Aug 24 2017
Upon prolonged irradiation, human stem cells’ defenses are activated
Researchers from several Russian institutes, including MIPT, have found out how prolonged exposure to ionizing radiation affects human stem cells. They discovered that it causes a cell cycle delay, which leads to faster repairs of radiation-induced DNA double-strand breaks, with fewer errors. It is unclear what the health implications are, particularly how this affects the risk of developing cancer. The paper was published in Oncotarget.
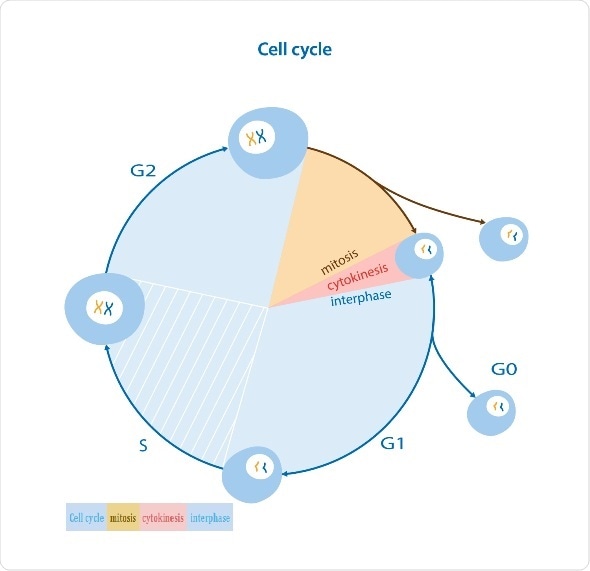
Cell Cycle. G0 is the resting phase when the cell does not undergo division. G1 refers to the phase in the cycle when the cell prepares for division by duplicating its constituent parts, with the exception of the chromosomes. During the S phase, the DNA is copied in a process duplicating all 46 chromosomes. G2 is the final stage in the preparation for division, or mitosis.
When statistics is no good
To a physicist, an ordinary flashlight or a portable radio is, among other things, radiation sources, and ionizing radiation is the proper scientific name of the high-energy rays that an ordinary person thinks of when they hear the word “radiation.” It comes in different types, including X-rays, gamma rays, and streams of various particles. Ionizing radiation is capable of turning neutral atoms and molecules into charged ions. The human body is inevitably exposed to radiation, with an average person receiving about 3 milligrays of natural background radiation annually. Moreover, one X-ray exam amounts to anywhere from 0.001 to 10 milligrays of additional exposure, depending on the exact procedure. That said, overexposure is dangerous: A dose of more than 1,000 milligrays received within a brief period of time causes acute radiation sickness.
To ensure radiation security, it is vital that we can accurately assess the risks posed by ionizing radiation. Studies of people that were exposed to radiation have only conclusively established the increased risk of cancer as a result of receiving a high dose of radiation. This led the regulating authorities to accept a linear model, under which low doses of radiation, too, increase the risk of cancer. However, experiments showed that low-dose radiation exposure either had no adverse biological effect or even was beneficial, as evidenced by prolonged life spans and less frequent cancer occurrence. Apart from that, the importance of the so-called dose rate should not be overlooked. Exposure to equal doses of radiation over shorter or longer time intervals has a different effect, with “slow” irradiation causing less harm. The extent to which dose rate affects the biological outcomes has been a cause of much debate. Because in a real-life setting, people are more likely to face prolonged exposure to low-dose radiation, it is crucial that we understand its effects.
DNA double-strand breaks
One of the negative effects of radiation is the formation of the so-called DNA double-strand breaks, in which both strands of the double helix are severed. Fortunately, the cell is capable of repairing damaged DNA. If one of the two strands is damaged, the other can be used to reverse this. However, in the case of a double-strand break, other — more error-prone — mechanisms have to be employed. Left unrepaired or misrepaired, such lesions can give rise to oncological diseases. This explains why research into the effects of radiation on living cells tends to focus on double-strand breaks. Not long ago, it was found that stem cells — functionally undifferentiated cells — play a major part in the formation of tumors by accumulating mutations and passing them on to the specialized cells that are their descendants. However, stem cell response to prolonged irradiation remains poorly understood.
The scientists conducted several experiments using stem cells derived from gingivae, or the gums. They treated the cells with identical radiation doses administered over long and short time spans. The formation of double-strand breaks was monitored using stained γH2AX and 53BP1 proteins as markers. With brief but intense radiation exposure, the incidence of both markers was found to increase linearly with the dose. But in the case of prolonged irradiation, the response was linear only up to a certain point, followed by a plateau at 1,000 milligrays. In other words, after reaching a certain number, the lesion count does not continue to rise. A balance of sorts is achieved between break formation and repair.
DNA repair
The cell comes equipped with repair systems capable of mending DNA double-strand breaks. However, following intense irradiation, the cell has to resort to a mechanism known as end joining — a quick but faulty procedure — in eight out of 10 double-strand breaks. This often leads to chromosomal aberrations. Such misrepairs of DNA breaks can potentially result in cell death, oncogene activation, and anti-oncogene suppression. But there is an alternative mechanism of DNA repair, called homologous recombination. It uses a similar or identical DNA molecule as a template and produces much fewer errors, but it is only available during certain phases in the cell cycle. The researchers monitored homologous recombination using Rad51, another protein marker. During a two-hour long exposure, the amount of Rad51 remained roughly constant, followed by a linear growth afterward. The team hypothesized that prolonged irradiation might activate homologous recombination.
Cell division
Stem cells can be divided into two groups, called proliferating and quiescent, where the former undergo division and the latter have ceased reproducing, and there is a balance between the two types of cells. The researchers counted up the DNA double-strand breaks in proliferating and quiescent cells separately. This is made possible by a certain protein that is only found in cells undergoing division. It turned out, in both types of cells, the number of DNA breaks grew, eventually reaching a constant value.
It was also observed that exposure to radiation did not change the roughly 4-1 ratio between proliferating and quiescent cells. However, a more detailed investigation revealed that four hours of “slow” irradiation result in a considerably increased number of cells in the S and G2 phases of the cycle, that is DNA synthesis and final preparation for division, respectively. It is during these phases that a copy of the cell’s DNA is available for the sake of division, but also to be used as a template in homologous recombination. This fact is a likely explanation for the detection of increased amounts of the Rad51 marker. To put it another way, irradiation causes a delay in the cell cycle with the consequence that, at any given time, there are more cells in those phases which enable homologous recombination. This means it is possible to repair DNA double-strand breaks correctly.
“We have shown that prolonged irradiation of mesenchymal stem cells leads to cell cycle redistribution. This might influence the biological response to radiation,” says Sergey Leonov, the director of the Phystech School of Biological and Medical Physics. “Our findings could become the basis of further research into double breaks in stem cells and their effect on tumor formation.”