Postpartum depression (PPD) is reported to occur in 10-15% of delivering women with an estimated 400,000 women affected annually in the US. It is the most common complication of childbirth and is a significant public health concern.
PPD has an insidious impact on the lives of families by affecting maternal-infant bonding, breastfeeding, child-rearing practices, and overall child well-being. A mother’s PPD has been shown to place their infants at risk of impaired cognitive and emotional development. Unfortunately, PPD is associated with both maternal suicide and infanticide.
Both the American Psychiatric Association: Diagnostic and statistical manual of mental disorders (DSM-5) and the International classification of diseases 10 (ICD-10) define Postpartum Depression (PPD) as a Major Depressive Episode (MDE) which occurs in the postpartum period. Because as many as 50% of major depressive episodes that present postpartum actually began during pregnancy, the DSM-5 allows the onset of the depressive episode to occur in pregnancy or within 4 weeks of delivery.
Postpartum depression is an episode of major depression, as opposed to the milder and much more common “baby blues” which occurs in 50-85% of postpartum women and is associated with mood lability, tearfulness, anxiety and sleep disturbance, but the affected women have minimal or no impairment in daily activities.
Why don’t many mothers want to take antidepressants to treat the symptoms of postpartum depression?
In addition to the general reluctance of patients to take any chronic medication, patient acceptance of the use of psychotropic medication for the treatment of PPD may be limited by maternal concerns regarding infant exposure through breastfeeding and the unknown future effects of such exposure. Another concern is the potential impact of medication side effects, particularly on late night child care.
A bigger concern is a women’s access to care for postpartum depression. There are significant barriers to a woman receiving appropriate care for her PPD. The first and most important issue is that depression must be identified by the patient or her physicians.
Women may not acknowledge that they are depressed for multiple reasons - they are occupied with the newborn care, they believe they have “baby blues”, they believe that their symptoms will improve on their own, and there is the stigma of the diagnosis of depression.
Another significant problem is that there is insufficient and incomplete screening for PPD. Finally there is the issue of access to an appropriate mental health specialist once PPD has been identified.
What non-drug solutions are currently available for mothers with postpartum depression?
Treatment options for PPD are currently limited to psychotherapy, pharmacotherapy, and electroconvulsive therapy (ECT). Psychotherapy is effective and may be appropriate in milder cases of PPD, but may be limited by the local availability of trained counsellors. Also PPD requires immediate intervention but there may be significant waiting times for access to therapy services.
Although there are no systematic trials of ECT in PPD, case literature supports its effectiveness in postpartum psychiatric states, on the other hand, ECT is an invasive medical procedure and requires general anaesthesia for its use.
ECT also has well-documented adverse effects, including headache, muscle pain, and memory deficits. In addition, recovery time from each ECT treatment may take several hours, which can limit the ability of a new mother to care for her infant.
Because physicians typically prescribe pharmacotherapy or ECT for more severe cases of PPD, the end result is that many women choose to expose themselves and their infant to the adverse effects of PPD rather than receive treatment.
Please can you outline Neuronetics’ recent trial evaluating the NeuroStar TMS? What did the study involve?
The primary objective of this trial was to evaluate the antidepressant effectiveness of acute treatment with the NeuroStar TMS Therapy System for women with major depressive disorder with postpartum onset. This was an open-label trial using NeuroStar TMS as a monotherapy.
The key inclusion criteria were women aged 18-50 with DSM-IV defined Major Depressive Disorder, and who had onset of current illness beginning during the third trimester or up to 6 months following live childbirth. The women were required to have moderate depression at baseline with a 17-item Hamilton Rating Scale for Depression (HAMD17) score ³18, and an Edinburgh Postnatal Depression Scale (EPDS) score ≥10.
Patients were treated for a minimum of 4 weeks to a maximum of 8 weeks. The goal of treatment was the remission of symptoms, defined as an EPDS (<10) and a HAMD17 (<11).
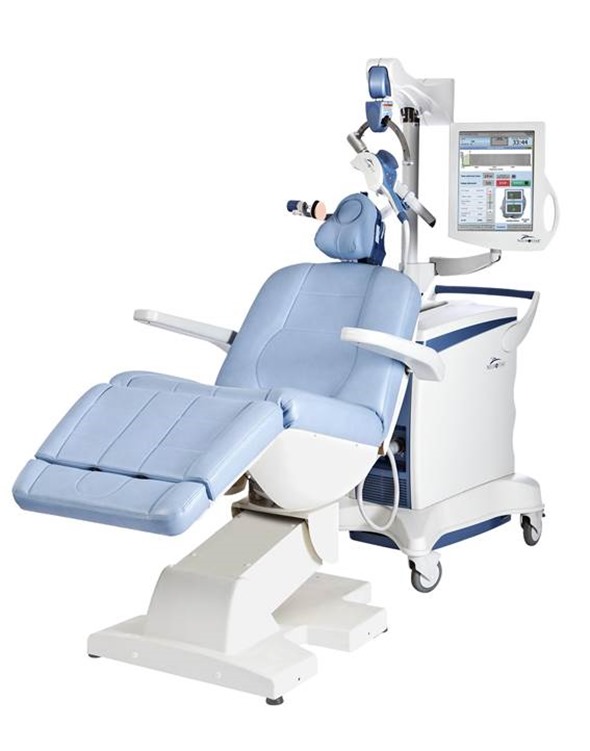
All treatments were performed using the NeuroStar TMS Therapy system using the standard treatment protocol of stimulation at 120% of motor threshold with a pulse frequency of 10 pulses per second using cycles of 4 seconds of active stimulation followed by 26 seconds of no stimulation for a total of 3000 pulses per treatment session.
What were the main findings of the trial?
We enrolled 26 patients at 8 sites of whom 19 patients were evaluable and are included in the final analysis. The average patient age was 29.9 years (range 19-39). 14 of the women achieved remission of symptoms by the end of 8 weeks of TMS therapy (EPDS<10); 12 of these 14 patients also met remission criteria by HAMD17 (<9).
There was also a substantial improvement in the mean change in score from baseline to end of acute treatment for both the clinician rated HAMD17 and the EPDS, at 59.3% and 69.3% respectively. Mean EPDS scores improved from 20.6 at baseline to 8.2 by the end of TMS treatment.
Importantly, there were no serious adverse events, treatment emergent mania, or suicidal ideation. The most common reason patients left the study prior to completion was difficulty complying with the treatment schedule.
What further research is needed to evaluate NeuroStar TMS therapy?
NeuroStar TMS is currently FDA cleared and has a CE mark for the treatment of Major Depressive Disorder in adult patients who have failed to receive satisfactory improvement from prior antidepressant medication in the current episode.
This pilot study shows that NeuroStar TMS was also effective as a monotherapy for the treatment of women with post-partum depression with 73.7% (14/19) of evaluable patients achieving remission of their depressive symptoms within 8 weeks of treatment.
Although this study provides health care providers with additional data regarding the use TMS for depression with postpartum onset, a larger cohort of women would likely need to be studied for a regulatory filing.
What do you think the future holds for managing postpartum depression?
We believe that the data from this study demonstrates the potential importance of a novel, non-invasive, non-drug treatment like NeuroStar TMS Therapy that allows women to pursue an option that avoids the medical concerns that lead them to choose not to pursue the currently available treatment options. This study is an important step in that direction.
Improved care for women with PPD will need to be multifaceted, with better screening for depression in the peripartum, better access to psychiatric services, and continued research on treatment options of PPD.
What’s your vision for Neuronetics?
Our vision at Neuronetics, Inc. is to implement innovative business strategies that will continue to meet the needs of our customers through the development and commercialization of non-invasive, cost-effective treatments that benefit both the people affected by psychiatric and neurological disorders, and the clinicians who care for them.
By working collaboratively with the clinical community as well as key stakeholders in the mental health space, we are dedicated to improving the lives of patients suffering from these chronic conditions through the delivery of clinically-proven safe and effective solutions.
As the established market leader in transcranial magnetic stimulation technology, we are committed to broadening NeuroStar TMS treatment accessibility for existing patient populations in need of a non-drug therapy option, including expanding access to adolescents with symptoms of Major Depressive Disorder (MDD).
In recent years, insurance coverage for patients has increased from 100 million to over 200 million covered lives, in both government and commercial insurance plans, providing more patients access to NeuroStar TMS Therapy than ever before in the United States.
Where can readers find more information?
Readers can visit www.neurostar.com, which includes a physician locator in which patients can find a doctor in their respective area, or call the Neuronetics Customer Service Center at (877) 600-7555 to learn more information about the treatment.
In addition, patients are encouraged to talk to their doctor to determine if treatment with NeuroStar TMS is right for them. NeuroStar TMS therapy is currently available at more 725 treatment centers in 49 states.
About Dr David Brock and Christopher Thatcher
 David Brock, MD, Medical Director, Neuronetics, Inc.
David Brock, MD, Medical Director, Neuronetics, Inc.
Dr. Brock is board certified in Neurology, with added qualification in cerebrovascular disease, and is also board certified in Neurocritical Care. He has over 15 years’ experience as an academic neurologist treating patients with complex neurological conditions. Prior to joining Neuronetics, Inc., he was a neurologist on the faculty at Thomas Jefferson University, where he was associate director of the Stroke Center and an Institutional Review Board chairman.
Dr. Brock has been an investigator in numerous clinical trials and has been published in the fields of stroke and neurocritical care. He is co-author of Gray’s Clinical Neuroanatomy: The Anatomic Basis for Clinical Neuroscience, which focuses on how knowing functional neuroanatomy is essential for a solid neurologic background for patient care in neurology.
 Christopher Thatcher, President & CEO, Neuronetics, Inc.
Christopher Thatcher, President & CEO, Neuronetics, Inc.
With more than 16 years of experience as a business leader in global medical device, equipment, pharmaceutical and healthcare product sectors, Mr. Thatcher drives business strategy at Neuronetics, Inc.
Prior to joining the company, Thatcher served as divisional vice president and business unit manager at Ametek, Inc., where he evolved the company’s medical device division, which led to significant increases in revenue. He has also served as president of corporate initiatives at medical device company Integra LifeSciences. He worked at Bausch & Lomb as vice president of the Americas sector and Canadian general manager, where he led the Canadian executive and management team.
He is a board member of for Micro Interventional Devices, an emerging medical device company in Newtown, Pennsylvania.