Human scabies, which involves the transmission of an ectoparasitosis to humans via direct or indirect skin contact, is caused by Sarcoptes scabiei var. hominis, which is a mite that only targets human beings. Skin eruption with classical scabies is attributable to both the infestation and a hypersensitivity reaction to the mite.

Image Credit: SciePro / Shutterstock.com
Scabies generally represents an annoyance due to itching, rash, and its ability to spread effortlessly, although there is a looming possibility of superinfection, especially with Streptococcus pyogenes. The most common sites of infestation are the fingers and the wrists; however, in older individuals, the infection may manifest as a diffuse truncal eruption.
Characteristic clinical presentation
Scabies has three basic clinical presentations: classic, crusted, and nodular.
Classic scabies is the most common form with notable symptoms of severe pruritus, which is often worse in the evening, irritability, fatigue, and, in some patients, fever from aforementioned secondary infections. The classic sign of scabies is the burrow, which is defined as a serpiginous grey line in the skin formed by the digestive secretions from the advancing mite.
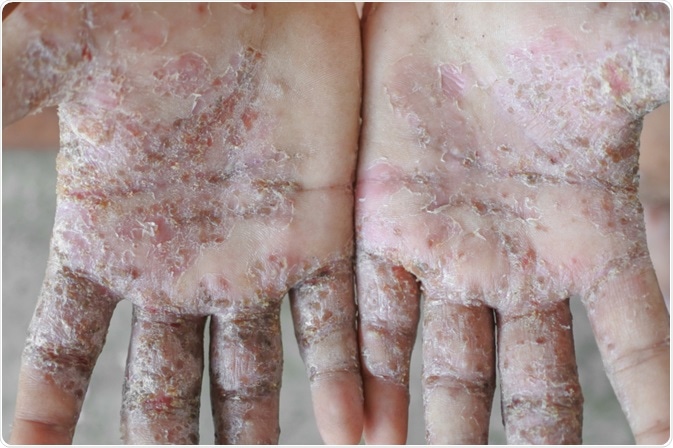
Image Credit: phugunfire / Shutterstock.com
Crusted scabies, which is also known as Norwegian scabies, occurs in immunocompromised patients, such as those on long-term immunosuppressive therapy or those with human immunodeficiency virus (HIV) or human T-cell lymphotropic virus type 1 (HTLV-1). This presentation of the disease is described as psoriasiform dermatitis, frequently associated with hyperkeratotic skin crusts that are limited to the scalp, face, nails, or soles.
Nodular scabies is an uncommon variant of the disease characterized by extremely pruritic reddish-brown nodules up to two centimeters (cm) in size that are typically found on the genitalia, groin, buttocks, and axillae. Those nodules are considered to be the result of hypersensitivity reactions to mite products.
A more prompt pruritic allergic reaction is frequently observed, in a patient who has previously had scabies. Erythematous papules develop at the tunnel entry sites and pruritic papules may appear as part of an urticarial reaction; therefore, not every itching spot contains a mite.
SCABIES, Causes, Signs and Symptoms, Diagnosis and Treatment.
Diagnosis
Even though scabies should be considered for any patient who presents with a pruritic dermatosis, clinicians must evaluate a wide array of diagnostic possibilities. The diagnosis rests largely on the adequate history and examination of the patient, as well as on the history of the family and close contacts.
Confirmation of the diagnosis requires the isolation of the mite, eggs, or mite feces. The simplest technique requires scraping the skin over the burrow with a scalpel blade, smearing the scrapings on a glass slide, and applying a drop of mineral oil to the debris.
After applying a coverslip, diagnostic findings of mites, eggs, or mite feces under the microscope can be easily acknowledged. An average adult female mite is between 330 and 450 micrometers (µm) in length.
Atypical or otherwise complex presentations may necessitate the use of more definitive diagnostic modalities, such as microscopic examination of skin scrapings prepared with potassium hydroxide, high-resolution digital photography, dermoscopy, or skin biopsy.
Alternative methods that can be applied include the burrow ink test, in which suspicious papules are marked with ink and then wiped off with an alcohol pad to remove ink left on the surface. A positive result occurs when the ink tracks down the mite burrow, forming a characteristic zigzagged line visible to the naked eye.
Studies of advanced diagnostic tests, such as polymerase chain reaction (PCR) or enzyme-linked immunosorbent assay antibody (ELISA) detection, are underway. Genotypic differentiation among the populations of Sarcoptes scabiei and worldwide comparison of genotypic data in order to construct a phylogenetic tree is also feasible.
References
Further Reading
Last Updated: Apr 30, 2021