Several studies have shown that increased exposure to polluted air is associated with the severity of disease. Air pollution has also been shown to aggravate the course of the coronavirus disease 2019 (COVID-19) pandemic. Many industrial chemicals are known to suppress immune functions and worsen the disease course in many infections. Globally disseminated and immunotoxic industrial chemicals like perfluorinated alkylate substances (PFAS) may contribute to this as well.
Thus, elevated background exposure to PFAS is associated with decreased antibody responses to vaccinations in children and adults. Also, children with higher levels of exposure to these chemicals are more prone to infectious diseases. Moreover, major PFAS are said to interfere with proteins involved in critical pathways linked to severe clinical outcomes for COVID-19.
Assessing the impact of elevated PFAS exposures on the course of SARS-CoV-2 infection
A team of researchers from the Harvard T.H.Chan School of Public Health, Boston, MA; University of Southern Denmark; Odense University Hospital, Denmark; Statens Serum Institut, Copenhagen, Denmark; National University Hospital, Copenhagen, Denmark; and the University of Copenhagen recently carried out a study in Denmark in which they determined the plasma PFAS concentrations in individuals with a confirmed severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection.
This scanning electron microscope image shows SARS-CoV-2 (round magenta objects) emerging from the surface of cells cultured in the lab. SARS-CoV-2, also known as 2019-nCoV, is the virus that causes COVID-19. The virus shown was isolated from a patient in the U.S. Image captured and colorized at NIAID's Rocky Mountain Laboratories (RML) in Hamilton, Montana. Credit: NIAID

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
They wanted to assess the impact of elevated background exposures to immunotoxic PFAS on the infection's clinical course and study the association of PFAS exposure with the COVID-19 severity. Their work is published on the preprint server medRxiv*.
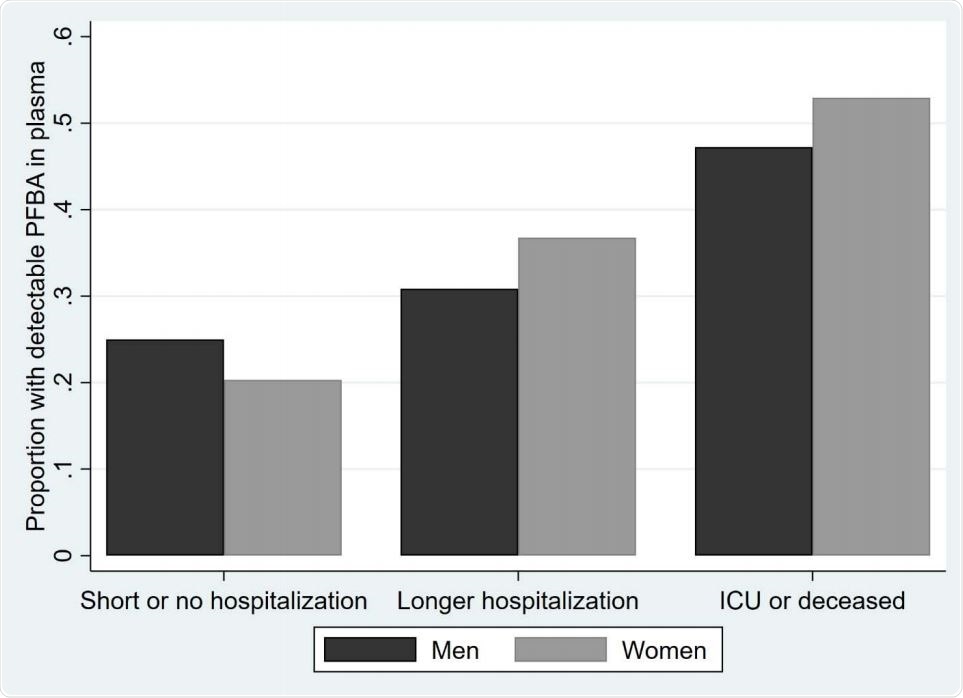
Proportion of plasma samples with detectable PFBA concentrations at different disease severities. Results are shown for 44 men and 64 women with up to two weeks of hospitalization, 94 men and 68 women with longer hospitalization, and 36 men and 17 women admitted to the intensive care unit (ICU) or deceased (P = 0.003).
Using ordinal and ordered logistic regression analyses to identify links between PFAS levels and disease severity
The team obtained plasma samples of 323 individuals with confirmed SARS-CoV-2 infection from Danish biobanks. The subjects belonged to the age group of 30-70 years. The concentrations of PFAS were measured at the background exposures, and the study included 5 PFAS that are known to be immunotoxic.
Registration data of the subjects was obtained to classify them based on disease status and demographic variables. The team used ordinal and ordered logistic regression analyses to study the associations between PFAS levels and clinical outcomes.
The study results showed that plasma-PFAS levels were higher in males and patients with Western European background. While the PFAS levels tend to increase with age, they were not necessarily associated with the presence of chronic disease. Out of 323 subjects, 108 (33%) were not hospitalized, and among those who were hospitalized, 53 (16%) were either in intensive care or deceased.
"The results of this study are parallel to findings in regard to other environmental toxicants, viz., air pollutants and suggests a need to ascertain the impact of relevant occupational or environmental exposures on COVID-19 severity."
Among the five immunotoxic PFAS studied, perfluorobutanoic acid (PFBA) had an odds ratio (OR) of 2.19 for increasing disease severity. However, OR decreased to 1.77 after it was adjusted for sex, age, sampling site, blood sampling, and diagnosis interval.
Increased plasma concentrations of PFBA is associated with severe COVID-19 prognosis
This study aimed at evaluating the potential worsening of COVID-19 disease associated with increased background exposure to PFAS. Several PFAS have been shown to be immunotoxic agents in experiments with lab animals and also in humans.
According to the authors, this study's results agree with the findings of previous studies on other environmental toxicants or air pollutants and highlights the need to confirm the impact of occupational or environmental exposures to air pollutants on the severity of COVID-19.
The team says that while existing evidence on air pollution is solely based on ecological studies that don't take into account individual exposure levels, their present study benefits from determining the plasma-PFAS levels of the subjects.
The authors concluded that increased plasma PFBA levels were associated with more severe COVID-19 prognosis, even after adjustment for comorbidities, sex, age, origin, sampling time, and location. Although PFBA levels in plasma were lower than most PFAS studied, PBFA accumulates in the lungs, and hence they believe that PBFA exposure may contribute to the severity of disease.
"These findings at background exposure levels suggest a need to ascertain if exposures to environmental immunotoxicants may worsen the outcome of the SARS-CoV-2 infection."

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Severity of COVID-19 at elevated exposure to perfluorinated alkylates Philippe Grandjean, Clara Amalie Gade Timmermann, Marie Kruse, Flemming Nielsen, Pernille Just Vinholt, Lasse Boding, Carsten Heilmann, Kaare Molbak medRxiv 2020.10.22.20217562; doi: https://doi.org/10.1101/2020.10.22.20217562, https://www.medrxiv.org/content/10.1101/2020.10.22.20217562v1
- Peer reviewed and published scientific report.
Grandjean, Philippe, Clara Amalie Gade Timmermann, Marie Kruse, Flemming Nielsen, Pernille Just Vinholt, Lasse Boding, Carsten Heilmann, and Kåre Mølbak. 2020. “Severity of COVID-19 at Elevated Exposure to Perfluorinated Alkylates.” Edited by Jaymie Meliker. PLOS ONE 15 (12): e0244815. https://doi.org/10.1371/journal.pone.0244815. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0244815.