A new study found that a common bacterium responsible for chest infections and sepsis in sick people, and which fails to respond to the strongest antibiotics, is spreading through hospital contacts.
The bacterium, called Klebsiella pneumoniae, is spreading through European hospitals, and some strains cannot be controlled even by carbapenems, an antibiotic category that was so far reserved as the final line of treatment for resistant infections. Such strains are called extremely drug resistant (XDR) bacteria. The patients chiefly affected include the very young and the very old, and those with weakened immune systems.
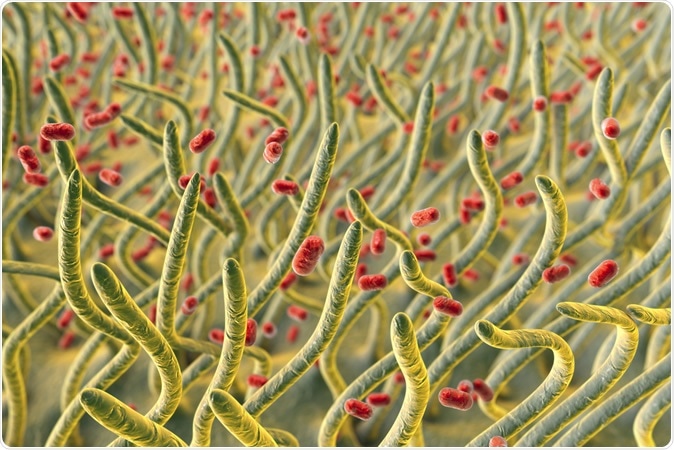
Klebsiella pneumoniae bacteria in respiratory tract, 3D illustration showing cilia of respiratory tract and bacteria. Image Credit: Kateryna Kon / Shutterstock
The study was carried out by the Center for Genomic Pathogen Surveillance, at the Wellcome Sanger Institute, University of Freiburg. They looked at 1700 samples of the bacterium isolated from patients in 32 countries, from almost 250 hospitals. Following genome sequencing, they concluded that the XDR strains led to about 350 deaths in 2007, but by 2015 they had gone up to over 2000, a rise of six times. This shows clearly that carbapenems are no longer reliable in the fight against antibiotic resistance, and this being so, doctors have few other lines of defense.
The survey covering the Enterobacteriaceae family, to which Klebsiella pneumoniae belongs, is remarkable for its size, exceeding all previous surveys in number, and marks the beginning of intensive and widespread surveillance of carbapenem resistance across Europe. The genome sequencing led to the discovery of certain genes that code for the carbapenemase enzymes that can break up these antibiotics. Recently, scientists have found that some bacteria carry one or more of these genes, and these have spread rapidly, probably due to the overuse of antibiotics in certain hospitals. The reason is that when bacteria are wiped out by other antibiotics, the remaining XDR bacteria take the lead in infections.
The current research found that almost 70% of XDR bacteria isolated from the patients belonged to just four strains with their derivatives. Moreover, the greater the resistance, the easier was their spread within hospitals. They concluded that more than half the XDR strains spread between patients in the same hospital, or between patients and other contacts.
First author Sophia David pointed out, “The 'One Health' approach to antibiotic resistance focuses on the spread of pathogens through humans, animals and the environment, including hospitals. But in the case of carbapenem-resistant Klebsiella pneumoniae, our findings imply hospitals are the key facilitator of transmission - over half of the samples carrying a carbapenemase gene were closely related to others collected from the same hospital, suggesting that the bacteria are spreading from person-to-person primarily within hospitals."
Not only so, antibiotic resistance was seen in related bacteria across hospitals in the same country but not across national borders, which suggests that they are being spread by healthcare facilities. The way out would be to put in place more stringent infection control measures, including the movement of patients from one hospital to another.
High levels of hospital hygiene were also stressed by the researchers. Co-author Hajo Grundmann says, “We are optimistic that with good hospital hygiene, which includes early identification and isolation of patients carrying these bacteria, we can not only delay the spread of these pathogens, but also successfully control them. This research emphasises the importance of infection control and ongoing genomic surveillance of antibiotic-resistant bacteria to ensure we detect new resistant strains early and act to combat the spread of antibiotic resistance.” they have also contributed a figure of 21 for the number of single nucleotide polymorphisms that should be detected for an optimal identification of a cluster originating in a single hospital, and to trace the international spread of these deadly bacteria.
The researchers are already mapping the second Enterobacteriaceae survey and are putting all their data on the public domain using MicroReact, an online tool developed by the Centre for Genomic Pathogen Surveillance. This will hopefully help to trace antibiotic resistance as it spreads in various harmful bacteria, and how new forms are emerging. One key aspect of the current work is its use of genomic sequencing, which enables them to track new strains of antibiotic resistance by their genomes rather than by older less accurate measures. Another researcher, David Aanensen, comments, “Currently, new strains are evolving almost as fast as we can sequence them. The goal to establish a robust network of genome sequencing hubs will allow healthcare systems to much more quickly track the spread of these bacteria and how they're evolving.”
Journal reference:
Epidemic of carbapenem-resistant Klebsiella pneumoniae in Europe is driven by nosocomial spread, Sophia David, Sandra Reuter, Simon R. Harris, Corinna Glasner, Theresa Feltwell, Silvia Argimon, Khalil Abudahab, Richard Goater, Tommaso Giani, Giulia Errico, Marianne Aspbury, Sara Sjunnebo, the EuSCAPE Working Group, the ESGEM Study Group, Edward J. Feil, Gian Maria Rossolini, David M. Aanensen & Hajo Grundmann, Nature Microbiology (2019), https://www.nature.com/articles/s41564-019-0492-8