Hemochromatosis is a disorder in which iron overload occurs in the body, causing iron toxicity. This leads to storage of iron within the heart, the liver, and the pancreas, among other tissues, damaging them and causing organ failure if it remains untreated.
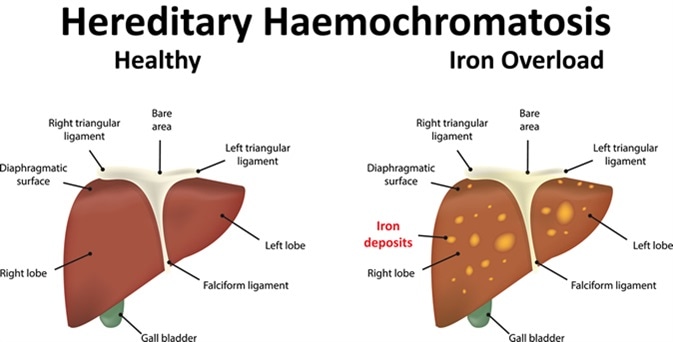
Hereditary Haemochromatosis. Image Credit: Joshya / Shutterstock
Types
Both primary and secondary hemochromatosis can occur. Primary or hereditary form, it is inherited and primarily results due to hepcidin disruptions in most cases. Hepcidin is a hormone secreted by the liver which promotes iron absorption. Secondary hemochromatosis may be due to iron deposition in damaged tissue, or due to the presence of excessive iron in the body because of repeated transfusions or iron administration in conditions such as anemia or thalassemia.
Hereditary hemochromatosis is classified as follows:
- Type 1 which is the most common form with symptoms appearing between 50 and 60 years in men, and after 60 years in women (or after menopause). It affects about a million people in the USA
- Type 2 or juvenile hemochromatosis in which the onset occurs in childhood or adolescence.
- Type 3 which sets in before the age of 30 but after childhood is over (15 years or so).
- Type 4 which is also called ferroportin disease and also begins in adult life.
Neonatal hemochromatosis is an autoimmune disorder in which the fetus is affected in utero by rapidly increasing levels of iron.
Mayo Clinic: William Palmer, M.D. - Hereditary Hemochromatosis
Causes and Risk Factors
Mutations in several genes produce the clinical outcome of hemochromatosis, notably the HFE gene in Type 1 disease which affects the pattern of iron absorption from the gut. The first three types are autosomal recessive in inheritance, while the fourth has an autosomal dominant pattern.
In most cases (90%), the gene mutation does not produce clinical disease. In recessive disease, if only one gene is abnormal, the individual carries the disease but is not affected. If both parents pass on one copy of the gene to the offspring, the child will have hemochromatosis.
Risk factors for hereditary hemochromatosis include the presence of two copies of the abnormal gene, a positive family history, such as a parent or a sibling with the disease, being descended from a family of North European origin rather than of African, Hispanic or Asian origin.
Symptoms
The symptoms are initially vague, such as weakness, tiredness, abdominal or joint pain, and loss of libido. However, at times, there are many people with hereditary hemochromatosis in which symptoms generally don’t appear. As the condition progresses, damage to tissues results in arthritis, diabetes, heart muscle damage, skin bronzing, and liver damage.
Environmental factors interact with lifestyle and genetic factors to determine the rate of progression. The final outcome in untreated cases is heart failure, liver failure, failure of reproductive organs, and full-blown diabetes.
Diagnosis and Treatment
The diagnosis rests on the evaluation of signs and symptoms using blood tests to detect a high level of iron, or the use of screening tests in a patient with a family history of this condition, or who is being tested for some other reasons such as arthritis, liver disease, diabetes, heart disease, or erectile dysfunction (impotence). The commonly performed tests are serum transferrin saturation and serum ferritin. Transferrin carries bound iron in the blood and is normally up to 45% saturated. Ferritin is the storage form of iron in the body and is measured if the transferrin levels are abnormally high. If both tests are repeatedly positive, genetic testing is required to confirm the diagnosis. Other tests are done to assess damage to organs such as the liver, heart, and pancreas, and may include imaging with MRI, biopsy and liver function testing.
Treatment is by removing blood from the body (phlebotomy) at scheduled intervals, to force the body to use up stored iron to make more blood, thus bringing down the levels of iron in the body. The removal of the blood ensures that the iron from its breakdown does not reenter the circulation. In some conditions such as anemia or heart diseasewhen blood removal is not practical, chelation therapy is performed to bind excess iron using a binding (chelating) agent, which converts the complex iron into a soluble one and results in its excretion via urine or stool.
Further Reading
Last Updated: Feb 26, 2019