Virtual reality (VR) is the name given to the technology that allows a user to simulate a situation or experience of interest, using a VR headset, within an interactive but computer-generated environment. The simulation is immersive and may require the use of special 3-D goggles with a screen, or gloves that provide sensory feedback, to help the user learn from experience in this virtual world.
 Image Credit: Fit Ztudio / Shutterstock.com
Image Credit: Fit Ztudio / Shutterstock.com
Virtual reality is used in many areas of healthcare, in a variety of applications. These include medical training, for both doctors in training and students, patient treatment, medical marketing, and educating people about a disease or medical condition or process. It is estimated that the global market for VR could be more than ~4 billion dollars by 2020.
Medical training
Current medical training has shifted from the rote memorization of facts to imparting skills to use facts to arrive at a proper management strategy when faced with a given patient. This training includes problem-oriented learning, communication skills, and VR-based learning.
Any kind of medical situation can be simulated using VR, to allow the students to deal with it as in real life. This is followed by feedback and debriefing, to allow them to learn from their mistakes, if any. The cheapness of VR systems and the fact that faculty are not required to be present makes access more flexible and broad-based.
VR can be used to help medical professionals visualize the interior of the human body, thus unveiling otherwise inaccessible areas. For one, the dissection of cadavers, which was a norm for every new medical student, has given way to the study of human anatomy via VR.
Computer graphics have made it possible to recreate any part of the body in great detail, with extreme faithfulness to reality. Moreover, training can be offered using scenarios that closely mimic common surgical situations.
For instance, real-life surgical procedures can first be filmed from multiple angles with stunning quality and then combined with models of the body site being operated on, to allow the student to ‘operate’ in VR.
Understanding how fractures occur and are aggravated in real life is of immense use to orthopedic surgeons in training. Since minimally invasive surgery is of great benefit in reducing operative costs, complications and recovery time, simulation-oriented VR-based training is a very effective method of transferring skills to would-be laparoscopic surgeons.
In fact, the American Board of Internal Medicine (ABIM) pronounced the superiority of this type of training before attempting to treat patients in real life, given that it has been effective in imparting standardized instruction in invasive monitoring and mechanical ventilation.
The same is the case with learning to apply sutures in the operating room, as well as in orthopedic surgeries, where the use of VR with tactile and sensory feedback is found to be both safe and reproducible, as well as inexpensive, compared to conventional training.
The high cost of such VR environments, including the cost of monitors, programming, and the other tools required for such training, may perhaps be offset by including a greater number of students in each program. However, the results are clearly superior, with more accurate knowledge resulting from the use of VR.
Treatment of patients
Virtual reality is useful in planning complex operations beforehand, such as neurosurgical procedures, as it helps the surgical team walk through the whole surgery and rehearse their planned intervention.
This maximizes safety by minimizing surprises. The data is compiled from CT, MRI and ultrasound scans, which are complemented by VR and haptics. The reconstruction looks and feels like the actual patient when in surgical surroundings.
VR is also crucial in surgical robotics, which depends on a robotic arm controlled by a human surgeon at a console. The surgeon depends on the camera positioned within the body to provide a view of the area being operated on. However, tactile and sensory feedback is also important during surgery, and a fair imitation may be provided by VR in their absence.
Mental health patients with phobias, for instance, also find VR very helpful, as do their therapists. For instance, to treat clients with agoraphobia, or acrophobia, a corresponding situation may be recreated in the therapist’s own center, to help the client face it little by little. This is also the case with post-traumatic stress disorder (PTSD).
Thus, VR offers the practical benefits of on-site coaching, with progressive exposure therapy filled in with the actual sensory experience of the trigger situation to increase the power of the technique.
This is coupled with the convenience and privacy of a therapy center, at far lower costs in terms of time, travel and tiredness. It can also be repeated as required, in increasing order of difficulty.
Pain management
Virtual reality is also found to be useful in the work of relieving pain and rehabilitation of patients with severe pain, such as those who are recovering after having received a skin graft, during the daily cleaning of burns wounds, or to make daily injections more bearable for children.
Immersive VR has been found to effectively distract and thus relieve the pain of such patients, especially when the use of anesthesia or sedation is contraindicated.
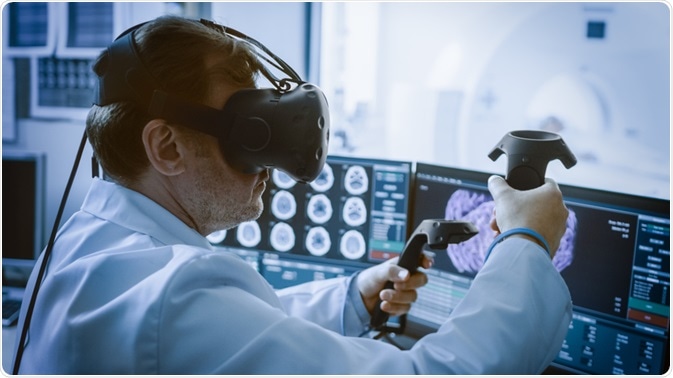 Image Credit: Gorodenkoff / Shutterstock.com
Image Credit: Gorodenkoff / Shutterstock.com
Physical therapy and rehabilitation
During physical therapy, too, virtual reality allows shortening of recovery times by making it easier for patients to do their exercises. This is because the VR turns the patient’s attention away from the pain, providing an absorbing alternative reality that simultaneously entrances, motivates and encourages them to complete the activity.
Thus, patients who are recovering from a stroke may be able to practice specific movements without the risk of further injuring themselves by a fall. This will boost their confidence when it comes to actually moving around in their real-life setting.
Addiction
Medical virtual reality can also be useful in helping with recovery from addiction to substances, using gradual exposure techniques along with coaching on how to respond to the addiction urges. The use of the patient’s own environment in the simulated situation may help practice resisting common triggers before being exposed to the real thing.
Health education
Again, when patients need to understand their medical condition, virtual reality comes to the rescue by providing an understandable and detailed reconstruction of the organs and tissues of interest. This helps the patient to grasp the principles of the treatment, increasing satisfaction with the intervention.
The actual effects of certain lifestyle practices and noxious substances on the body may also be best communicated by VR, such as the growth of certain tumors, obesity and related metabolic dysfunctions, and the impact of smoking or drinking on lung and liver function, respectively.
Fitness
Virtual reality has been used in numerous fitness apps to promote physical activity every day by making it more fun. They either gamify physical exercise, provide goals and rewards, give feedback on the movements, or just make it more enjoyable by immersing the user in a beautiful landscape.
Marketing
Marketing is a huge part of modern medicine. Virtual reality makes it possible for doctors to share their knowledge with patients, and for patients to communicate their experience without words to their doctors, allowing for powerful and effective communication, enhanced awareness of disease, and of potential interventions.
VR is still in its early days as far as medical applications are concerned. In the future, VR is likely to be increasingly used to enhance the safety and efficacy of surgical procedures, especially those which are minimally invasive or non-invasive, and to better understand the intricacies of the human body.
On the other hand, there are no large-scale trials showing its benefits, while it may possibly be disorienting and addictive. Also, if poor-quality VR tools are used, the learning may be inferior and possibly dangerous for the patient.
References
Samadbeik, M. et al. (2018). The applications of virtual reality technology in medical groups teaching. Journal of advances in medical education & professionalism vol. 6,3 (2018): 123-129. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6039818/
Pottle, J. (2019). Virtual reality and the transformation of medical education. Future healthcare journal. https://dx.doi.org/10.7861/fhj.2019-0036. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6798020/
Müller-Wittig W. (2011) Virtual Reality in Medicine. In: Kramme R., Hoffmann KP., Pozos R.S. (eds) Springer Handbook of Medical Technology. Springer Handbooks. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-540-74658-4_63. https://link.springer.com/chapter/10.1007/978-3-540-74658-4_63.
Li, L. et al. (2017). Application of virtual reality technology in clinical medicine. American journal of translational research vol. 9,9 3867-3880. 15 Sep. 2017. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5622235/
Further Reading
Last Updated: Jan 11, 2021