The coronavirus disease 2019 (COVID-19) pandemic caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) led to numerous and sweeping restrictions in many countries, including the UK, limiting social and economic activity.
One reasonable concern raised by many public health researchers was the negative effect of such restrictions, as well as of the redirecting of most healthcare resources towards COVID-19 management on routine medical care, such as infant and childhood vaccinations.
A new study examines this aspect of the pandemic-related regulations, providing an estimate of the immunization rates in Scotland and England, two neighboring countries with independent national healthcare systems.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Background
Not only did healthcare systems reconfigure themselves to increase acute and intensive hospital bed capacity and attending staff, by canceling elective procedures and most screening programs, but patients themselves stopped seeking both elective and emergency care over the period of lockdown, for instance. It is noteworthy that child health services were not suspended at any period within the UK.
High vaccine coverage is essential to allow direct and indirect immune protection against other infectious diseases. However, the World Health Organization (WHO) warned against allowing routine immunization rates to drop, as claimed by more than 80 countries, including the UK, USA, and Singapore, during the early part of the pandemic.
Since indirect measures were relied on to arrive at this conclusion, the scientists in this study, available as a preprint on the medRxiv* server, carried out an observational study, analyzing the “natural experiment” of the pandemic by comparing vaccination rates just before, during and after the first COVID-19 lockdown in these two countries, beginning on March 23, 2020.
The vaccines included in this study included the 6-in-1 DTaP/IPV/Hib/HepB vaccine and the Measles, Mumps and Rubella (MMR) vaccine. The first vaccine is recommended to be given at four-week intervals beginning at eight weeks of age, and the second at 12 months, and 40 months, respectively.
In Scotland, timely vaccine uptake was reckoned to occur within four weeks of the due date; in England, due to the lack of data, timely uptake was reckoned as uptake at six months for the first and 16 months for the first dose of the second vaccine, respectively.
What did the study find?
Vaccine uptake increased during the pre-lockdown, lockdown, and post-lockdown periods and in 2019, a pre-pandemic period. The lockdown period was taken as March 23 to July 31, 2020.
In Scotland, the pre-school 6-in-1 vaccine uptake was already high, at 94% in 2019. The first dose of the vaccine was given to 1.3% more children relative to 2019, being given to >95% during the lockdown and post-lockdown periods. With the second dose, the baseline uptake of 85% increased to ~90% during the lockdown, declining slightly to 89% in the post-lockdown period, but still above the 2019 rate.
The third dose of the 6-in-1 vaccine had a 2019 uptake of 73%, which increased during the lockdown to 82%, falling slightly to 80% post-lockdown.
This means that 7,500 more children in the infant/pre-school group were immunized on time during this period compared to the 2019 rates. The lowest rate was just before the lockdown began, followed by a rise to peak levels in June and then a decline, though still above pre-pandemic levels.
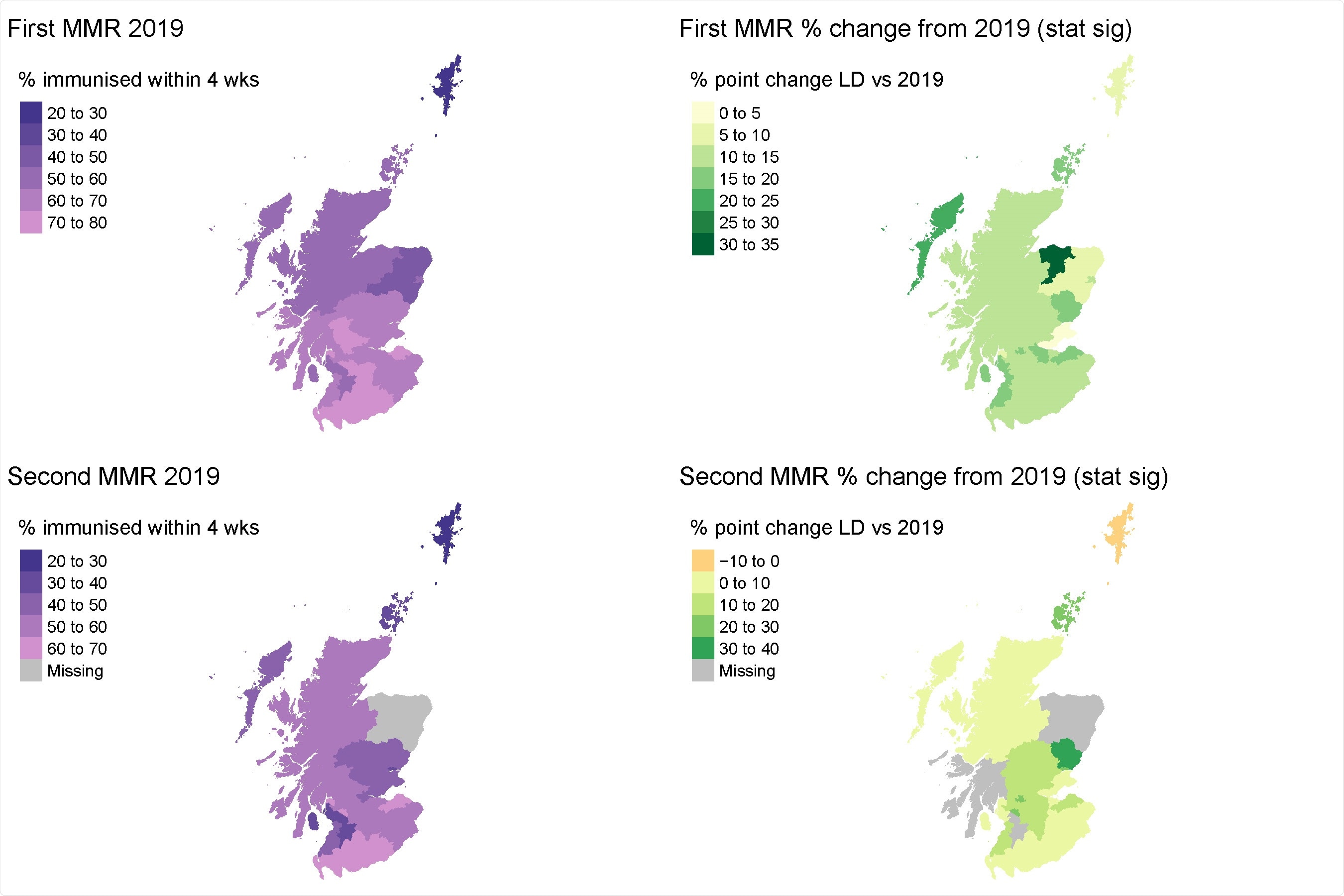
Conversely, the MMR vaccine uptake had already gone up a little before the lockdown began. With the MMR vaccine, the baseline percentage of 65% increased to >67% in the pre-lockdown period, before shooting up to >78% during the lockdown. In the post-lockdown period, it went down a little to 75%.
With the second dose, the 2019 uptake was 52%, going up to 53% in the pre-lockdown period, and then by 14% more during the lockdown, at 66%. Post-lockdown, it went down slightly to 63%.
Overall picture
All vaccines thus averaged an increased mean uptake. When the 31 individual Health and Social Care Partnerships (HSCP), the local area in which the children live, is analyzed, a small number of regions have shown a reduction in vaccine uptake during the pandemic.
The improvement is seen to be due to a significant rise in 8/31 HSCPs, mostly in the thickly populated urbanized central region of Scotland. However, a rise in MMR uptake was seen to occur with both doses, at up to 30% of 2019 values.
Post-lockdown, the increase over the baseline persisted except for the first dose of the hexavalent vaccine, which was increased only in the lowest deprivation quintile (the poorest or least cared for children).
Deprivation associated with increased uptake
The social deprivation measures were associated with rising uptake of vaccines even before the lockdown, except for the first 6-in-1 vaccine that was found to be linked to a higher intake only in the most deprived quintile. Overall, this corroborates the differential rise with the two types of vaccine since the uptake of the two MMR doses became noticeably more different with the degree of deprivation.
The first MMR dose was taken up in more significant numbers for moderately and severely deprived children, but for the second, only the most deprived. Whatever the factors that led to higher MMR vaccine uptake, they appear to have worked more effectively among these children.
Thus, lockdown led to a higher catch-up with infant and pre-school immunizations, but the final uptake varied between age groups. That is, there may be a ceiling effect limiting maximal uptake, depending on the earliest vaccination.
England demonstrates a fall in uptake
In England, the vaccine uptake data showed a slight decline for all doses during the lockdown periods relative to the 2019 baseline rate. The reduction ranged from a 0.5% reduction for the first 6-in-1 dose, from the earlier rate of >96%, to 2% for the third dose, down from ~89%.
Significantly, the uptake for both vaccines had already begun to fall before the lockdown began, with this trend being most noticeable in the pre-lockdown period.
What are the implications?
“This is an important message … and will help normalize timely immunization uptake for both parents and health services. Improving public and professional confidence is particularly vital given in the current climate of promoting vaccination against SARS-CoV-2.”
The data here should not be stretched beyond their limits, and further work is required to understand what contributes to better vaccine uptake. For example, many parents could not easily get appointments for vaccination or childcare. Others had vaccine hesitancy due to concerns about adverse effects exacerbated by misinformation shared via social media.
Increased accessibility of vaccination centers, or providing public transport, or by ensuring transport to families shielding vulnerable members, could help preserve and enhance uptake. Using reminder services could also help, not just to remember vaccination dates but to discuss concerns with a healthcare professional, which is a rewarding strategy in modulating such fears.
The government of Scotland also put in due effort to prevent immunization delays, which appears to have paid off.
Conversely, an earlier survey in England showed that some parents with young children did not know if immunization was still continuing, especially minority groups. Secondly, some parents felt that the risk of these diseases was lower due to the restrictions on social interaction, especially with fewer colds, coughs, and fevers.
“We have demonstrated that a robust child immunization service can continue to deliver high and even increasing uptake rates. The challenge now is to use and expand on this knowledge to promote future vaccination programs, including those targeting SARS-CoV-2.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources