Researchers in the United States and Israel have conducted a study showing that women who have coronavirus disease 2019 (COVID-19) are twice as likely to experience acute clinical stress while giving birth, compared with women giving birth who do not have the illness.
Women with COVID-19 are more likely to perceive more pain during childbirth and more likely to give birth to newborns that need to be transferred to neonatal intensive care.
The adverse outcomes appeared to be associated with restrictions regarding visitors and support companions.
Up to one-quarter of women with COVID-19 were not allowed to have visitors during their hospital delivery stay. Women who had no visitors were six times more likely to report acute stress during birth, compared with women who did have COVID-19 but were allowed visitors.
“The findings underscore an increased risk for childbirth-induced psychological morbidity in COVID-19-affected populations,” writes the team from Massachusetts General Hospital and the Interdisciplinary Center in Herzliya in Israel.
“As hospitals continue to revise policies concerning visitor restrictions, attention to the wellbeing of new mothers is warranted,” says Sharon Dekel and colleagues.
A pre-print version of the paper is available on the medRxiv* server, while the article undergoes peer review.
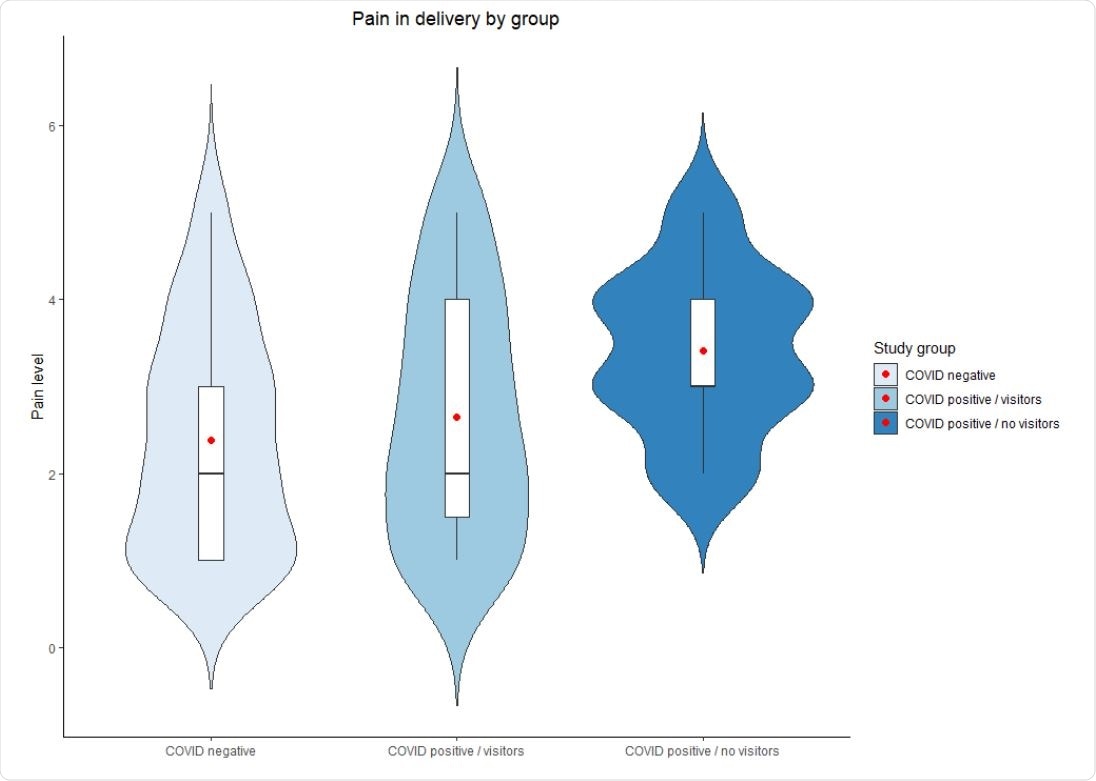
Pain in delivery by study group. Red dots represent the mean.
Delivering mothers among the few populations still entitled to hospital care
While the COVID-19 pandemic has swept the globe causing an unprecedented public health crisis, many non-emergency hospital-based visits and procedures have had to be postponed.
Pregnant women reaching the delivery stage have been among the very few groups of individuals that have continued to receive care in the hospital setting.
A significant proportion of these women had suspected or confirmed COVID-19 while they were giving birth. As well as potentially suffering from symptoms of the illness, they may have been worried about transmitting the virus to their infant or others in the hospital.
“At present, the impact of being COVID-19 positive, confirmed or suspected, on the childbirth experience and maternal and neonatal outcomes remains unclear,” write Dekel and colleagues.
The researchers say it is important to consider the potential of increased psychological adversity during labor and delivery among women with COVID-19.
“To the best of our knowledge, no study has examined how giving birth while potentially being ill with the virus may amplify acute traumatic stress responses to childbirth,” they add.
The researchers say one essential point to consider is the potential effects of social isolation.
Mothers who have COVID-19 may be drastically restricted in terms of being allowed visitors or support companions, both while they endure labor and delivery and during their postpartum stay.
“They may also have gone without visitors while being separated from their newborn to reduce additional transmission risks,” the team points out.
What did the researchers do?
Dekel and colleagues launched a survey on April 2nd, 2020, during the midst of the COVID-19 pandemic in the United States, with the aim of understanding more about the impact of COVID-19 on childbirth and maternal mental health.
Among a large sample of 2,417 women who gave birth while COVID-19 was prevalent in the United States, 68 reported having suspected or confirmed COVID-19 (also referred to hereafter as COVID-19 positive).
Based on a wide range of background factors such as demographics, prior mental health, and trauma history, this group was matched with COVID-19-negative women who also gave birth during the pandemic’s outbreak.
“This rigorous matched-control group approach has not been implemented in previous studies and allows for the generation of knowledge on the potential adverse influence of COVID-19 infection status of birth outcomes while controlling for background factors that are associated with COVID-19 infection and negative maternal outcomes,” says the team.
What did the team find?
The researchers found that COVID-19-positive women were up to two times more likely to experience acute stress during childbirth than COVID-19-negative women.
The COVID-19 positive women were more likely to experience higher levels of pain during childbirth, even though no significant between-group differences were identified for factors such as obstetrical complications, the use of pain medication, or the mode of delivery.
“These findings underscore how childbirth can become a traumatic experience and evoke an acute stress response for women with the novel coronavirus,” say Dekel and colleagues.
The adverse outcomes were associated with visiting restrictions
Hospital policies enforcing visiting restrictions were frequently implemented in cases where women had suspected or confirmed COVID-19.
As much as 25% of these women had no visitors during their hospital stay.
The COVID-19-positive women were 11 times more likely to not be allowed a support companion during their delivery stay, compared with COVID-19 -negative women.
They were also significantly more likely to be separated from their newborns, who were nearly four times as likely to be admitted to neonatal intensive care.
Women with COVID-19 who had no visitors were six times more likely to report clinical acute stress during their delivery stay than women with COVID-19 who were allowed to have visitors during their stay.
“More research is needed to optimize maternal care”
The researchers say the findings may be useful for informing clinical policies during the COVID-19 pandemic.
“While much attention has been paid to the physical symptoms in mothers with COVID 19, our study emphasizes the importance of considering mothers’ psychological wellness,” they write.
“As hospitals around the world continue to update their delivery protocols for COVID-19-positive women and determine risk and benefits of visitor restriction policies, more research is needed to optimize maternal care during these unprecedented times,” concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources