A team of 121 researchers from the United States and Canada reports that while digestive manifestations seem to be common among people hospitalized with coronavirus disease 2019 (COVID-19), the majority appear to be mild and not associated with severe clinical outcomes.
Experts from the North American Alliance for the Study of Digestive Manifestations of COVID-19 and collaborators say that of almost 2,000 patients, more than half experienced a gastrointestinal symptom such as diarrhea or nausea at some point during their illness. More than half of patients also had an abnormal liver test result.
However, around three-quarters of the gastrointestinal symptoms were categorized as mild. After adjustment for confounding factors, neither gastrointestinal symptoms nor abnormal liver test results were associated with an increased risk for mechanical ventilation or death.
A pre-print version of the paper is available on medRxiv*, while the article undergoes peer review.
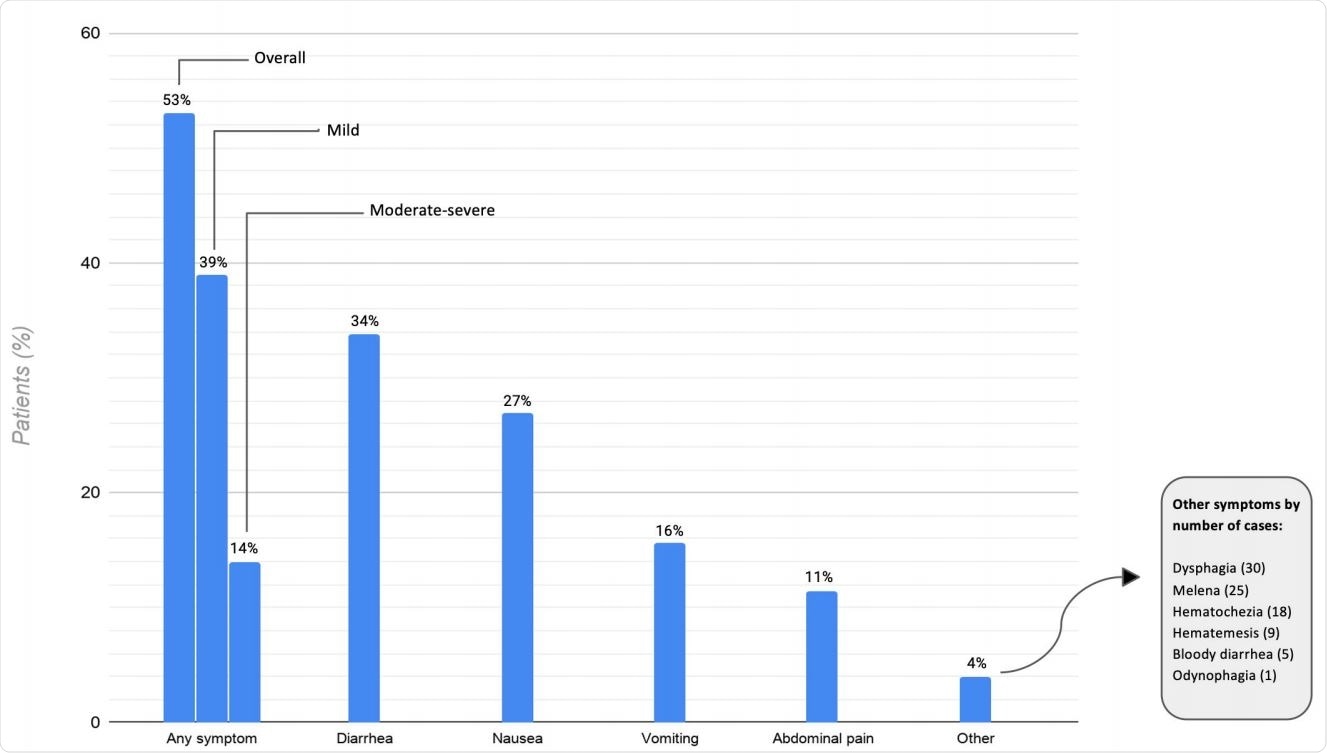
Gastrointestinal symptoms in patients hospitalized with COVID-19.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Digestive system involvement in COVID-19
Although COVID-19 is predominantly a respiratory illness, studies have also pointed to digestive system involvement and gastrointestinal symptoms.
To infect cells, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) first binds to the angiotensin-converting enzyme 2 (ACE2) receptor, which is expressed at higher levels in the gut than in the respiratory system.
Joseph Elmunzer (University of South Carolina) and colleagues say it has been proposed that intestinal infection might influence the severity of respiratory and systemic pathogenesis by altering the microbiome, intestinal immunity, and gut permeability.
Reports have so far been conflicting
Digestive manifestations may frequently occur in patients, but reports have been conflicting, and the true prevalence remains unknown.
A series of studies conducted in China suggested that gastrointestinal symptoms occur in less than 10% of cases, while other studies have pointed to higher prevalence, ranging from 30 to 60%. Similarly, the reported prevalence of abnormal liver test results has ranged from 15 to 50%.
Furthermore, the effect that digestive manifestations may have on overall outcomes in COVID-19 is not known. Some studies have reported associations between gastrointestinal symptoms, liver abnormalities, and disease severity, but again reports have been conflicting.
Studies assessing digestive manifestations have been limited in scope, only reporting on an isolated geographical region or a single hospital, for example. According to the authors, the studies have also used different and potentially biased sampling methods.
What did the current study involve?
Now, Elmunzer and the team have assessed the prevalence and severity of digestive manifestations among 1,992 hospitalized COVID-19 patients (aged an average of 60 years) using data collected from 36 medical centers across North America between 15th April and 5th June 2020.
Digestive manifestations were divided into gastrointestinal symptoms, and liver test abnormalities and multivariate regression analysis were performed to investigate whether such manifestations were associated with severe patient outcomes (mechanical ventilation or death).
Digestive manifestations were common but mild
The team reports that 53% of patients had experienced at least one gastrointestinal symptom at some point during their illness. Of those individuals, symptoms were considered to be mild in 74% of cases. The most common symptom was diarrhea (34%), followed by nausea (27%), vomiting (16%), and abdominal pain (11%).
Fifty-five percent of patients had an elevated liver test result at some point during their illness. Of those individuals, 35% had an elevated alanine aminotransferase (ALT) or total bilirubin (TB) level, suggesting SARS-CoV-2 infection may have resulted in hepatic injury, write the researchers.
However, the ALT and TB levels were elevated to less than five times the upper limit of normal in the large majority (77%) of cases, suggesting that clinically important hepatic injury is uncommon in cases of COVID-19, say Elmunzer and team.
No association with severe outcomes
By the end of the study period, 32% of patients had required mechanical ventilation, 19% had died, and 1.5% were still hospitalized. The median length of hospital stay was nine days.
After controlling for potential confounders, the presence of gastrointestinal symptoms, or an abnormal liver test result on admission were not associated with the use of mechanical ventilation or death.
“Among patients hospitalized with COVID-19, gastrointestinal symptoms and liver test abnormalities were common, but the majority were mild, and their presence was not associated with a more severe clinical course,” write the researchers.
Nevertheless, the findings provide valuable information on the overall burden of digestive manifestations in hospitalized COVID-19 patients, they add.
“Future mechanistic investigation will be necessary to better understand whether infection leads to direct hepatic injury,” concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources