Diagnostic testing, contact tracing, and the isolation of infected individuals and their contacts form the foundation of managing the current coronavirus disease 2019 (COVID-19) pandemic. Moreover, the number of positive tests is a key measure of the severity of the outbreak at regional, national, and international levels.
The true number of infections with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is also essential to calculating the disease's actual incidence and the infection mortality rate. In addition, it helps to understand how effective control measures are at containing viral spread.
However, many infected individuals are never tested, and many others are falsely declared negative due to poor test sensitivity. Thus, the total number of cases is not known. A new preprint research paper posted to the medRxiv* server estimates the number of infections that are diagnosed from testing alone as being about a fourth of the total.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Two data sources
Testing symptomatic individuals with a fairly sensitive test typically results in underestimating the total number of infections but is essential to identify hotspots of transmission.
On the other hand, random testing provides a more accurate estimate of the overall prevalence of infection, but cannot be applied to infection clusters. Both types of data were available for the researchers to answer the question of the proportion of total infections identified by testing.
The researchers used a number of data sources from England to arrive at their estimate, combining the positive test results with the range of the incubation period and the variation in test sensitivity with time. The sources were the daily publication of the number of positive tests among suspected infected individuals by the UK government; and the publication of the population prevalence by the Office for National Statistics (ONS).
The former is based on several diagnostic tests. One is polymerase chain reaction (PCR) testing, the sensitivity of which varies with the phase of the infection. Another is the use of rapid point-of-care testing with lateral flow devices (LFDs), using to screen possible contacts or infected individuals in schools, residential care centers, and other settings where the risk of transmission is high. These are relatively less sensitive than the PCR, especially when not performed by professionals but yield faster results.
The ONS data is based on randomized sampling and is more accurate. The researchers adjusted the number of diagnostic tests against the ONS data to reach their estimate.
Impact of VOC
The newly emerging variants of the SARS-CoV-2 virus pose a challenge in terms of different clinical presentations. This may be accompanied by varying incubation periods, different rates of viral shedding, and a different pathology.
These new variants may also result in differences in the test results as well as in the number of people who seek testing. This will, of course, affect the proportion of infections that are reported by diagnostic testing.
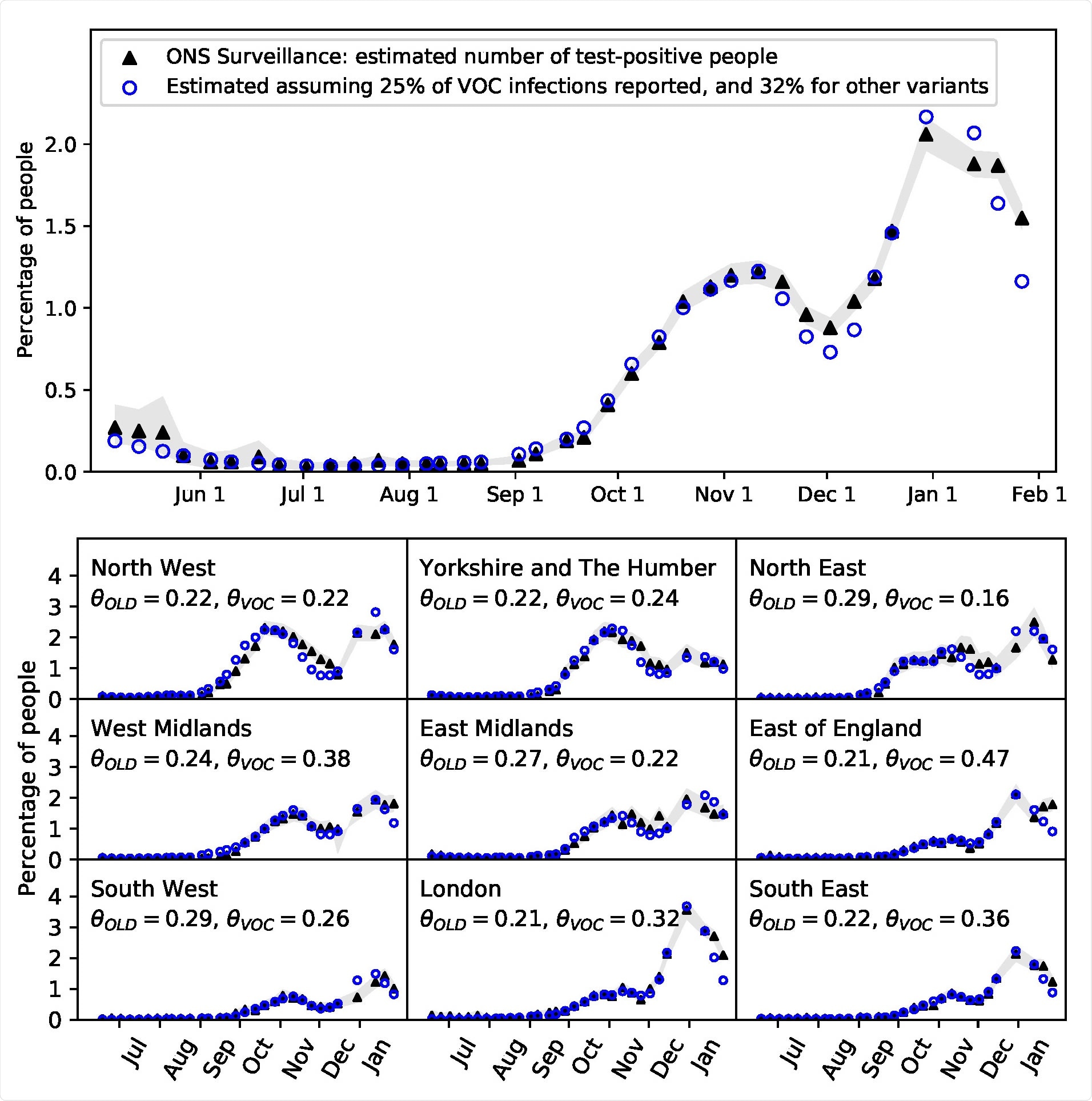
The number of SARS-CoV-2 test-positive people in England (top) and in each of the 9 regions of England (bottom). Blue circles show the estimate given by Eq.(6), black triangles show the ONS infection survey data.
Differences in reporting rate by region
The differences in the proportion of reported cases by region and over time could be a new way to understand how these variants present. The southern regions of England show a noticeable difference in case reporting compared to the others, in that percentages of reported infections increased until the start of December 2020. In other regions, the percentages went down. This is despite the fact that testing increased steadily in all regions and was exclusively carried out by PCR at this time.
Increase in reported infections
The increase in reported infections across all regions during November and December 2020 may be partly, at least, due to the increasing proportion of infections caused by the UK variant of concern (VOC) in this period. Since some proof exists of this variant's higher virulence compared to the parental strain, it may result in a higher reported rate of infections.
Another reason could be the adoption of Lateral Flow Device (LFD) testing for widespread screening, increasing the number of asymptomatic infections reported. Therefore, the researchers excluded the estimated number of positive LFD tests from the total to obtain an estimate of the percentage of infections reported with a positive PCR.
With a higher assumed rate of LFD positivity, the percentage of reported infections caused by the VOC drops.
VOC has higher reporting rates
Nonetheless, the VOC has a higher proportion of reported cases than the older variants, indicating that this is the primary reason for the increase in reported cases from November onwards. This assumes that the positive proportion of LFDs remains constant over time.
Overall, they found that 25% of non-VOC variants were reported overall in England, varying by region. If the LFD positivity is taken to be zero, 32% of VOC infections were reported.
VOC may have a longer detection period
They also explored the possibility that the detection of infections caused by the VOC could occur over a more extended period, that is, for more than three weeks after exposure. In such a case, an infection detected after three weeks from exposure (historical infection) would more likely be part of the ONS estimates than the daily test positivity reports.
It is assumed that historical infections are more likely to have been detected if the PCR cycle threshold is high. In such a case, the tests used for ONS sampling surveys should have mean cycle thresholds corresponding to the percentage of historical infections.
Indeed, the researchers found that the highest ONS cycle thresholds correlated with periods when their prevalence estimates were below the ONS figures. In several regions, the reporting rates showed inverse correlations with the cycle threshold values reported by the ONS, lending support to the postulate that test sensitivity also contributes to the changes in reporting of VOC infections.
What are the implications?
The report shows significant variation in the proportion of positive tests in England. The researchers attribute this to differences in test-seeking between the north and south of England. Towards the end of the year, there have been marked reductions in tests requested in the northern regions, leading to uncontrolled viral spread.
This observation must be confirmed, as it has important implications for determining how the infection is likely to spread and what control measures are most beneficial.
About 25% of older variants are being reported, while the VOC seems to have a higher reporting rate, at 32%. The VOC may have a higher reporting rate, accounting for this change. However, other factors may also be at work.
The abrupt shift may be a clue to still other changes that have passed unrecognized until now. If so, the state of current knowledge about SARS-CoV-2 may soon reveal itself to be obsolete.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources