Many people today think they have a penicillin allergy and cannot be treated with this drug family. However, recent studies show that having a history of penicillin allergy is not a reliable indicator of this condition in the current time.
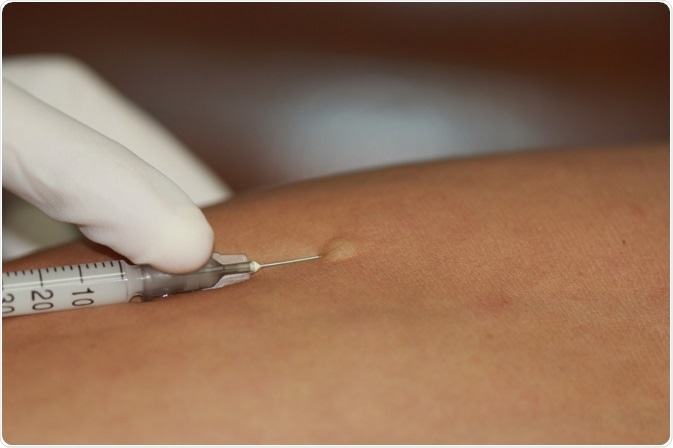
Image Credit: enuengneng/Shutterstock.com
True penicillin allergy is rare, occurring in only 1-5 of 10,000 cases treated with penicillin. In fact, in 9 out of 10 cases, allergy testing shows that the supposed allergy is absent.
The reasons for this phenomenon include the documented fact that even true allergies can wane over time, and secondly, many symptoms of intolerance such as nausea are wrongly labeled as an allergy.
Among over 3 million patients, 6000 patients reported a history of allergy symptoms after their first prescription of penicillin. Just under half were prescribed the drug again, according to the UK General Practice Database.
This is often because penicillin is included in a combination product prescribed by brand, without the doctor recognizing its presence. This group had over 11 times the risk of allergy to penicillin as the general population. Even so, less than 2% of these patients developed an allergic event.
However, even though very uncommon, true penicillin allergy is the most important adverse reaction to this drug, because it can cause respiratory obstruction and death.
What is Penicillin?
Penicillin is a commonly used antibiotic drug, from a family, called the beta-lactams. Another set of drugs from this class is called the cephalosporins.
Penicillin was originally discovered from the humble bread mold, Penicillium notatum, in 1928, by the Scottish physician Alexander Fleming.
The drug was soon tested severely in the second world war when it was used to treat wounded soldiers. The near-miraculous results achieved in the field of infection control elevated the drug to a larger-than-life pedestal.
Today, the penicillins include 15 or more compounds, including ampicillin, amoxicillin, amoxicillin-clavulanate, and methicillin. They are prescribed for a wide range of infections, including streptococcal infections of the throat, sinus infections, and dental infections.
What Is True Penicillin Allergy?
A true allergy to penicillin is caused by a mistaken reaction to the drug by the immune system which recognizes it wrongly as a harmful substance.
Penicillin G is the drug with the highest reported rates of drug allergy, especially when used as procaine penicillin – because procaine itself causes hypersensitivity.
Both acute and subacute penicillin allergy are observed. The first is mediated by IgE and the second by IgG antibodies.
Image Credit: joel bubble ben/Shutterstock.com
Symptoms of True Penicillin Allergy
The most severe form of IgE-mediated allergy is anaphylaxis, caused by vasodilation and the resulting sudden drop in blood pressure, along with dyspnea and wheezing due to airway constriction.
The clinical signs such as urticaria, angioedema (swelling of the lips, throat and/or face), itching, and sometimes abdominal pain, diarrhea, nausea, and vomiting. It occurs most commonly after parenteral administration and is rarely seen with oral or skin prick exposure.
The mechanism of anaphylaxis is the systemic exposure of already existing IgE antibodies attached to mast cells, causing them to crosslink. This results in the degranulation of many mast cells at the same time, releasing histamine and other chemicals that act on the blood vessels all at once.
Milder reactions may occur, such as itching, skin redness, rash, or swelling.
A similar reaction may occur without involving IgE antibodies and is called an “anaphylactoid” reaction.
Subacute penicillin allergy occurs with the binding of the drug to already existing IgG antibodies, which activate the complement system. This, in turn, sets inflammation in motion, producing fever, urticaria, and joint pain or inflammation.
Does Penicillin Allergy Last for Life?
Up to 50% of people with penicillin allergy become tolerant to the drug over time, and this rises to 80% over 10 years. Thus, people who have had reactions 10 or more years ago should be re-assessed with a skin test.
If antibiotics are needed and penicillin would be by far the best option, desensitization may be offered under strict medical supervision.
A family history of penicillin allergy is not a contraindication to penicillin use. Similarly, if a patient with a history of allergy to penicillin has since taken penicillin without incident, the drug may be prescribed again.
The absolute contraindications to penicillin use are a history of severe drug reactions with systemic symptoms such as Steven-Johnson syndrome, toxic epidermal necrolysis, or drug reactions with eosinophilia, or if there is a history of anaphylaxis.
Is Skin Testing for Penicillin Allergy Useful?
While an acute IgE-mediated reaction rules out a repeat administration of penicillin, a history of subacute or nonspecific allergic reactions does not. However, practically, these cannot be distinguished without skin testing.
Skin testing is fast, effective, and safe, and can provide an accurate diagnosis of true penicillin allergy when performed by an allergist or immunologist in a properly equipped center.
Various dilutions of two forms of penicillin are used, namely, the major determinant penicilloylpolylysine and commercially available penicillin G.
These are closely related to those found in the blood of patients treated with the drug are administered, first through minute skin pricks, and then placed just under the skin, in very small amounts.
If the test is negative, the patient is given oral penicillin as a challenge dose as well. It usually takes 2-3 hours for the whole procedure, including the observation period.
The skin test has a negative prediction value of over 95%, but nearer 100% if the oral challenge is also performed.
The relative unavailability of these dilutions at lower levels of healthcare is the primary reason why skin testing is so little used to correctly identify those patients who truly have a true penicillin allergy.
A positive skin test means the occurrence of a red wheal. This means that penicillin cannot be administered, neither can other beta-lactam antibiotics which often show cross-reactivity with it.
The patient and healthcare provider should be alert to signs of allergy, such as dizziness, a rapid or weak pulse, slurring of speech, bluish discoloration of the skin, lips, and nails in the fair-skinned, nausea, vomiting or diarrhea, to avoid rapid deterioration to impending cardiovascular collapse. Adrenalin and corticosteroids are the drugs of choice in this situation as they quickly arrest the hypersensitivity reaction.
If the skin test is negative, the risk of penicillin allergy is that of the general population. Thus, the universal use of skin testing in all patients suspected to have a penicillin allergy, from their history, could help extend the use of this effective but relatively inexpensive drug.
This, in turn, could prevent the widespread use of more broad-spectrum antibiotics, that could introduce multiple drug resistance, as well as being less effective and more costly.
Cephalosporins And Penicillin Allergy
Can cephalosporins be used with a history of penicillin allergy? The answer has conventionally been to point to the 10% incidence of cross-reactivity between the two drug families. However, cephalosporin allergy is much less common even than penicillin allergy.
Researchers now think that the extent of cross-reaction depends on the presence of similar side chains between penicillin and the cephalosporin in question.
Thus, the second and third generation of cephalosporins may be less likely to cross-react with penicillin than the first generation, and less likely even than unrelated drugs.
References and Further Reading
Further Reading
Last Updated: May 4, 2020