Since its emergence in December 2019, in Wuhan, China, the coronavirus disease 2019 (COVID-19), caused by infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has led to more than 1 million deaths worldwide.
COVID-19 is a raging pandemic that has affected all walks of human life. Yet, to date, there are no specific and effective therapies that can reduce the morbidity and mortality of this SARS-CoV-2 infection.
While vaccines are on their way, validated targets are needed to explore therapeutic solutions for COVID-19 further. One such validated target is the circulating proteins.
Combining the information from human genetics and the thousands of circulating proteins, the probability of an accelerated arena of COVID-19 therapies improves significantly.
Sirui Zhou et al., in a recent medRxiv* preprint paper, identify circulating proteins influencing COVID-19 susceptibility and severity by employing a large-scale two-sample Mendelian randomization (MR) study. It is a challenge to disentangle the causal relationship between circulating proteins and COVID-19 susceptibility or severity.
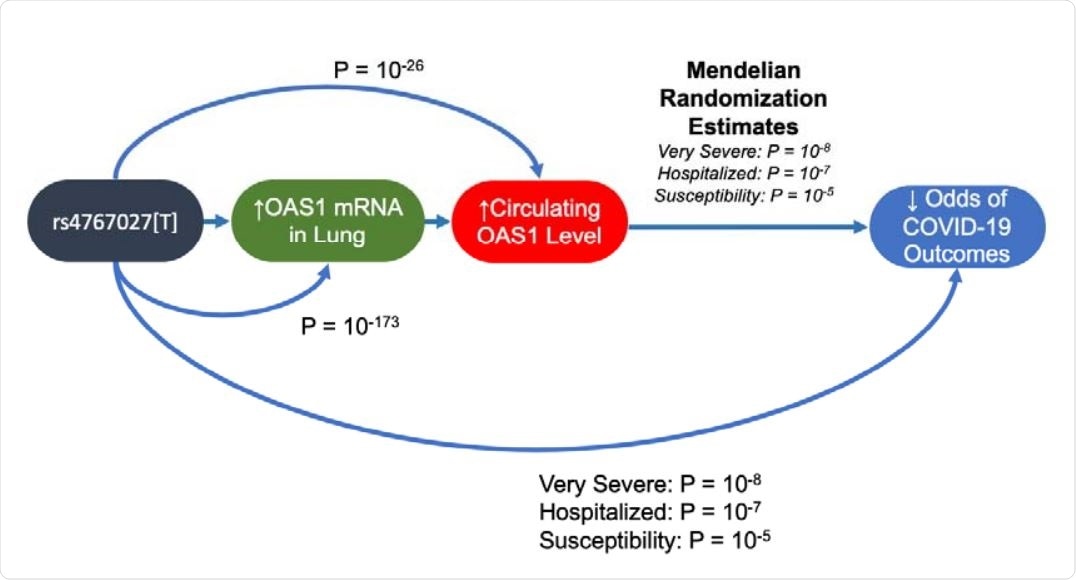
Summary of Evidence Supporting a role for OAS1 in COVID-19 Outcomes

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This study design rapidly scans hundreds of circulating proteins and reduces any bias that may arise due to confounding and reverse causation.
Confounding variables obscure the ‘real’ effect of an exposure on outcome. Confounding happens when both the circulating protein and COVID-19 share a common cause. Reverse causation is when the exposure-outcome relation is biased due to other environmental factors, leading to an unexpected result that interferes or masks the actual result. Here, the reverse causation occurs when COVID-19 itself influences the level of a circulating protein.
To address such limitations, the researchers use the Mendelian randomization (MR) - a genetic epidemiology method that uses genetic variants as instrumental variables, to test the effect of an exposure (protein levels in this study) on an outcome (here COVID-19 outcomes). As the genotypes are randomly assigned at conception and before the disease onset, the MR studies are not affected by reverse causation.
However, the MR method has three core assumptions: 1) the genetic variants must be associated with the exposure of interest, 2) they do not affect the outcome, except through the exposure of interest (i.e., a lack of horizontal pleiotropy), and 3) they do not associate with the confounders of the exposure-outcome relationship.
The researchers identified the genetic determinants of circulating protein levels in large-scale protein level GWASs (genome-wide association studies). They then selected the SNPs (single nucleotide polymorphisms) associated with circulating proteins, which were proximal to their encoded genes (cis-pQTLs).
They assessed if these genes were associated with COVID-19 outcomes in the ICDA Host Genetics Initiative COVID-19 outcomes GWASs (https://www.covid19hg.org/results/), and then undertook MR analyses to estimate the effect of the circulating protein level of COVID-19 outcomes.
In this study, multiple sensitivity analyses were conducted to probe MR assumptions. The results obtained were consistent throughout. The study assessed 955 proteins for three COVID-19 outcomes in ~17,600 cases and 1.3 million controls.
The evidence showed increased OAS1 and IL 10RB levels strongly associated with reduced COVID-19 susceptibility and severe outcomes. In this context, the researchers point out that therapies activating OAS1 may be considered to reposition towards better COVID-19 treatments.
While de novo drug development will take time, understanding the circulating proteins will enable better patient therapies.
The undertaken study of the etiology of circulating proteins in COVID-19 infection is a challenging goal because, in such cases, the infection itself causes changes in the circulating proteins.
In conclusion, the researchers found significant evidence that OAS1 has a protective effect on COVID-19 susceptibility and severity. Based on this result, the researchers suggest exploring interferon beta-1b and PDE12 inhibitors, which are known to increase OAS1 levels and further understand the role in COVID-19 outcomes.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Circulating Proteins Influencing COVID-19 Susceptibility and Severity: a Mendelian Randomization Study, Sirui Zhou, Guillaume Butler-Laporte, Tomoko Nakanishi, David Morrison, Jonathan Afilalo, Marc Afilalo, Nofar Kimchi, Zaman Afrasiabi, Nardin Rezk, Meriem Bouab, Charlotte Guzman, Louis Petitjean, Xioaqing Xue, Christos Tselios, Branka Vulesevic, Yiheng Chen, Vincent Mooser, Vincenzo Forgetta, Daniel Kaufmann, Brent Richards, medRxiv 2020.10.13.20212092; doi: https://doi.org/10.1101/2020.10.13.20212092, https://www.medrxiv.org/content/10.1101/2020.10.13.20212092v1
- Peer reviewed and published scientific report.
Zhou, Sirui, Guillaume Butler-Laporte, Tomoko Nakanishi, David R. Morrison, Jonathan Afilalo, Marc Afilalo, Laetitia Laurent, et al. 2021. “A Neanderthal OAS1 Isoform Protects Individuals of European Ancestry against COVID-19 Susceptibility and Severity.” Nature Medicine 27 (4): 659–67. https://doi.org/10.1038/s41591-021-01281-1. https://www.nature.com/articles/s41591-021-01281-1.