The long-awaited roll-out of vaccines against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has finally begun, with several vaccines having received authorization in the USA, Europe, and Asia. However, the supply of vaccines is still limited, making it necessary to plan vaccine distribution over a large population strategically.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Current situation in the USA
The first two vaccines to receive emergency use authorization from the US Food and Drug Administration (FDA) were the Moderna and Pfizer-BioNTech vaccines, which are reported to have an efficacy of over 94% in preventing symptomatic COVID-19 infection. According to which front-line workers and others at high risk of infection were assigned top priority, a prioritized vaccination schedule was then rolled out.
Of the almost 30 million doses distributed among the states, about 10 million had already been administered by January 13, 2021. In the current study, the researchers modeled the effects of rolling out the vaccine at various times, in various orders of priority, and in single vs. double dose regimens, concerning the population-level mortality. The model was based on age and risk parameters.
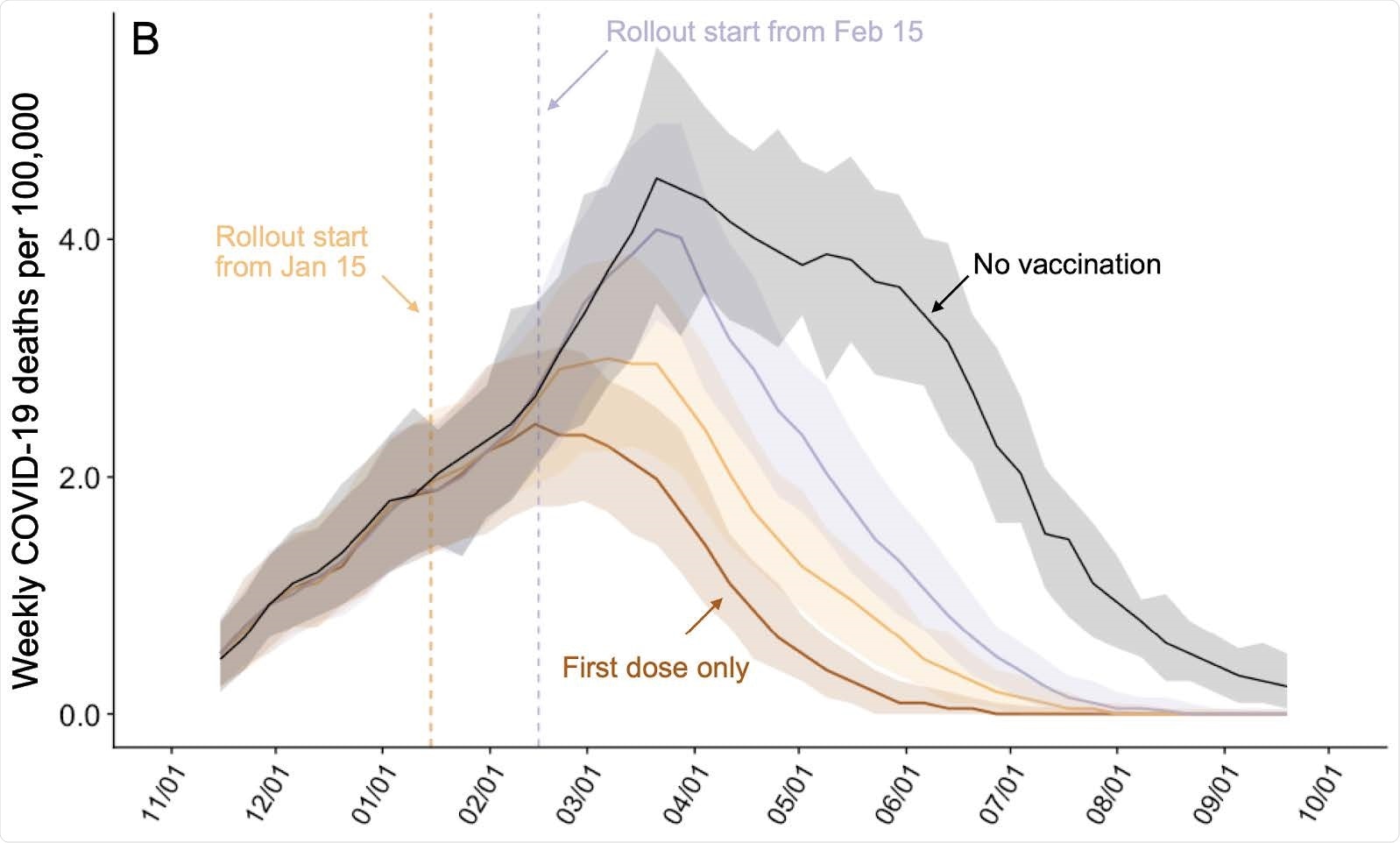
Projected COVID-19 mortality in the Austin-Round Rock MSA from November 8, 2020 to September 17, 2021 under various vaccine rollout scenarios. Weekly incident COVID-19 deaths per 100,000 assuming intermediate (70%) uptake (9) without vaccine (black) or under a ten-phase risk-based rollout of a 95% efficacious infection-blocking, starting either January 15 (orange) or February 15 (purple). The brown line assumes that only first doses are administered starting January 15. Solid lines and shading indicate the median and 95% CI across 200 stochastic simulations, respectively.
Study model
The study model centered on Austin, a city in Texas, with the number of COVID-19 deaths being projected over eight months following the deployment of two types of vaccines: one that prevents infection by rendering the vaccinated individual less susceptible to, and the other targeting symptomatic infection. The study is based on the assumption that the vaccine is leaky, resulting in a 95% reduction in susceptibility.
The date of vaccine roll-out is either January 15 or February 15, and the weekly quota of vaccination is estimated to be 10 million. Vaccine allocation to each city is on a pro-rata or proportional basis.
The model compared three strategies, one that distributes the vaccine on a first-come, first-served basis; one which prioritizes three groups before vaccinating the general public, namely, those over 65 years, those with high-risk medical conditions, or both; and a ten-phase strategy with sequential administration of the vaccine to age-risk groups that are at descending risk for severe COVID-19 outcomes. The study assumes that about 8% of individuals have become immune following natural infection by this date.
Infection-blocking vaccine
In the third scenario, with perfect risk-prioritization being adhered to in vaccine roll-out, with a vaccine that prevents infection, the researchers estimate a 52% reduction in deaths due to COVID-19 compared to unvaccinated controls if 50% of the population is vaccinated. If 90% coverage is accomplished, 56% of deaths would be prevented.
If the coverage is low, that is, 50%, priority-based vaccination is mostly irrelevant. At 90% coverage or more, the ten-phase strategy is superior initially, following which those over 65, and young adults at high risk, are prioritized.
Symptomatic infection-blocking vaccine
With a vaccine that blocks only symptomatic infection, the effect of 50% coverage beginning January 15, using the ten-phase strategy, is estimated to be capable of reducing the death toll by 40%, compared to 32% with unprioritized roll-out strategies. Suppose the coverage under the ten-phase strategy is 89% with a single dose. In that case, the estimated reduction is 50% and 66%, respectively, for a vaccine that blocks only symptomatic disease and one which prevents infection as well.
With these findings as a basis, high-risk groups should be prioritized. With a delayed roll-out in February 2021, at only 50% uptake, giving the vaccine to those over 65 and those at high risk may prevent about 17,000 deaths in excess of a non-prioritized schedule.
Delay in roll-out is the deadliest parameter
On the other hand, the single factor associated with a more significant number of deaths in both the USA and Europe is a delay in vaccine roll-out, compared to either poorly prepared or executed prioritization plans or unwillingness to take the vaccine.
At this point, thousands of deaths are occurring daily in these countries. As new variants begin to take over in many of these regions, with even greater transmissibility, the process of ensuring that vaccination reaches susceptible people before the virus does is the greatest challenge. This is more so because, in contrast to preventive seasonal influenza campaigns, which occur before the influenza virus begins to circulate freely, COVID-19 vaccination is emerging on a stage where the causative virus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is in full cry already.
Single-dose expanded programs
Some immunization programs have chosen to expand the reach of the first dose of the vaccine rather than complete the two-dose regimen in as many people as possible. The hope is that the partial immunity elicited by the first dose will still be more effective in reducing the number of deaths, compared to achieving much higher immunity in half the number of people.
However, the USA has expressed disagreement with this approach, due to the absence of any clinical trial data demonstrating the utility of a single-dose regimen. It is against this background that the current study models a situation in which providing just one dose of either type of vaccine, at 80% efficacy, would probably prevent more deaths than insisting on two doses for all participants.
What are the implications?
The researchers point out that more information must be gathered about vaccine efficacy following single-dose trials since more assumptions are being made about the type of onset, the duration of immunity, and the eventual outcome of vaccination, whether prevention of infection, symptomatic disease, or any combination of both. The actual performance of the model also depends on the susceptible fraction of the population, the changes in the behavior of the people over time or following vaccination,
However, the study strongly suggests that distributing vaccines by priority should not slow down the roll-out, as has been seen in the USA.
The researchers describe their plan: “Our projections suggest two immediate strategies to amplify the impact of COVID-19 vaccines in the US––hybrid distributions that combine active outreach to priority groups with passive distribution to the general public and foregoing plans to hold second doses in reserve.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Wang, X. et al. (2021). The impacts of COVID-19 vaccine timing, number of doses, and risk prioritization on mortality in the US. medRxiv preprint. doi: https://doi.org/10.1101/2021.01.18.21250071. https://www.medrxiv.org/content/10.1101/2021.01.18.21250071v1
- Peer reviewed and published scientific report.
Wang, Xutong, Zhanwei Du, Kaitlyn E. Johnson, Remy F. Pasco, Spencer J. Fox, Michael Lachmann, Jason S. McLellan, and Lauren Ancel Meyers. 2021. “Effects of COVID-19 Vaccination Timing and Risk Prioritization on Mortality Rates, United States.” Emerging Infectious Diseases 27 (7). https://doi.org/10.3201/eid2707.210118. https://wwwnc.cdc.gov/eid/article/27/7/21-0118_article.