Researchers in the United States have provided important insights into the immune processes that may be associated with post-acute sequelae of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection – also referred to as long COVID (coronavirus disease 2019).
Approximately 10 to 40% of people who recover from COVID-19 experience post-acute sequelae of SARS-CoV-2 infection (PASC) – a condition characterized by the persistence or recurrence of symptoms that cannot be explained by another health condition.
However, the biological processes associated with PASC are unknown, and there are limited data on immunologic trends over time associated with ongoing clinical symptoms.
Now, researchers from the Icahn School of Medicine at Mount Sinai in New York, the University of California in San Francisco, and Monogram Biosciences Inc., in San Francisco have shown that among individuals recovering from COVID-19, those who went on to develop PASC generally exhibited higher levels of the cytokines tumor necrosis factor-alpha (TNF-alpha) and interferon gamma-induced protein 10 (IP-10) during the early recovery period.
Individuals with PASC also exhibited a trend towards higher levels of the cytokine interleukin 6 (IL-6) during early recovery that became more pronounced during late recovery.
“Persistent immune activation may be associated with ongoing symptoms following COVID-19,” says Michael Peluso and colleagues. “Further characterization of these processes might identify therapeutic targets for those experiencing PASC.”
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
What is known about PASC so far?
The acute phase of SARS-CoV-2 infection is characterized by inflammation and immune dysregulation, but the recovery phase that follows is not well understood.
A significant proportion of individuals recovering from COVID-19 do not fully return to their baseline health and instead go on to develop (PASC).
Inflammation during early SARS-CoV-2 infection has been associated with adverse patient outcomes, especially among individuals hospitalized with COVID-19.
A growing body of evidence suggests that the inflammation that occurs during the acute phase of infection can last for weeks to months.
For example, convalescent plasma has been found to exhibit increased levels of the inflammation markers interferon (IFN)-gamma and monocyte chemoattractant protein (MCP)-1, as compared with pre-pandemic plasma.
While the clinical implications of persistent inflammation have been established for some chronic infections, including HIV, they are less well understood for acute infections such as SARS-CoV-2, says Peluso and colleagues.
“Among those recovering from COVID-19, there are limited data on immunologic trends over time and in association with ongoing clinical symptoms,” writes the team.
What did the current study involve?
In a prospective cohort study of 121 individuals with a history of documented SARS-CoV-2 infection, the researchers compared blood plasma levels of inflammation markers between individuals with and without PASC during the early recovery period (less than 90 days since symptom onset) and the late recovery period (beyond 90 days since onset).
Seventy-three (60%) of the 121 participants reported one or more symptoms at the late recovery timepoint, with the most common symptoms including memory or concentration problems (57%), fatigue (56%), shortness of breath (38%), and a loss of sense of smell (37%).
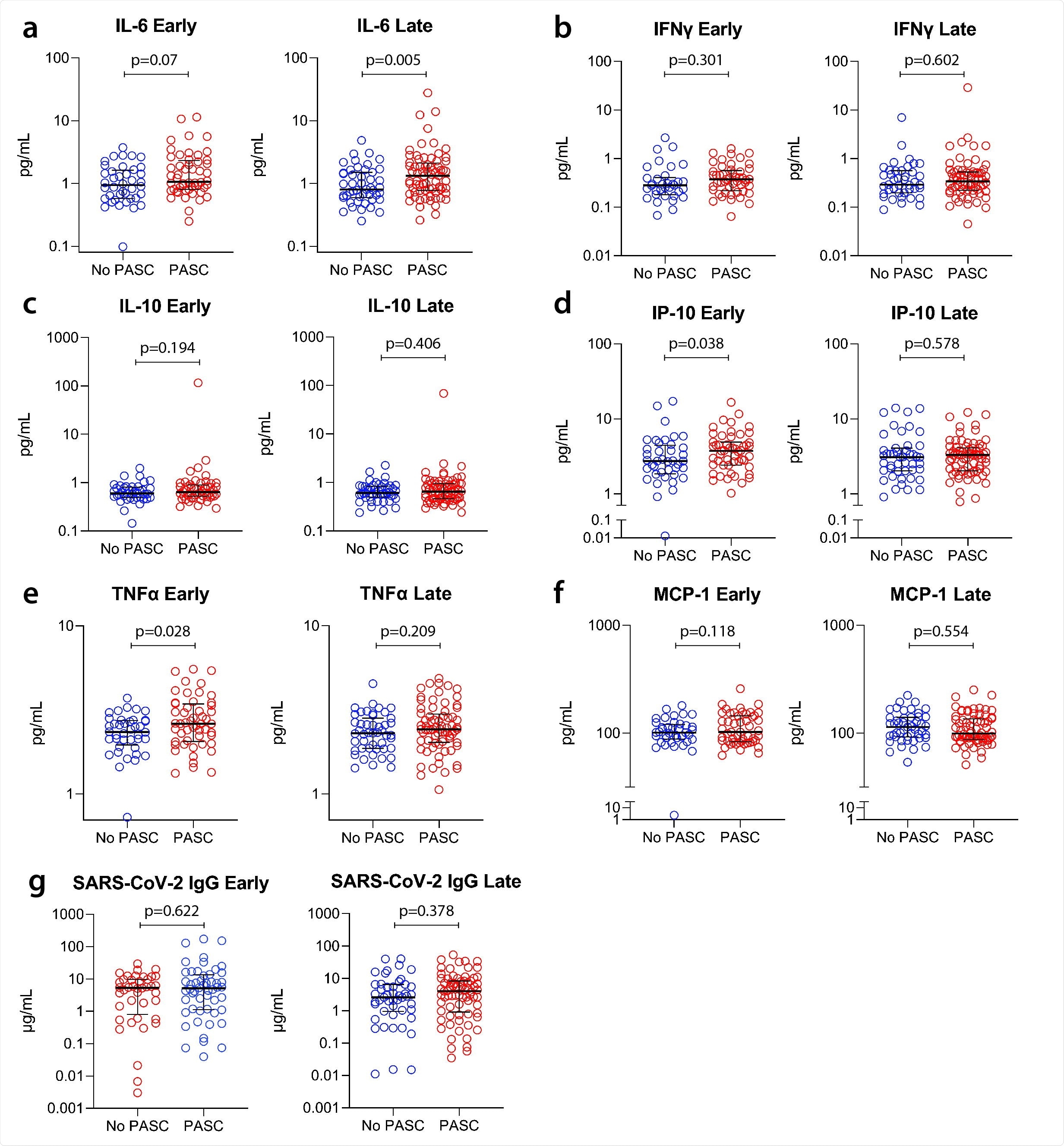
During early recovery, levels of TNF-alpha and IP-10 were an average of 14% and 28% higher, respectively, among those who went on to develop PASC, compared with those who did not develop PASC.
The level of IL-6 was also an average of 29% higher during early recovery among individuals who developed PASC, with this trend becoming more pronounced during late recovery. The IL-6 level was an average of 44% higher among those with versus without PASC during the late recovery period.
“A better understanding of these pathogenic processes is critical”
“We identified several biomarkers – particularly IL-6 and TNF-alpha – that differ during early and late recovery among those who continue to experience symptoms at a median of 124 days following infection,” says Peluso and colleagues. “Individuals with persistent symptoms were likely to demonstrate higher levels of markers of inflammation and immune activation during the first 90 days of COVID-19 recovery.”
The researchers say that these observations may inform about the biological pathways that lead to PASC and facilitate the identification of potential therapeutic strategies.
“A better understanding of these pathogenic processes is critical for identifying therapies to treat and/or prevent this condition among the millions of individuals who have recovered from acute SARS-CoV-2 infection,” concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Peluso M, et al. Markers of immune activation and inflammation in individuals with post-acute sequelae of SARS-CoV-2 infection. medRxiv, 2021. doi: https://doi.org/10.1101/2021.07.09.21260287, https://www.medrxiv.org/content/10.1101/2021.07.09.21260287v1
- Peer reviewed and published scientific report.
Peluso, Michael J, Scott Lu, Alex F Tang, Matthew S Durstenfeld, Hsi-en Ho, Sarah A Goldberg, Carrie A Forman, et al. 2021. “Markers of Immune Activation and Inflammation in Individuals with Postacute Sequelae of Severe Acute Respiratory Syndrome Coronavirus 2 Infection.” The Journal of Infectious Diseases 224 (11): 1839–48. https://doi.org/10.1093/infdis/jiab490. https://academic.oup.com/jid/article/224/11/1839/6376537.