With the COVID-19 pandemic continuing to affect many parts of the globe, our understanding of the short-term and acute effects of the disease has been growing, but its consequences on long-term health are still poorly known. Some studies report individuals with symptoms such as fatigue, muscle weakness, and breathlessness six months after severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. These long-term effects are known as Long COVID.
Although children are at lower risk for severe COVID-19, they still have many different symptoms. Some data suggests up to a third of hospitalized children required intensive care, with some children showing multi-organ failure requiring support to breathe. A few children develop a severe condition a few weeks after recovery called multisystem inflammatory syndrome in children (MIS-C).
Data on the long-term effects of severe COVID-19 in children is still limited to small studies. But, these show that more than half the children have at least one symptom that persists even after four months of infection.
In a new study published on the medRxiv* preprint server, researchers followed hospitalized children after discharge to understand the effect of COVID-19 over the long term.
Following hospitalized children after recovery
The researchers studied children admitted to the Z.A. Bashlyaeva Children’s Municipal Clinical Hospital in Moscow between April and August 2020. The team followed up with the parents of these children in February 2021 to complete a survey.
From the hospital medical records, the team obtained information such as demographics, symptoms, co-morbidities, care at the hospital, clinical outcomes. Using the follow-up survey, the team obtained information on persistent symptoms and the children's general physical and psychosocial well-being compared to before COVID-19.
Of the 836 children admitted to the hospital and with accurate contact information, the researchers were able to conduct a follow-up survey of 518 children. The median age of the children was about 10 years,.
The most common pre-existing condition was a food allergy, followed by allergic rhinitis and asthma, gastrointestinal problems, eczema, and neurological problems. About 37% of the children had pneumonia during their stay in the hospital, and about 2.7% had severe disease.
During the follow-up, about one-fourth of the children reported at least one persistent symptom. The most common were fatigue, followed by insomnia. They also reported changed smell and headaches. Most symptoms decreased over time, but sleep disturbances and headaches did not change. This could be related more to psychological mechanisms rather than virus effects. Some symptoms such as fatigue and sleep issues were seen together.
Wellness scores for children with persistent symptoms were much lower than the scores before COVID-19, while children with no long-term symptoms did not report any changes in wellness. Other changes such as decreased appetite, increased sleep, and reduced physical activity were reported to be because of COVID-19. About one in twenty parents attributed changes to COVID-19.
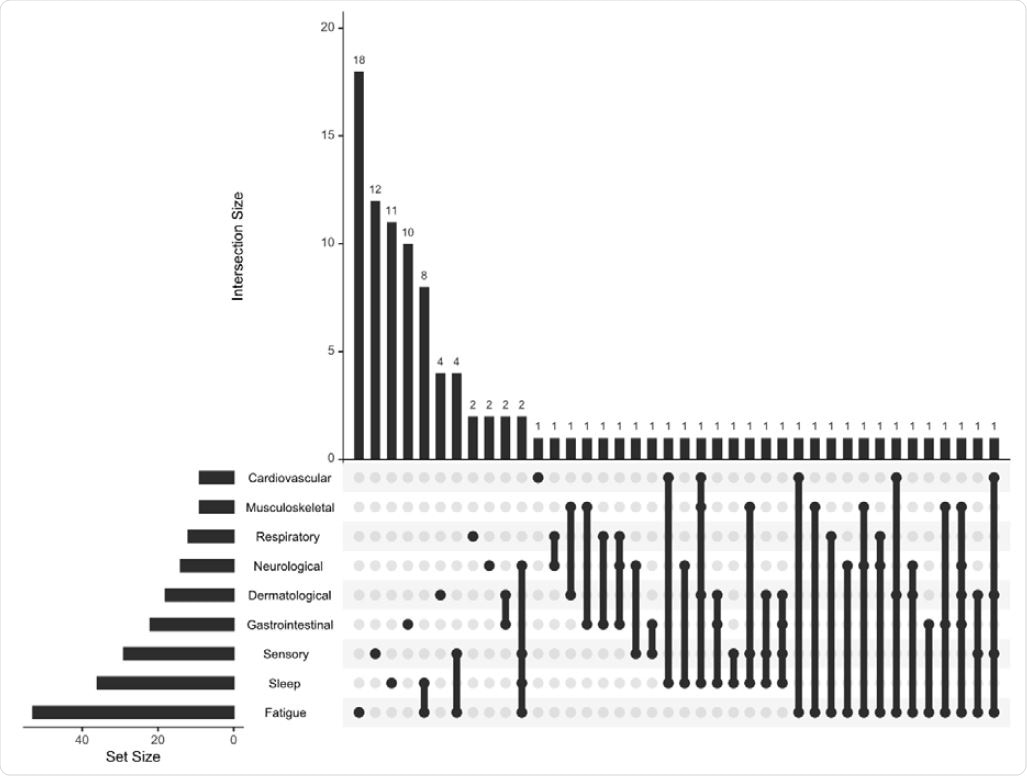
Upset plot representing coexistence of 317 the persistent symptom (present at the time of the follow-up interview and lasting for over 5 months) categories at the follow-up assessment. The values represent the number of individuals experiencing a persistent symptom category or combination of categories. Black lines link multiple symptoms indicated by black dots.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Risk factors for long COVID
Older children, above 6 years, had greater odds of persistent symptoms than children less that 2 years old. In adults also, the risk for long COVID-19 symptoms has been seen to increase with age. Another predictor for long-term symptoms was allergic diseases. This is also similar to what is seen in adults. Studies have reported long COVID in people with asthma. Some reports suggest COVID-19 consequences may be related to mast cell activation, seen in allergic diseases, which may be responsible for long-term consequences of COVID-19.
Since the study is based on the ISARIC COVID-19 Health and Wellbeing Follow-Up Survey for Children, it will help compare with other such future studies. The large sample size and the longest time of follow-up to date is another strength of the study.
The authors do note some limitations. The study was based only on children in Moscow and included only hospitalized children, which is not a very representative population. Only parents or caregivers of the children were interviewed for the follow-up survey and there could be a recall bias risk. Further studies are needed to help better understand the long-term effects of COVID-19 in children and how the risk factors play a role.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Risk factors for long covid in previously hospitalised children using the ISARIC Global follow-up protocol: A prospective cohort study, Ismail M Osmanov, Ekaterina Spiridonova, Polina Bobkova, Aysylu Gamirova, Anastasia Shikhaleva, Margarita Andreeva, Oleg Blyuss, Yasmin El-Taravi, Audrey DunnGalvin, Pasquale Comberiati, Diego G Peroni, Christian Apfelbacher, Jon Genuneit, Lyudmila Mazankova, Alexandra Miroshina, Evgeniya Chistyakova, Elmira Samitova, Svetlana Borzakova, Elena Bondarenko, Anatoliy A Korsunskiy, Irina Konova, Sarah Wulf Hanson, Gail Carson, Louise Sigfrid, Janet T Scott, Matthew Greenhawt, Elizabeth A Whittaker, Elena Garralda, Olivia Swann, Danilo Buonsenso, Dasha E Nicholls, Frances Simpson, Christina Jones, Malcolm G Semple, John O Warner, Theo Vos, Piero Olliaro, Daniel Munblit, Sechenov StopCOVID Research Team medRxiv 2021.04.26.21256110; doi: https://doi.org/10.1101/2021.04.26.21256110, https://www.medrxiv.org/content/10.1101/2021.04.26.21256110v1
- Peer reviewed and published scientific report.
Osmanov, Ismail M., Ekaterina Spiridonova, Polina Bobkova, Aysylu Gamirova, Anastasia Shikhaleva, Margarita Andreeva, Oleg Blyuss, et al. 2021. “Risk Factors for Long Covid in Previously Hospitalised Children Using the ISARIC Global Follow-up Protocol: A Prospective Cohort Study.” European Respiratory Journal, January. https://doi.org/10.1183/13993003.01341-2021. https://erj.ersjournals.com/content/59/2/2101341.