An interview with Prof. Chris Griffiths, OBE MD FRCP FMedSci
What is psoriasis and how does it develop?
Psoriasis is a chronic immune mediated inflammatory disease, which affects the skin. It occurs in about 2 per cent of the UK population and affects at least 60 million people around the world.[1],[2]
The disease manifests as red, heavily scaled plaques, which are raised patches, anywhere on the skin. The most common involved sites are the scalp and the extensor aspects of the elbows, knees, and the lower back.
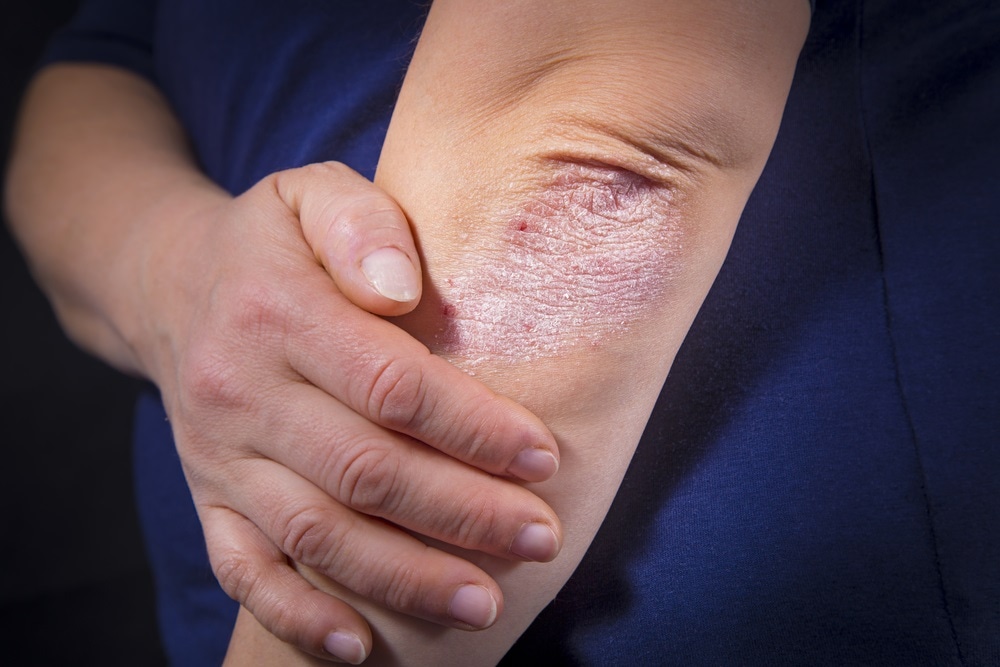
Image credits: Hriana | Shutterstock
However, the whole-body surface area can be involved. It produces significant physical, social and psychological detriment and is associated with a number of comorbidities such as psoriatic arthritis, cardiovascular disease, depression and diabetes, which form the metabolic syndrome.[3],[4]
Psoriasis can be genetically determined allowing it to run in families, particularly in those where it develops early in life.[5] Most people develop psoriasis before the age of 30 but it has been known for cases to develop after the age of 40, so it can develop anytime in life.[6],[7]
It is driven by the immune system in genetically predisposed individuals and there are certain triggers such as infections, for example a streptococcal pharyngitis, various medicines, or stress, but for many cases we don't know why it starts.[8] At present we have no cure for psoriasis.
What physical, psychological and social burden does psoriasis have on patients, and how are these linked?
The physical burden is that the plaques themselves can be, not just itchy but really quite painful, and they frequently crack and bleed. It can also affect the hands and feet, which can interfere with dexterity and cause discomfort in walking.
The comorbidities include psoriatic arthritis, which can have a significant detriment on physical mobility in up to 30 per cent of people who have that condition. The physical side is often underestimated by healthcare workers.[5] However, I think nowadays we are much more cognisant of how it affects the individual physically.[9]
Psychologically and socially, psoriasis has very significant consequences.[4],[10] One of the major stressors for people who have psoriasis is that they often practice avoidance coping. They will constrain their lives to avoid people knowing that they have psoriasis, for example they won't go to a local swimming pool because they're concerned that they may be asked to leave the pool. [10][11]
Members of the general public often believe that psoriasis, as with other skin conditions, might be contagious. There's a considerable stigma attached, which feeds the psychosocial side effects, such that people may withdraw from life and keep to themselves.[10],[12] They're not able to wear the clothes and have the lifestyle that they want.[13]
People with skin disease in general but particularly psoriasis are ostracized from society.[11] As a good example, for someone in a supermarket receiving change from the supermarket attendant, the attendant may not actually put the money into the patient's hand if they have psoriasis on their hands.
Overt bullying does also occur, I've heard many stories about children at school who get bullied because they've got psoriasis.[14]
What impact does or can psoriasis have on long-term patient health as well as the skin-related symptoms?
We now know that there's a significant long-term detriment on patient health, it's not just the skin, though the skin has a very major role. The effects on long-term patient health can be seen as what is termed the cumulative life damage..[10] This means that if people are not managed early, adequately and appropriately in the course of their disease, they can accumulate a chronicity of the condition.
Patients can accumulate comorbidities such as psoriatic arthritis and cardiovascular disease, hypertension and diabetes, which may come as a consequence of having the disease for a certain period of time.[15] But the exact link is not known or well worked out.
Patients can become depressed and anxious. There is debate around whether this is because of the stigmatization and the withdrawal, or whether there's an organic cause and psoriasis is not just inflammation in the skin, but inflammation in other organs, including the brain, which can lead to depression.[16]
What is your approach when assessing how best to treat each individual patient?
I think that's a very good point. The management of psoriasis is not just getting patients on the right medicine. We know that psoriasis is not a single disease, it's likely many or several different diseases that clinically look very similar which, with time, we’ll be able to differentiate according to genetics and immunology.
This will allow us to classify people into different forms of the disease and allow us to place people on the correct treatment, such as a biologic, according to the disease signature or profile.
The management also involves altering the patient’s lifestyle with the right advice to help themselves, for example: losing weight, stopping smoking, stopping drinking alcohol or reducing alcohol intake, more sleep, and more exercise. All of these on their own will help manage the disease to an optimal level.
This is a holistic, whole patient view. At the same time, one has to screen for cardiovascular risk factors, such as a high cholesterol and high blood pressure.
Please give a bit of background into your work with psoriasis and types of psoriasis treatment.
I am an expert on psoriasis, having been in the psoriasis field for 36 years.
I have been involved with that whole journey from demonstration that the immune system is involved, to what we now call the biologic era. I did my initial training with Prof. Lionel Fry in St Mary's Hospital, London. That's where we did that original work on psoriasis immunology and further in Michigan with Professor John Voorhees, another acknowledged psoriasis expert.
For the past 26 years I've been in Manchester, UK, where we set up one of the first multidisciplinary psoriasis clinics for complex patients, and at the same time, initiated research around what we call the brain skin axis. This work identified the links between brain function and psoriasis.
I also helped to establish the national UK and Ireland biologics registry – British Association of Dermatologists Biologics and Immunomodulators Register (BADBIR) for psoriasis, back in 2007. This is now the leading such registry worldwide with over 18,000 patients followed up long-term on biologics and conventional systemic therapies.[17]
I also started the dermatology clinical trials unit in Manchester where we've trialled and navigated the NHS approval process for most of the biologics that we use for psoriasis in this country. I chair the Medical Research Council stratified medicine consortium on psoriasis – Psoriasis Stratification to Optimize Relevant Therapy (PSORT), which looks to ascertain what biomarkers can be used in an algorithm to predict which patient will respond to which biologic.[18]
A new initiative in Manchester is the psoriasis rapid access clinic where we are now seeing patients with psoriasis within a few months of them first developing the disease. This allows us to enact or operationalize a holistic view of treatment, getting patients onto the right treatment and lifestyle very early on.
From Manchester we run the Global Psoriasis Atlas on behalf of the International League of Dermatological Societies, the International Psoriasis Council and the International Federation of Psoriasis Associations. The website for this project was launched on World Psoriasis Day, 29th October 2019. This is the first attempt, at the behest of the World Health Organization, to collate all the epidemiological information we have on psoriasis from around the world, in order to ascertain the true burden of the disease.
How do you engage with primary care teams to support their role in diagnosis, timely referral and on-going management?
The main area to really make a difference, is in primary care. It must be difficult to be a GP, with so many calls on one's time. Often skin disease gets demoted down the hierarchy of importance because it never seems to have the urgency unless it's skin cancer. However, psoriasis is a condition that does have significant systemic manifestations and should be given a higher priority.
We need to train and educate GPs more about the recognition and diagnosis of psoriasis. This should include what can be done early on, and not just giving patients a cream but actually giving patients advice about the disease, what it is and what it isn't, and how they can start to get onto the right lifestyle, the right treatments, and also refer them early.
The key is not to be inert for years with nothing much happening, as cumulative life damage is occurring. A lot of what we try to do with our rapid access clinic in Manchester is to take some of the pressure off GPs and ask them to refer patients straight to us. We'll take over the initial management. Hopefully we'll be able to manage them at a distance using an app, which will allow them to have the direct connection back to us in the rapid access clinic.
I think this has to be the way to manage patients and it has been used quite successfully in the management of early rheumatoid arthritis. We're trialling this in Manchester to see if it will save money in the long-term by reducing comorbidities and cumulative life damage, which should therefore save on the social care budget as opposed to the health care budget.
How do you work with your patients in a patient-centred way which manages each individual’s expectations from their treatment?
The future is going to be much more proactive in the way we manage patients, than the current reactive process. I think that the more we use big data and data streaming from an individual, the more we'll be able to monitor their health in a proactive manner. The approach needs to be a collaborative one, working with patients to develop programmes they are comfortable with and that suits their needs. We are very strong advocates of patient involvement.
Can you tell us about the Psoriasis Shout Out® programme?
Since 2014 we've run the Psoriasis Shout Out® programme, an initiative that aims to get people talking about psoriasis and to bring psoriasis patients together with professionals working in the field. Our overarching message is a positive one - it is possible to live well with psoriasis.
We run a week-long roadshow of events each year to raise awareness about psoriasis to the general public. The campaign also works to inform patients about what's possible nowadays and that they should seek help early on, whilst providing information around the things they can do to help themselves. We run all sorts of initiatives around this programme, for example we’ve done flash dances and even poetry projects.
In Manchester, we have a trailer and exhibition stand that goes around to various places across the city over the course of the week and members of the team will engage with passers-by about the disease. It's amazing how many people with psoriasis come forward under those circumstances and turns out they've not previously had very much in the way of advice or treatment.
How important is it to measure overall quality of life for patients while assessing the impact of their treatment plan?
I think measuring quality of life is very important and it’s not easy to do in psoriasis.
We can measure psoriasis using the psoriasis area severity index (PASI) and for quality of life we use the dermatology life quality index (DLQI).[19],[20] This is a 10-point scale that patients complete themselves. We ask questions about how psoriasis has affected certain aspects of their lives over the previous week and that provides a snapshot of whether they have very good quality of life, which would be zero out of 30, or very poor, which would be anything really greater than 10 to 15 or above.
You may have people whose psoriasis is physically mild, but they still may have an impaired quality of life. That might be because the psoriasis is very itchy or it's on sites such as the face or palms or genitals even, which are interfering with how they'd like to run their lives, and they feel stigmatized or embarrassed about that. If the patient doesn’t have a DLQI quality of life score of zero or 1 then there is still something to be investigated.
It’s important we include these measures within our clinical trials. We need these data as it's not just about the improvement of the PASI, it is also about the improvements of DLQI.
Do you have an example of a challenging case, where the patient’s life has been transformed through your holistic and patient-centred approach to delivering care?
One of the great things about running the psoriasis clinic is that one can experience how biologics can invoke transformational change in people's lives. Just a month ago, there was a 58-year-old lady, who had been on one the biologics for about three to four months.
I saw her back in the clinic and she said, "Professor Griffiths, I really want to thank you, my psoriasis is now clear, and I am now doing something that I’ve wanted to do since I was 14." I asked her what that was and she said, "Well, my psoriasis began when I was 14, and this is the time when my friends were starting to go to the swimming pool, but I never learned to swim because I wouldn't go with them as I was too self-conscious. But now that my skin is clear of psoriasis I'm learning to swim, so I can do something I've actually put off for 44 years."
What do you see as the future of psoriasis treatment?
I think we have made phenomenal progress over the past several years with the biologic therapies and some of the newer small molecule therapies, which are truly founded on understanding the basic mechanisms of the disease.
However, that's not the answer for everybody. There's still a lot of unmet need and it comes down to understanding what the patients need, which is seeing them early, being able to ascertain barriers to access to care for people with psoriasis, not just in the Western world, but also in the least developed countries.
As far as the Global Psoriasis Atlas is concerned, we went to Tanzania in July to do some field work, which was quite an eye opener. Although psoriasis is not as prevalent as it is in the UK, people are frequently misdiagnosed by non-dermatologist, healthcare workers as having fungal disease.
Even if they do get a correct diagnosis, the treatments available to them are very limited. I believe passionately that just because they may live in a place, such as Tanzania, doesn't mean that they shouldn't have the best care available. This for me is the key issue, it's looking at psoriasis as a global problem and not just one that's linked to the wealthier countries of the world.
About Prof. Chris Griffiths
Chris Griffiths OBE MD FRCP FMedSci
University of Manchester, Manchester, UK
Chris Griffiths qualified from St Thomas’ Hospital Medical School, London and trained in Dermatology at St Mary’s Hospital, London, and at the University of Michigan, USA. He was appointed to the Foundation Chair in Dermatology at the University of Manchester in 1994 and is an honorary consultant dermatologist at Salford Royal NHS Foundation Trust. In 2015 he received the Sir Archibald Gray Medal, for outstanding service to British Dermatology and in 2019 the British Society for Investigative Dermatology Medal for contributions to research. In the 2018 Queen’s New Year Honours he was appointed OBE, “for services to dermatology”.
Chris is the current President of the European Society for Dermatological Research and a past-President of the British Association of Dermatologists (BAD) and International Psoriasis Council. Chris is Director of the MRC stratified medicine consortium on psoriasis (PSORT); Director of the Global Psoriasis Atlas; and Chief Investigator of the BAD Biologics and Immunomodulators Register (BADBIR). He has a career-long research interest in all aspects of psoriasis and is active in global health initiatives being special advisor to the International League of Dermatological Societies on global health research and policy.
This article has been sponsored by, and developed in conjunction with, Janssen-Cilag Ltd.
EM-24085
Date of preparation: January 2020
Journal references:
[1] Griffiths CE, et al. (2017) The global state of psoriasis disease epidemiology: a workshop report. Br J Dermatol; 177(1):e4-e7.
[3] Griffiths CE, Barker JN. (2007) Pathogenesis and clinical features of psoriasis. Lancet;370(9583):263-271.
[4] Ferreira BI, et al. (2016) Psoriasis and Associated Psychiatric Disorders: A Systemic Review on Etiopathogenesis and Clinical Correlation. J Clin Aessthet Dermatol;9(6): 36-43.
[5] Roberson ED, Bowcock AM. (2010) Psoriasis genetics: breaking the barrier. Trends Genet; 26(9):415-423.
[6] Nograles CE, et al. (2009) New insights into the pathogenesis and genetics of psoriatic arthritis. Nat Clin Pract Rheumatol;5(2):83–91.
[7] Queiro R et al. (2014) Age at disease onset: a key factor for understanding psoriatic disease. Rheumatology;53(7):1178-1185.
[8] Fry L, Baker B. (2007) Triggering psoriasis: the role of infections and medications. Clinics in Dermatology;25:606–615.
[9] National Institute for Health and Care Excellence. Impact of psoriasis more than skin deep. Available at: https://www.nice.org.uk/. Accessed January 2020.
[10] Ros S, et al. (2014) Cumulative Life Course Impairment: The Imprint of Psoriasis on the Patient’s Life. Actas Dermosifiliogr;105(2):128-134.
[11] Ginsberg I, Link B. (1993) Psychosocial consequences of rejection and stigma feelings in psoriasis patients. Int J Dermatol; 32(8):587-91.
[12] Hrehorów E et al. (2012) Patients with Psoriasis Feel Stigmatized. Acta Derm Venereol 2012; 92: 67–72.
[13] Khoury LR, (2014) Body image altered by psoriasis. A study based on individual interviews and a model for body image. J Dermatolog Treat.;25(1):2-7.
[14] Magin P. (2013) Appearance-related bullying and skin disorders. Clinics in Dermatology;31:66–71.
[15] Oliveira M de F, et al. (2015) Psoriasis: classical and emerging comorbidities. An Bras Dermatol;90(1):9–20.
[19] Zheng J. (2017) Absolute Psoriasis Area and Severity Index: an additional evaluation for clinical practice. Br J Dermatol;176(3):576.