brazilian Amazon during a Largely Unmitigated Epidemic.” Science, December. https://doi.org/10.1126/science.abe9728. https://www.science.org/doi/10.1126/science.abe9728.