The rapid spread of the severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) has caused the coronavirus disease 2019 (COVID-19) pandemic. To date, the virus has claimed more than 3.8 million lives worldwide.
The reverse transcriptase-polymerase chain reaction (RT-PCR) is considered the gold standard for detecting SARS-CoV-2 in upper and lower respiratory specimens as well as for diagnosing COVID-19.
Researchers have stated even though the neutralizing antibodies are found in the sera several months post COVID-19 recovery, the duration of its presence is not yet known.
Many cases have been reported where patients' PCR results turned negative after their symptoms resolved and a second PCR showed a positive result.
Based on the genomic analysis of COVID-19 reinfected patients, it appears that they were reinfected as opposed to not clearing the initial infection. However, a research gap exists regarding genomic evaluations.
Reinfection is determined by the presence of two positive molecular tests separated by a negative test and a time gap, along with the recurrence of clinical symptoms.
New research published on the medRxiv* preprint server provides a detailed analysis of COVID-19 patients who had repeated positive PCR tests for SARS-CoV-2 infection in a large US COVID-19 electronic health record (EHR) database. Additionally, researchers of the present study characterized the demographic and clinical data including SARS-CoV-2 test reports, symptoms, medication, and complications associated with COVID-19 disease.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This research has been conducted following the guidelines of the Centers for Disease Control (CDC) and Prevention Common Investigation Protocol for Investigating Suspected SARS-CoV-2 Reinfection.
In this study, scientists characterized the clinical and testing data of 23 patients obtained from a large electronic health record database. These patients had shown repetitive positive SARS-CoV-2 PCR test results, more than sixty days apart, separated by two consecutive negative tests.
The clinical symptoms related to severe COVID-19 disease were ascertained. The median age of the candidates was 64.5 years. Among the 23 candidates, 40% were Black, and 39% were female. Additionally, the majority of the candidates, i.e., 83%, smoked within the preceding year. In terms of health, 61% of the candidates were obese, and 83% had immune compromising conditions.
More than 96% had more than two comorbidities, which included hypertension and diabetes. Among the 23 patients, 19 patients were COVID-19 positive with 60-89 days in between two positive PCR tests and 4 patients showed positive PCR tests, with more than 90 days between two positive tests.
Researchers revealed that in most cases, i.e., over 70% of patients hospitalized during the first positive test were also admitted to the hospital at the second test. This may be because in most cases, reinfection was not associated with less severe disease.
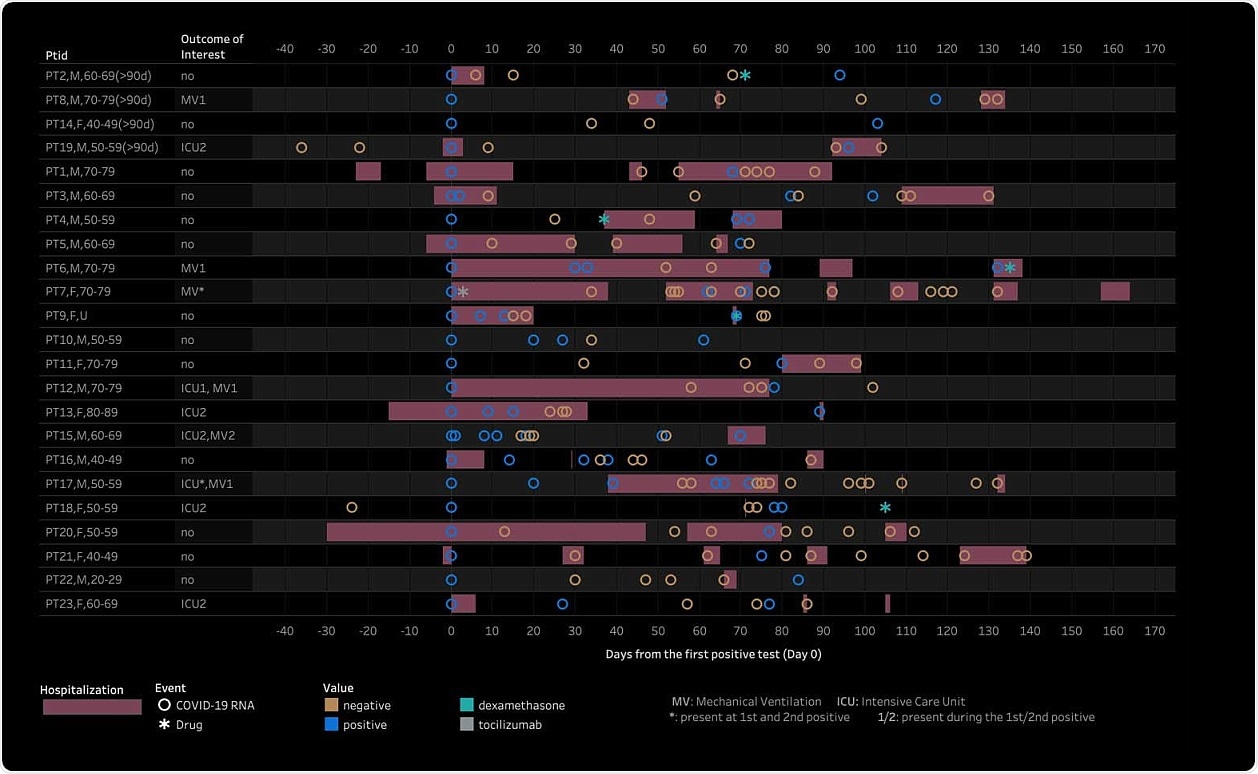
COVID-19 RT-PCR testing and clinical journey for 23 patients with repeatedly positive tests
The study revealed that the percentage of immune-compromised patients, such as advanced stage renal disease on dialysis, solid organ transplant, and cancer, were more in the study population who were affected by COVID-19 compared to the general population without COVID-19. Researchers have revealed that reinfection may be due to increased clinical conditions related to the immune defect.
Researchers also revealed that immune-compromised populations with COVID-19 are at a high risk of getting affected more severely by the disease.
A similar observation was found among patients with a functional kidney transplant, undergoing dialysis, or alcohol-related liver disease.
These observations align with previous observational prospective studies conducted in Madrid, which showed increased mortality and deteriorating liver functions in patients with cirrhosis and COVID-19.
The previous study had shown an average of 101 days between first and second positive tests. Also, viral genomic sequences strongly exhibited reinfection rather than failure to clear an initial infection.
The current study adds to the previous observations by reporting that reinfections may be a common occurrence. However, as most of the patients in the Optum dataset did not have repeated tests after COVID-19 diagnosis, researchers failed to conclude the true incidence rate of recurrent detectable SARS-CoV-2.
One of the current analysis limitations is the lack of data on RT-PCR platforms or semi-quantitative RT-PCR cycle threshold (Ct) values. Nonetheless, candidates included in the present study satisfied the CDC criteria and based on the current data, cases were classified as reinfection instead of relapse of COVID-19 disease. However, researchers failed to determine if COVID-19 was the primary diagnosis associated with hospitalization, if patients were incidentally found to be SARS-CoV-2 positive post-hospitalization for other ailments, or if patients exhibited symptoms during their hospital stay.
Despite the limitations, the present study has provided a comprehensive characterization of a large EHR database across the US. The outcome of this research could help prioritize patients who show signs of reinfection.
More research is required in the future to assess the possibility of reinfection by degree and type of immunosuppressive condition, the severity of disease, etc.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Dong, X. et al. (2021). Comprehensive characterization of COVID-19 patients with repeatedly positive SARS-CoV-2 tests using a large US electronic health record database, medRxiv 2021.06.10.21256915; doi: https://doi.org/10.1101/2021.06.10.21256915, https://www.medrxiv.org/content/10.1101/2021.06.10.21256915v1
- Peer reviewed and published scientific report.
Dong, Xiao, Yujia Zhou, Xiao-ou Shu, Elmer V. Bernstam, Rebecca Stern, David M. Aronoff, Hua Xu, and Loren Lipworth. 2021. “Comprehensive Characterization of COVID-19 Patients with Repeatedly Positive SARS-CoV-2 Tests Using a Large U.S. Electronic Health Record Database.” Edited by N. Esther Babady. Microbiology Spectrum 9 (1). https://doi.org/10.1128/spectrum.00327-21. https://journals.asm.org/doi/10.1128/Spectrum.00327-21.