Non-pharmaceutical interventions (NPIs) and virus testing are melded in the effort to flatten the curve, thus reducing the number of new cases occurring daily and offering healthcare systems and public authorities the time to prepare for the coming wave of infections. However, given the resulting instability of the social and economic situation, both federal and state governments are chafing to return to normalcy as soon as possible.
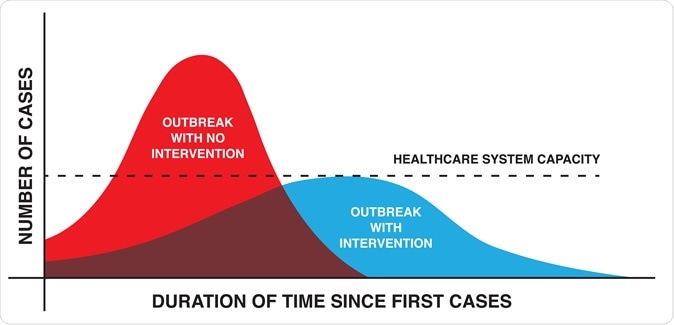
Flatten the COVID-19 curve illustration slowing the spread of the virus. Image Credit: DigitalMammoth / Shutterstock

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
The current study aims to examine how feasible the strategy of gradual easing of lockdown orders can be in the absence of a vaccine.
How was the study done?
The researchers looked at a large urban area in Washington State’s King County. They modeled various scenarios of removing lockdown and social distancing requirements over one year dating from the first infection. They hope to develop a potential guideline for the authorities to optimize the changes that should be implemented to evolve a sound lockdown relaxation policy.
The researchers used the open-source FRED model to create an agent-based simulation. FRED stands for Framework for Reconstructing Epidemic Dynamics. The model included the county population, patterns of daily contacts, SEIR-model based transmission estimates for COVID-19 in the county, and current NPIs in place.
After running a 365-day simulation, the daily incidence of new cases was estimated to evaluate how relaxing social distancing would change the situation.
The fundamental assumptions
The baseline assumptions made by the researchers included:
- The first infection date in King County is January 15, 2020, in a man from Snohomish County who commuted to Seattle, WA, thereby possibly having some influence on King County.
- This case represents the only non-local transmission, with all other patients being attributed to community transmissions in the county.
- All patients were classified as non-severe and severe groups. They assumed similar patterns of illness in those with or without symptoms, terming this the non-severe cases.
- Symptoms are more severe in those who are older, but severe illness does not mean more infectious.
- Recovered patients were considered entirely immune to the illness.
The researchers modeled three NPIs used commonly in the USA – case isolation at home, school closure, and social distancing. They did not include contact tracing or voluntary home quarantine because these were not being done or were incorporated into the other measures.
Ending the lockdown
The researchers also simulated mix’n’match strategies using eight different levels of social distancing that were possibilities after the lifting of the current total lockdown on May 4, 2020. They also simulated a scenario in which no interventions were implemented. They simulated interventions before this date as set out in the Washington State emergency order.
School opening in fall was assumed given the practical difficulties involved in extending the closure beyond the close of the current academic year.
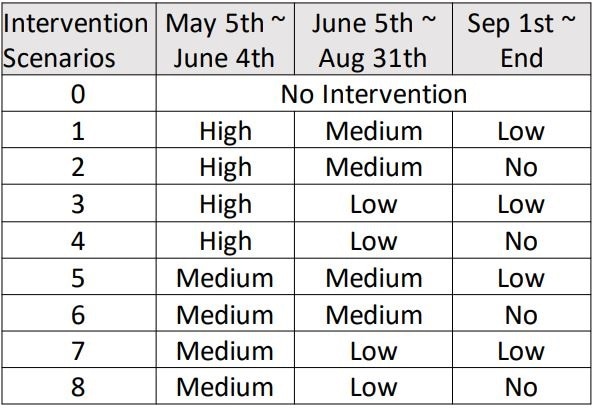
Scenarios
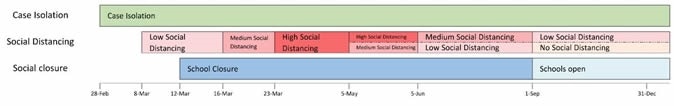
Diagram of Simulated Scenarios
The outcomes
The researchers found that in comparison to scenario 1-8, scenario 0 is associated with a far worse outcome. In other words, any intervention is better than no intervention, and the NPIs set in place in March did reduce cases and postpone the new cases.
The scenarios rank in ordinal number from 1 through 9, and finally 0, in terms of effective reduction in the viral spread.
The most robust and lasting intervention was in scenario 1, and the total infections go down from over 40% to 15% of the numbers in scenario 0.
The peak of the new daily cases was on March 18, 2020, in scenario 0, at 37,300 people. With other scenarios, the peak arrived earlier on March 11, 2020, affecting almost 18,800 people.
The second wave
Whichever the scenario, a second wave hit. With scenario 1, where the daily new infection rate dropped to 2 by June 4, in the simulation, and remained at about 20 until August, the incidence surged with the lifting of lockdown and opening of school. At this point the cases jumped back again to 874 cases a day in the absence of any importation.
In scenario 2, social restrictions were removed entirely from September 1 onwards. In scenario 5, on the other hand, low-level social distancing norms were kept in place from September to the time the simulation ended. Both ended with the same total number of infections.
In other words, the choice is between extending social distancing at high levels for one more month (until June 4) or keeping low-level social distancing in place through September.
One more comparison between scenario 1 and scenario 2 shows that when analyzed by place, the total lifting of social distancing requirements will cause a doubling of the peak workplace infections and a tripling or more of neighborhood infections after May 4, compared to keeping a low-level lockdown in place.
Limitations
The model has its limitations. For instance, in the early phase of the spread of the virus, the daily number of new cases is much higher than the number reported. This overestimation of true incidence may be acceptable since only 12% of symptomatic cases are reported in the US, especially till March 2020, and because so many COVID-19 infections go unnoticed or undiagnosed. Secondly, the researchers used only self-isolation and not the hospitalization or death rates during the disease spread. This was based on the assumption that disease transmission will be reduced to the same extent by hospitalization, death, or 100% self-isolation at home for severe patients.
Future challenges
The researchers summarize: “While reopening society is important in revitalizing the economy, policymakers should be very cautious in reopening even if daily confirmed cases decrease to one digit or even zero due to low reporting rate.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources