A food allergy refers to an adverse reaction of the body's immune system to certain foods which are perceived to be a danger to the body. While most allergic reactions are mild and easily managed, these responses can also be serious and life-threatening, causing anaphylaxis and even death.
It is estimated that up to 6 percent of children under the age of five have a food allergy, whereas food allergies only affect 3-4 percent of adults. However, the prevalence of food allergies is on the rise and is thought to account for around 150-200 deaths per year. This article aims to describe the role of the immune system in food allergies, as well as the symptoms, diagnosis, and treatments available.
Skip to:
What is a food allergy?
Food allergies occur when the immune system identifies the proteins contained within food as foreign bodies and mounts an attack in the same way as it does when microbes and bacteria are detected. The immune system releases several chemical mediators such as histamine that lead to symptoms of the allergy. Most commonly, food allergies are triggered by the immunoglobulin E (IgE) antibody.
Common food allergies found in children include egg and milk allergies, whereas adults are more likely to be allergic to fruit and vegetables. Nut allergies, on the other hand, are seen commonly across all age groups.
Extreme food allergies can cause a severe allergic reaction known as anaphylaxis. Symptoms of anaphylaxis include difficulty in breathing, swelling inside the airways and larynx that can cause choking, dizziness and even loss of consciousness. In addition, blood pressure can fall rapidly leaving the skin cold and clammy and sending the patient into shock.
The best way to prevent an allergic reaction is to avoid the food item completely. Food and related products, as well as cosmetic labels, should be read carefully to see if the ingredients contain any food that a person is allergic to.
Food allergy is sometimes confused with food intolerances such as lactose or gluten intolerance which may cause abdominal pain, bloating or diarrhea. Food intolerance is less severe than a food allergy, as the immune system does not respond as vigorously if food is consumed and the person is intolerant.
Over the past decade, awareness of food allergies has increased substantially across Europe and the US, with food and cosmetic products legally needing to display all ingredients including common allergens in bold. Many restaurants also cater to avoid usage of certain food allergens in their menus, as well as many schools and workplaces adhering to strict food regulations in terms of what can and cannot be brought in.
Despite this, deliberate bullying of children with food allergies still exists affecting the quality of life of affected children. Cases of inadvertent subjection of children to food allergens at parties have been reported.
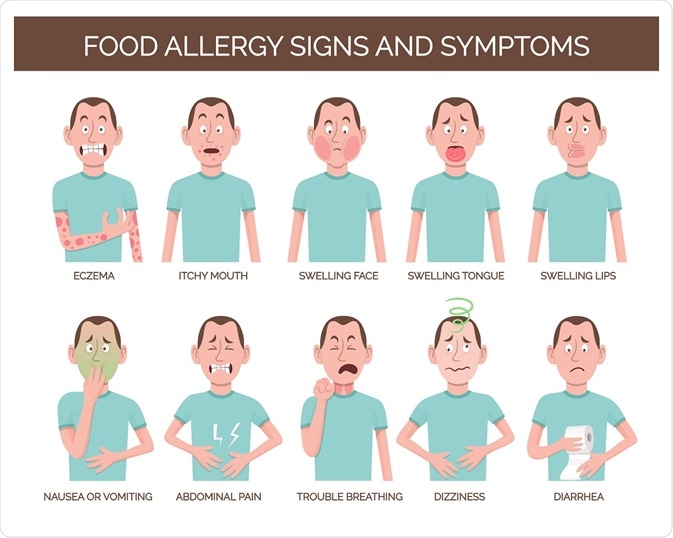
Food allergy signs & symptoms
Consuming food that you are allergic to may result in an immediate onset of symptoms, or may only occur after repeated exposure to the food item (known as a delayed allergic reaction). Food allergies are most commonly mediated by the antibody immunoglobulin (IgE) and symptoms usually appear within a few seconds or minutes.
Common symptoms of food allergies can include:
- A skin rash (called urticaria) that appears raised and is severely itchy. Urticaria may be confined to one part of the body (typically a rash on the face) or spread all over it. In some individuals, the skin may only become red, itchy, and not raised.
- Angioedema or swelling of the eyes, lips, mouth, throat, palate (roof of the mouth), tongue and face.
- Constriction of the throat and difficulty in breathing.
- Swelling of the larynx or voice box that may lead to hoarseness and further difficulty in breathing. There may be a cough and a tightness of the chest due to constricted breathing and some patients may develop an audible wheeze.
- Nausea, vomiting, and diarrhea along with abdominal bloating, pain and cramps, with blood or mucus present in stools.
- Flu-like symptoms including runny nose, nasal blockage, sneezing and watering or redness of the eyes (allergic conjunctivitis).
- Dizziness.
- Delayed allergic reactions may include atopic eczema that leads to the formation of itchy, dry and cracked skin lesions.
- Babies with food allergies (especially milk) cry due to colic and abdominal spasms. The baby may have diarrhea and there is usually a redness or nappy rash around the anus and the genitals.
 insemarDrawings | Shutterstock
insemarDrawings | Shutterstock
If a person experiences anaphylactic shock (the most severe allergic reaction), symptoms will typically include:
- Difficulty in breathing due to narrowing of the airways and swelling of the larynx
- Rapid heart rate
- Rapid fall in blood pressure causing dizziness or lightheadedness and cold, clammy skin.
- Itchy urticaria and angioedema
- Severe apprehension or anxiety
- Unconsciousness
Anaphylaxis is a life-threatening medical emergency and requires immediate attention. Usually, people who have known food allergies will carry adrenaline (epinephrine) injectors (epi-pens) to be administered immediately at any sign of anaphylaxis.
What causes food allergies?
Normally, the immune system defends against microbial infection by producing specific proteins or antibodies that can identify and then "recognize" the proteins displayed on microbial cell walls. Once identified by the antibodies, the microbes are targeted by chemicals released during an immune response.
The antibody that most commonly misidentifies proteins in food as invasive agents is immunoglobulin E (IgE). It stimulates the release of several chemical immune mediators including histamine within seconds of contact or ingestion of the allergen.
Histamine leads to the swelling and dilation of the small blood vessels located in the face, lips, mouth, throat, airways, and the larynx, causing swelling or tightening of these areas. Histamine also induces an itching sensation as well as increased mucus production in the mouth.
Non-IgE mediated allergic responses are often involved in a delayed allergic response that may occur hours after consuming the allergen. Further complications can arise when the allergic response is a combination of IgE and non-IgE mediated response. Food allergies often run in families but may also be found in individuals with no family history of food allergies.
According to the United States Food and Drugs Administration (FDA), eight main types of food trigger an allergic reaction:
- Eggs
- Milk
- Fish
- Shellfish
- Peanuts
- Nuts
- Wheat
- Soybeans
Certain fruits and vegetables including pears, apples, peaches, kiwi fruit, carrots, potatoes, parsnip, and celery can also trigger an allergic reaction (referred to as Oral Allergy Syndrome), as can commonly used food additives such as sulphite or benzoic acid. Other food allergens include those found in mustard, sesame seeds, and soya. Rarer allergies can be due to spices such as coriander and garlic, and very rarely to meat or gelatine.
 THPStock | Shutterstock
THPStock | Shutterstock
How are Food Allergies Diagnosed & Treated?
Diagnosis of food allergies
Diagnosing food allergies involves a detailed evaluation of a patient's history of symptoms and their association with the intake of a specific food type. Blood or skin prick tests or food elimination diets may also be used to narrow down the possible triggers of allergy.
Food diary
A detailed examination of past food exposure and the appearance of symptoms is carried out. The person with the allergy or their parents (in the case of children) will be asked to maintain a diary recording the frequency, duration, and severity of symptoms and the time they take to appear along with details of all foods consumed.
Family history
Any family history of similar food allergies or other allergic conditions such as asthma or eczema are also noted. Information on whether a child was breast or bottle fed may also be obtained as breastfed children are less likely to develop food allergies. In cases where the patient is a child, growth and development are assessed.
Food elimination
A food elimination diet may be used to check whether a certain food item is causing the allergy and a diet that completely lacks the suspected food item is followed for two to six weeks, after which it is gradually reintroduced. If the symptoms reduce or disappear when the food is withdrawn, only to reappear when it is included again, the food allergy is confirmed. This method should be carried out under medical supervision to avoid medical emergencies such as anaphylaxis.
Skin prick test for IgE
For people with an IgE-mediated food allergy, a skin prick test is recommended. Drops of highly diluted food items are placed over the forearm and the skin pierced using a tiny needle to see whether an allergic response such as redness ensues. Again, adequate medical support should be available to accommodate for any medical emergencies. Blood tests to detect antibodies to specific antigens may also be performed.
Treatment of food allergies
Medications used to treat allergies targeting the chemical mediators of adverse immune reactions, such as targeting histamine are commonly used. Antihistaminic agents are useful for treating mild-to-moderate allergies. However, during anaphylaxis, adrenaline (epinephrine) is required to reverse life-threatening airway swelling.
Histamine is one of the major mediators of allergic reactions and is released from several of the body's immune cells in response to a food allergen (a protein or compound present in food). Histamine release can cause itchy skin rashes, wheezing, constriction of airways, and a red and runny nose and eyes. Some antihistamines used to treat allergic reactions to foods include cetirizine, levocetirizine, azelastine and loratadine.
Some antihistamines cause drowsiness because they pass into the nervous system. Thus, driving and operating heavy machinery while taking them should be avoided. However, there are several antihistamines with selective action on peripheral histamine (outside the nervous system) that can be used for food allergy treatment while minimizing side effects.
Anaphylaxis is mediated by inflammatory mediators and cytokines, causing the severe symptoms associated with it. Adrenaline can act by narrowing the blood vessels and raising the blood pressure as well as by widening the airways to ease difficulties in breathing. Adrenaline needs to be administered immediately after detection of anaphylaxis.
People prone to anaphylaxis on exposure to certain foods may keep an auto-injector with prefilled adrenaline within easy reach. There are three types of auto-injectors including the EpiPen, the Anapen and the Jext. The injection of adrenaline is achieved by removing the safety cap and placing the injector against the outer thigh at a right angle and pressing down on the injector button for around 10 seconds. The injection can be administered through clothing to save time.
Trial treatments currently under investigation
At present, several trials of anti-IgE medications for food allergies and conditions such as asthma are underway. Oral immunotherapy has been increasingly used to help desensitize patients with food allergies. In this therapy, small doses of the allergen are placed sublingually (under the tongue). Over time, the doses are increased, allowing the body to build up a tolerance to the food.
The basis for this therapy is the same as that explaining why early exposure to common allergens (such as peanuts/peanut butter) during childhood or even infancy can reduce the likelihood of allergy development.
Key takeaways
- Careful avoidance of susceptible food allergens by a dietary change (e.g. elimination of all traces of peanuts) can be used to prevent future allergic reactions.
- Raising awareness with friends, family, workplace/school environments can further prevent accidental subjection to triggering foods.
- Carrying medication such as inhalers, epi-pens and anti-histamines can effectively reduce the symptoms should you come into contact with a food allergen.
Further Reading
Last Updated: Jan 11, 2023