Researchers in the UK have warned that cardiometabolic and pulmonary events among coronavirus disease 2019 (COVID-19) survivors following their discharge from hospital is likely to have an ongoing and substantial impact on the National Health Service (NHS) in England.
The team found that rates of these post-hospitalization events among more than 31,000 COVID-19 survivors were at least as high as among patients who had been discharged from hospital with pneumonia.
For the study, the team – from the University of Oxford, London School of Hygiene and Tropical Medicine, and The Phoenix Partnership in Leeds – used information from a data analysis platform called OpenSAFELY.
The OpenSAFELY platform was developed during the COVID-19 pandemic on behalf of NHS England to enable near real-time analysis of pseudonymized primary care records at scale, representing around 40% of England's population.
"We were able to source our cohorts from the OpenSAFELY platform, which contains over 17m adults," writes the team.
The rates of cardiometabolic and pulmonary events showed a similar pattern of elevation between the COVID-19 and pneumonia groups.
However, rates of stroke, pulmonary embolism, myocardial infarction, acute kidney injury, and incident type 2 diabetes were somewhat higher among the COVID-19 survivors.
Ben Goldacre and colleagues say the COVID-19-related events will probably continue to make up a substantial proportion of the overall hospitalizations for these conditions for some time.
"Further work is needed to identify what characteristics of COVID-19 patients put them at highest risk of adverse events," say the researchers.
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.
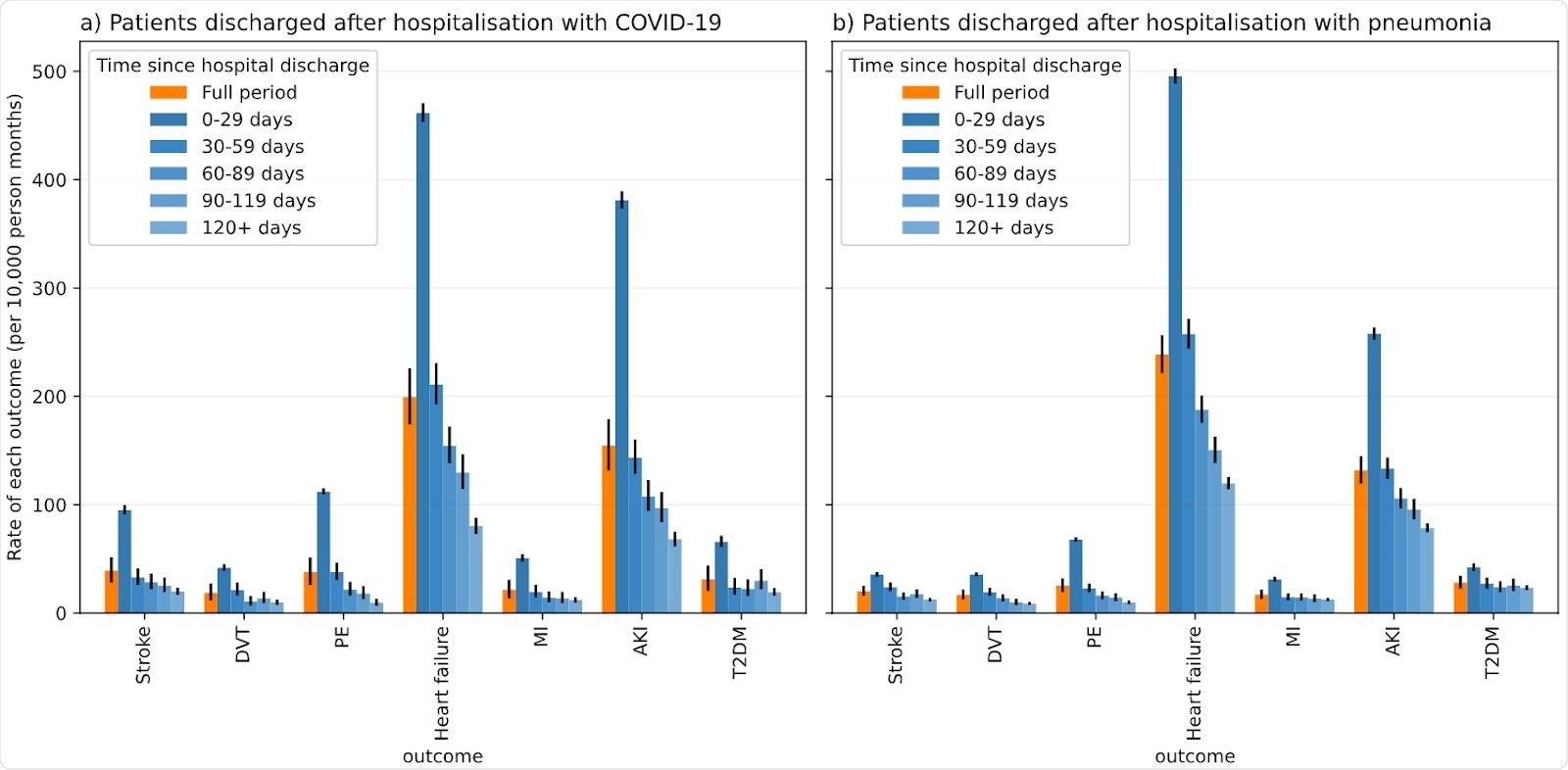
Rate of outcomes (events per 10,000 person months) in time periods following hospital discharge for COVID-19/pneumonia.
Evidence of a "post-acute COVID-19 syndrome" is increasing
Cardiometabolic and pulmonary complications, particularly thrombotic events, have been reported as key features of severe COVID-19. One study recently estimated that the risk of venous thromboembolism is around 15% among hospitalized COVID-19 patients, with this figure rising to around 30% among those who require intensive care.
"As the COVID-19 pandemic has progressed, it is increasingly reported that some patients who recover from the acute disease phase go on to experience a range of post-recovery clinical problems," says Goldacre and the team. "This post-acute COVID-19 syndrome is currently not well described or understood, with the UK National Institute for Health and Care Excellence stating that any bodily system could be affected, for an undetermined period of time."
Defining and quantifying the outcomes that characterize any such syndrome is essential so that both healthcare systems and patients can estimate the levels of burden to expect and plan for them accordingly.
It is also unknown whether COVID-19 is exceptional in its association with cardiometabolic and pulmonary events or whether this occurs with other respiratory infections.
"Work to date on cardiometabolic outcomes with COVID-19 has largely focused on risks during hospitalization, with a lack of evidence on how these risks evolve in survivors of severe COVID-19," writes Goldacre and colleagues.
What did the researchers do?
The team used OpenSAFELY data linking primary care records to death certificate and hospital data to assess 31,569 adult patients discharged from hospital (between 1st February and 1st November 2020) following the acute phase of COVID-19.
Rates of cardiometabolic and pulmonary events among these patients were compared with those among 68,303 patients discharged following hospitalization with pneumonia across the equivalent period in 2019 (prior to the pandemic).
Eight outcomes of interest were measured following hospital discharge: deep vein thrombosis, pulmonary embolism, ischemic stroke, myocardial infarction, heart failure, acute kidney injury and new diagnosis of type 2 diabetes.
Results were stratified by 30-day time windows (0–29 days; 30–59; 60 – 89; 90–120; and 120 plus) post-discharge to assess how the rate of outcomes changed over time.
What did the study find?
The rates of cardiometabolic and pulmonary complications followed a similar pattern of elevation between the two patient groups.
The highest rate of complication was observed in the initial 30 days post-discharge. This was followed by a 2-3 fold decrease in rate over the next 30 days, and then a more gradual decline.
Across both cohorts, complication rates were most pronounced for heart failure and acute kidney injury.
However, for the majority of outcomes, higher rates of serious cardiometabolic and pulmonary complications were observed among the COVID-19 patients than among the pneumonia patients.
Cox regression analysis revealed that compared with the pneumonia cohort, complication rates among the COVID-19 cohort were 78% higher for stroke, 38% higher for pulmonary embolism, 46% higher for myocardial infarction, 27% higher for acute kidney injury and 28% higher for type 2 diabetes.
The COVID-19-related events are likely to substantially impact on the NHS in the future
"The impact of the post-COVID-19 hospitalization events described in this study upon the NHS in England is substantial," writes the team. "It is likely that these COVID-19-related events will continue to make up a substantial proportion of the total hospitalizations for these conditions for some time."
"Next steps include seeing whether patients at highest risk of post-COVID outcomes can be identified and determining whether higher-risk groups could be targeted early for possible preventative action," concludes Goldacre and colleagues.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Goldacre B, et al. Rates of serious clinical outcomes in survivors of hospitalization with COVID-19: a descriptive cohort study within the OpenSAFELY platform. medRxiv, 2021. doi: https://doi.org/10.1101/2021.01.22.21250304, https://www.medrxiv.org/content/10.1101/2021.01.22.21250304v2
- Peer reviewed and published scientific report.
Tazare, John, Alex J. Walker, Laurie Tomlinson, George Hickman, Christopher T. Rentsch, Elizabeth J. Williamson, Krishnan Bhaskaran, et al. 2022. “Rates of Serious Clinical Outcomes in Survivors of Hospitalisation with COVID-19 in England: A Descriptive Cohort Study within the OpenSAFELY Platform.” Wellcome Open Research 7 (April): 142. https://doi.org/10.12688/wellcomeopenres.17735.1. https://wellcomeopenresearch.org/articles/7-142/v1.