Since the declaration of the COVID-19 pandemic, many countries have implemented restrictions on mobility and social interactions, including lockdowns. This has been associated with a reduction in the number of extremely preterm (EP) babies, according to one Danish study. A recent paper published on the preprint server medRxiv* in October 2020 reveals that this may not be the case.
In the Danish paper, the scientists reported a single EP birth during the month from March 12, 2020, compared to an average of ~11 EP births in the same period over the five years immediately preceding it in Denmark. This was supported by a single-center Irish study, which also showed that no babies with extremely low birth weight that is, below 1,000 grams, were born between January to April in 2020, as against ~5 in the same period during the previous two decades!.
This was also reported by other neonatal intensive care units (NICU) worldwide, and within the SafeBoosC-III consortium, though other neonatologists have stated the opposite. The difficulties posed by the pandemic in conducting clinical trials has not helped to conclude.
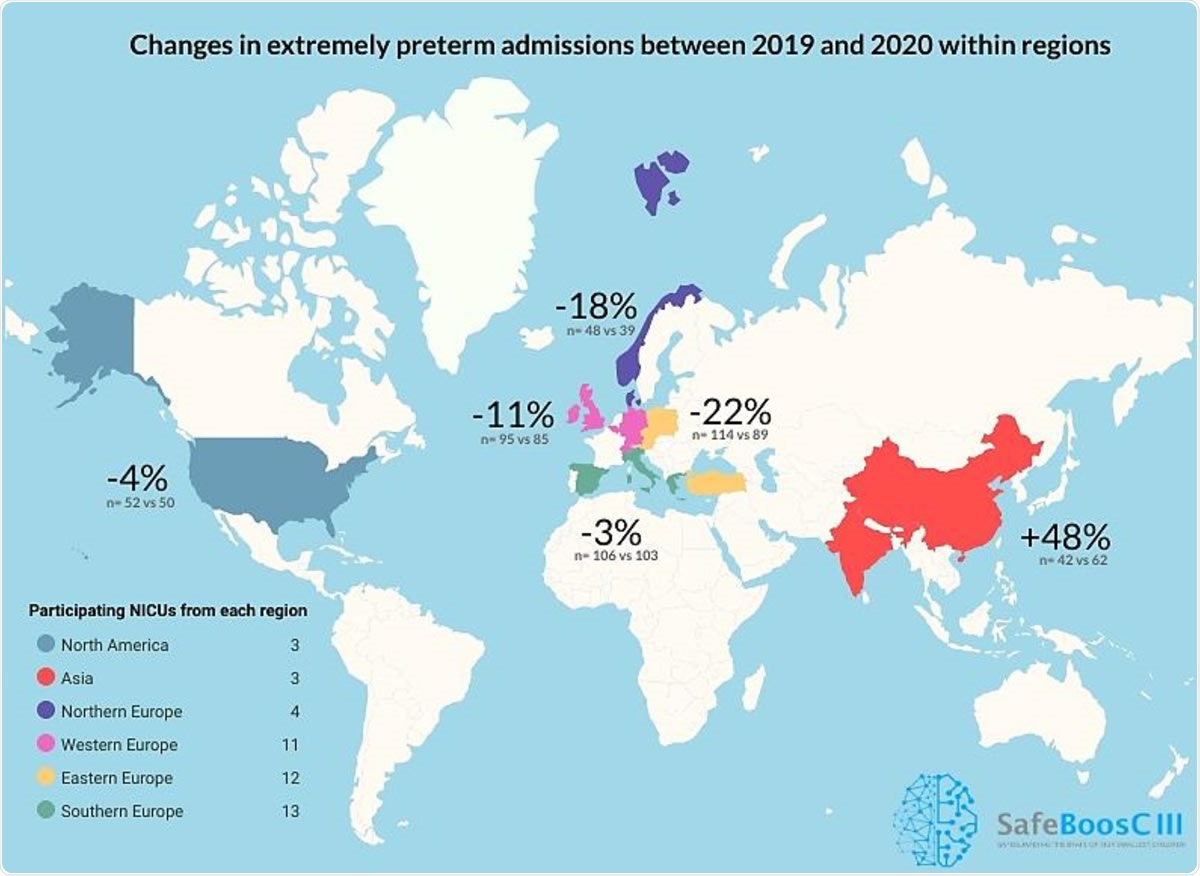
Change in percent in extremely preterm admissions between the three months with the most rigorous lockdown restrictions in 2020, compared to the corresponding months of 2019 in the 46 participating NICUs in the SafeBoosC-III consortium.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Lockdown Had No Significant Impact on EP Births
The current study uses data from the SafeBoosC-III trial regarding both the benefits and the harms of treatment of EP babies guided by near-infrared spectroscopy rather than routine monitoring. They looked at the number of EP admissions in NICUs during the global lockdown as their measure of the change in EP births. They also explored any possible geographical variation, especially any related to local lockdowns.
In this study, they found that 885 infants were admitted to 46 NICUs in 17 countries. About half of them, ~430, were admitted in the first three months, and the rest, ~460, in the corresponding period in the previous year. There was no significant difference in the admissions in these two years, even when examined by region.
The investigators were also asked to give their opinion as to whether the lockdown had caused a marked impact on the daily life of a pregnant woman. Almost 75%, or 33 out of 46, answered in the affirmative – the pandemic had brought a radical or very radical change.
Secondly, they were asked if, in their opinion, the restrictions on attending health institutions meant that very EP infants might not be admitted to NICUs. Again, almost 75% said this was probably or almost certainly not the case. Seven of 46 said changes had been made in their NICU, including carrying out COVID-19 testing on all patients before admission. One postulated that the substitution of online consultations for in-person visits might have allowed some intrauterine complications to go unnoticed, leading to more preterm births.
However, the facts show that there was no significant difference in the number of EP admissions during these three months when the lockdown was most rigorous, compared to the same three-month period in the preceding year. This pattern held good over the whole region. Neither was there any relationship between the level of restriction during the lockdown and the number of EP admissions in the NICU.
Limitations and Future Directions
While these results do not support those of earlier studies, the outcome indicates that the lockdown produced a minimal impact on the rate of EP births. Some plausible contributors to a good pregnancy outcome may include women being at home more, spending less time on their feet, having less stress, and avoiding many infections. On the other hand, less contact with their doctors may have reduced the odds of iatrogenic preterm birth as well.
The researchers say, “To our knowledge, this study is the largest so far, evaluating the effect of the first phase of the COVID-19 pandemic on EP infant admissions.” The size of the sample ruled out errors due to insufficient numbers, and the danger of selective reporting bias is ruled out since the trial protocol was registered beforehand.
The data was from the period of strict lockdown, which was not always the period of the peak case number. Secondly, response bias may have occurred since investigators were asked to give their subjective opinions on the impact of the lockdown on the lives of pregnant women and the admission of EP babies to their NICUs. Thirdly, the transfer of such babies from one NICU to another may result in a falsely high count of EP births if investigators are staffing both NICUs within the same country.
The study was limited to three weeks because of the perceived urgency of the situation. Future studies may be conducted over a more extended period to ensure better participation. In this study, 33 NICUs withheld participation, which could have skewed the results. The data was also not independently verified, and being self-reported, and unblinded, which could be a source of bias.
Finally, delayed effects of the lockdown on women’s health have not been explored. The researchers project much stronger studies of the epidemiology of the disease using data from neonatal care units and national registries, as well as on the children born during this period.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources