Pulmonary, or lung, fibrosis, is a term that denotes a life-shortening medical condition in which healthy tissue within the lung becomes thick and forms scar tissue. The resulting inflammation leaves the lungs lined with fibrous scar tissue, which cannot exchange gases efficiently. Treatment is purely symptomatic, other than allogeneic lung transplantation, which is highly invasive and has a 50% five-year mortality rate, as well as requiring lifelong immunosuppression.
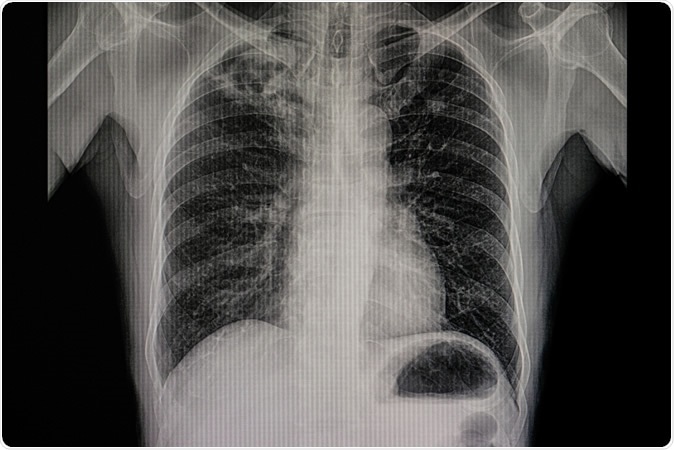
Xray film of a patient with active pulmonary tuberculosis with numerous cavitations and fibrotic change in the right upper lung. Image Credit: Tomatheart / Shutterstock
Stem cells and lung healing
The lungs contain resident stem cells, which can give rise to stem cells that can be used to promote the healing of lung injuries, but it was difficult to isolate and culture them. As a result, mesenchymal stem cells (MSCs) continued to be used to treat lung diseases. These have a low rate of engraftment in the lungs, and few differentiate into mature lung cells, probably because they are not native to the lung tissue itself.
A breakthrough came when some of the researchers behind the current study first demonstrated that therapeutic lung cells called lung spheroid cells (LSCs) could be produced by a three-dimensional culture technique, from lung biopsies obtained by the transbronchial route. This route, being minimally invasive, carries very low mortality compared to surgical lung biopsy. The LSCs are resident in the lung and can therefore engraft and survive here.
They were able to generate more than 50 million LSCs from one lung biopsy. They contained both lung stem cells and supporting cells, such as epithelial and mesenchymal cells. This mixture is essential to maximize the efficiency of stem cell function through the fibroblast growth factors and other signaling molecules released from these other cells. Once introduced into the body, they remain in the lungs for up to 21 days.
Over the last 5 years, the researchers have produced and tested LSCs in order to evaluate their effectiveness in this condition. Researcher Ke Cheng explains: "The mixture of cells in LSCs recreates the stem cells' natural microenvironment - known as the stem cell niche - where cells secrete exosomes to communicate with each other just as they would inside your body. LSCs secrete many beneficial proteins and growth factors known collectively as 'secretome' - exosomes and soluble proteins, which can reproduce the regenerative microenvironment of the cells themselves. In this work, we took it one step further and tested the secretome and exosomes from our spheroid-produced stem cells against two models of pulmonary fibrosis."
The study
The researchers carried out a comparison between secretome and exosomes from (MSC-Sec and MSC-Exo, respectively), a commonly used type of stem cell, and lung spheroid cell (LSC-Sec and LSC-Exo, respectively), in mouse and rat models of pulmonary fibrosis. The lesions in the lung were induced by chemical exposure or silica particles.
The scientists used a "stem cell sauna," which is a nebulizer that is used to inhale therapeutic proteins, small molecules, and exosomes straight into the lungs.
The findings
In mice with chemical-induced lung fibrosis, nebulization therapy with either LSC-Sec or MSC-Sec produced marked alleviation of fibrosis as compared to saline nebulization, but LSC-Sec reduced the fibrosis to nearly half, while MSC-Sec brought it down by a third.
However, when the mouse had silica-induced fibrosis, the treatment with LSC-Sec and MSC-Sec reduced fibrosis by just over a quarter and about 17%, respectively.
They then repeated the experiment with rats and found the same pattern. However, they also found that inhalation with LSC-Exo alone also produces the same type of improvement, but of lower magnitude compared to inhalation of the full secretome.
Implications
Cheng says, "This work shows that lung spheroid cell secretome and exosomes are more effective than their mesenchymal stem cell counterparts in decreasing fibrotic tissue and inflammation in damaged lung tissue. Hopefully, we are taking our first steps toward an efficient, non-invasive, and cost-effective way to repair damaged lungs."
Furthermore, it is not just about lung fibrosis. The researchers plan to test the efficacy of the therapy against even more lung diseases, including chronic obstructive pulmonary disease (COPD), pulmonary hypertension, and acute respiratory distress syndrome.
Moreover, the interest of the study does not end there. The findings also show that it is not just the stem cells, but the products they release, that can act just as well as the stem cells do to treat pulmonary fibrosis. Another researcher, Kenneth Adler, comments, "[This] can be a major finding that can have implications in many other diseases where stem cell therapy is being developed."
Journal reference:
Dinh, P.C., Paudel, D., Brochu, H. et al. Inhalation of lung spheroid cell secretome and exosomes promotes lung repair in pulmonary fibrosis. Nat Commun 11, 1064 (2020). https://doi.org/10.1038/s41467-020-14344-7