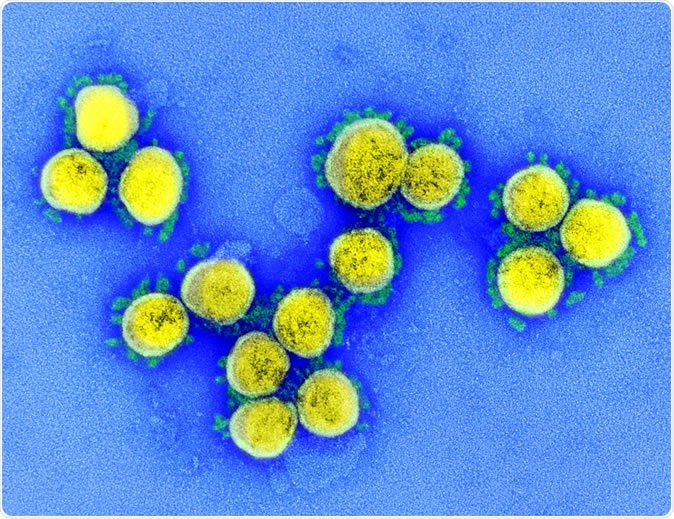
Even as the COVID-19 pandemic continues to smolder and flare up in various parts of the world, researchers are still trying to make sense of the virus, its routes of spread, its target tissues, and the immune responses it induces. One crucial piece of knowledge is that the primary viral receptor is a human enzyme called angiotensin-converting enzyme 2 (ACE2).
What is the RAS?

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
The RAS is an essential hormonal system that regulates the blood pressure, the salt and electrolyte balance, and blood volume. It also controls the regional blood flow and the growth rate of tissues in response to several stimuli. It is a network of cascading regulatory components as well as peptide hormones that modulate the function of blood vessels.
Angiotensin I (Ang I) is one of the major peptides in this system and is metabolized by the angiotensin-converting enzyme (ACE) to form angiotensin II (Ang II), which in turn is broken down by ACE2 to form Angiotensin 1-7 (Ang 1-7). While Ang II is a potent vasoconstrictor, pushing up the blood pressure, Ang 1-7 is a vasodilator.
What Is the Function of ACE2 In the Body?
ACE2 is a glycoprotein, an exopeptidase or peptide-cleaving enzyme attached to the outer surface of most cells in the human body. Its highest expression is in the kidney, the endothelium, the lungs, and the heart.
While it is similar in some ways to ACE, it is not blocked by the same drugs. By breaking down Ang II, it relieves vasoconstriction and hypertension. It also blocks the atherosclerosis-promoting effects of Ang II, such as inflammation and oxidative stress, endothelial dysfunction, migration, growth, and proliferation of vascular smooth muscle cells, and clotting within the blood vessels.
By producing Ang 1-7, ACE2 increases anti-inflammatory and antioxidant effects, improving vascular function. At the same time, higher levels of Ang II upregulate the expression of ACE2.
ACE2 in COVID-19
The SARS-CoV-2 that causes COVID-19 is able to enter host cells via the ACE2 receptor. This fact has led to the hypothesis that inhibition of the RAS could lead to higher levels of ACE2 expression, which in turn promotes viral attachment and entry to the host cells. This could increase the risk of severe illness and death.
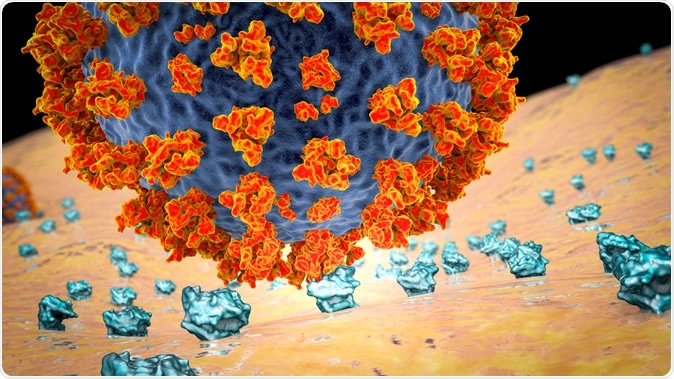
SARS-CoV-2 virus binding to ACE2 receptors on a human cell, the initial stage of COVID-19 infection. Image Credit: Kateryna Kon / Shutterstock
Few studies have considered the effect of inhibiting the RAS activity on the expression of ACE2 in human tissues that play an important role in regulating the blood pressure and determining the susceptibility to COVID-19 infection.
How Do Hypertension and RAS Inhibitors Affect ACE2 In Kidney Tissue?
The investigators in the current study looked at the ACE2 expression in kidney tissue from 436 patients with hypertension, other related conditions, and who were on RAS blockers. They used RNA sequencing to characterize the transcription products of the kidney cells.
They found that the levels of ACE2 increase with age in human lung and kidney tissue. This could explain the increased susceptibility of older people to symptomatic COVID-19 infection.
However, there was no link between the extent of expression of this viral receptor in the kidney and hypertension, nor with the use of commonly prescribed RAS blockers. Instead, the researchers found that the renal function, as described in terms of biochemical tests, is positively correlated with the expression of ACE2 in the kidney tissue. The study also shows that ACE2 is co-expressed with genes that play a major role in both the health and disease states of kidney tissue.
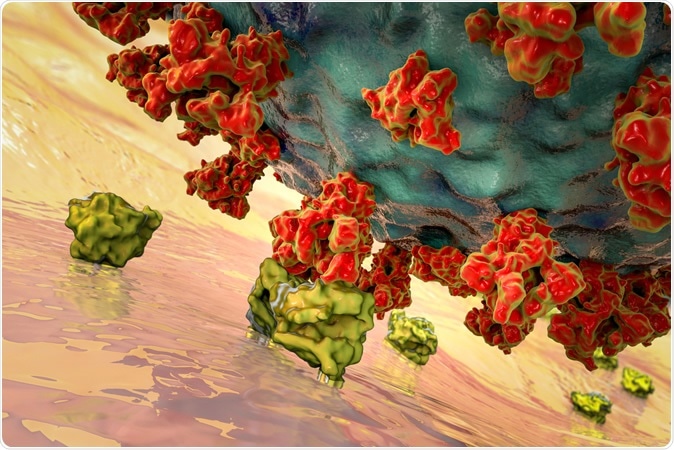
SARS-CoV-2 viruses binding to ACE-2 receptors on a human cell, the initial stage of COVID-19 infection, conceptual 3D illustration credit: Kateryna Kon / Shutterstock
What Does the Study Show?
The researchers summarize: “Collectively, our data indicate that neither hypertension nor antihypertensive treatment is likely to alter individual risk of SARS-CoV-2 infection or influence clinical outcomes in COVID-19 through changes of ACE2 expression.”
Even though the presence of ACE2 in abundance in kidney tissue is not linked to either a higher chance of COVID-19 or to a more severe outcome in case of infection, it is likely, according to the study, that the increasing levels of ACE2 with age plays a part in the higher risk of COVID-19 infection. However, under ordinary circumstances, the expression of ACE2 in the kidneys is protective to these organs against the deleterious effects of hypertension and vasoconstriction.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Jiang, X. et al. (2020). Hypertension and Renin-Angiotensin System Blockers Are Not Associated with Expression of Angiotensin Converting Enzyme 2 (ACE2) In the Kidney. medRxiv preprint. doi: https://doi.org/10.1101/2020.05.19.20106781. https://www.medrxiv.org/content/10.1101/2020.05.19.20106781v1
- Peer reviewed and published scientific report.
Jiang, Xiao, James M Eales, David Scannali, Alicja Nazgiewicz, Priscilla Prestes, Michelle Maier, Matthew Denniff, et al. 2020. “Hypertension and Renin-Angiotensin System Blockers Are Not Associated with Expression of Angiotensin-Converting Enzyme 2 (ACE2) in the Kidney.” European Heart Journal, October. https://doi.org/10.1093/eurheartj/ehaa794. https://academic.oup.com/eurheartj/article/41/48/4580/5940440.