The coronavirus disease (COVID-19) pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), continues to spread across the globe. Though some countries report surging cases, others seemed to have contained the virus's spread.
Many high-income countries have reported rising numbers of cases, while a few low-income countries such as the Philippines report a less severe COVID-19 outbreak. To date, the archipelagic country in Southeast Asia has reported 502,000 cases and 9,900 deaths among its population of around 108 million.
A team of researchers at the Department of Biology, the University of Hawaii at Manoa, Hawaii, Ateneo de Manila University in the Philippines, and the School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia, reported that the COVID-19 dynamics in the Philippines are driven by age, contact structure, and mobility.
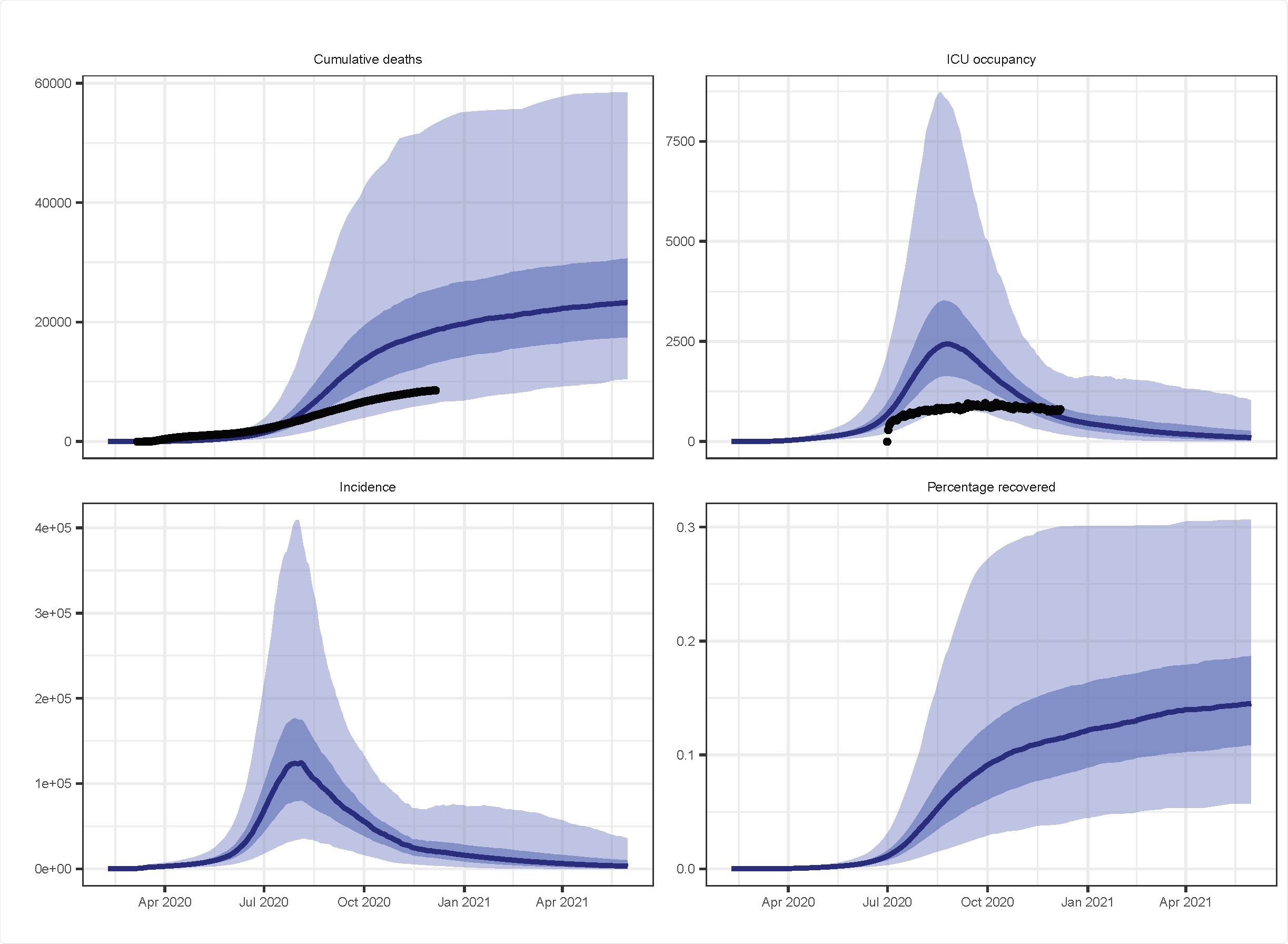
Model estimated epidemic indices from the calibrated Philippines model. Modeled median cumulative deaths, ICU occupancy, incidence, and percentage of the population recovered from COVID-19 (blue line) with shaded areas for 25th to 75th centile (dark blue) and 2·5th to 97·5th centile (light blue) and overlaid with reported cumulative deaths and ICU occupancy (black dots). Note that only the most recent estimate of cumulative deaths and ICU occupancy were included in the likelihood function, with the other time points presented as validation. ICU occupancy data was considered to have improved over the course of the epidemic.
Less severe COVID-19 outbreak
The COVID-19 pandemic first arrived in the Philippines in January 2020, as two tourists from Wuhan City, China, arrived in the country. From there, the virus spread through communities.
To date, the country is still under community quarantine measures, wherein schools are still closed, and people who are at high-risk are now allowed to go out, unless for essential travels.
The study, posted on the pre-print server medRxiv*, investigated COVID-19 epidemiology in the Philippines and the efficacy and sensitivity to micro-distancing policies.
The Philippines is a low-and middle-income country (LMIC) severely hit by the pandemic in the Western Pacific Region. However, the country succeeded in containing the virus's spread while easing its most restrictive quarantine measures.
The country has not yet rolled out vaccinations but is currently in discussions with vaccine providers. To curtail the coronavirus outbreak, the government has implemented non-pharmaceutical interventions, including school closures, community quarantines, and postponement of large-scale public events.
Since October 2020, the country has shifted from community quarantine orders to comply with Minimum Health Standards (MHS) policies. These include wearing of masks and face shields, social distancing, and regular hand washing.
In the study, the team wanted to see why the country has controlled the virus's spread, even though it is an LMIC. They presented a data-driven COVID-19 model, including age, contact patterns, time-varying testing rates, and macro-and micro-distancing.
The researchers found that younger age, changes in mobility, and personal protective behaviors, seem to explain why the country has maintained a less severe COVID-19 outbreak than high-income countries.
The study findings show that COVID-19 epidemiology in the Philippines is no different from higher-income countries. For example, the country's hospitalization and the infection fatality rate are similar to HICs.
Also, the study underlines the essence of robust surveillance and reporting systems to understand COVID-19 epidemiology better. A country with younger populations may help reduce the disease burden since there is a lower percentage of the elderly, which are at a higher risk of being seriously ill with COVID-19. Those who survive to old age in the country are often of higher socioeconomic status and have a lower infection risk.
The team also noted that the country has more intergenerational contacts, which can lower the disease burden because older adults often reside with family rather than home care facilities, where other countries report surging cases tied to these facilities.
The study findings also showed that the country has lesser severe outbreaks than other countries because it gradually eased quarantine measures, and people adhered to MHS.
"These results were consistent across regions that span a wide population density gradient, suggesting that this approach could also be effective in other similar settings," the team noted in the paper. Further, the residents practice personal protective measures, which are essential while waiting for vaccines' availability.
Over the past months until the holidays, the country reports about 1,500 cases per day, leaving hospitals with adequate intensive care unit capacity.
"As people resume semi-normal activities while maintaining MHS, low levels of transmission are likely to continue, but should not overwhelm the healthcare system," the team added.
The team added that the country provided an approach that could help other countries relax interventions more safely. This is important in countries where winter starts to kick in.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Source:
Journal references:
- Preliminary scientific report.
Caldwell, J., de Lara-Tuprio, E., Teng, T.R. et al. (2021). Understanding COVID-19 dynamics and the effects of interventions in the Philippines: A mathematical modelling study. medRxiv. https://www.medrxiv.org/content/10.1101/2021.01.14.21249848v1
- Peer reviewed and published scientific report.
Caldwell, Jamie M., Elvira de Lara-Tuprio, Timothy Robin Teng, Maria Regina Justina E. Estuar, Raymond Francis R. Sarmiento, Milinda Abayawardana, Robert Neil F. Leong, et al. 2021. “Understanding COVID-19 Dynamics and the Effects of Interventions in the Philippines: A Mathematical Modelling Study.” The Lancet Regional Health - Western Pacific 14 (September): 100211. https://doi.org/10.1016/j.lanwpc.2021.100211. https://www.thelancet.com/journals/lanwpc/article/PIIS2666-6065(21)00120-6/fulltext.