Globally, millions of individuals with HIV reside in urban locations, where structural and socioeconomic variables drive inequalities in accessing healthcare services and thus contribute to HIV epidemic propagation. Cities must have adequate healthcare infrastructure that authorities could exploit to mitigate HIV transmission. The HIV-containment potential of interventional strategies at urban locations has been demonstrated previously in multiple cities. The H-TEAM program commenced in 2014 using an integrated methodology to decrease the incidence of HIV infections in Amsterdam.
 Study: A 95% decline in estimated newly acquired HIV infections, Amsterdam, 2010 to 2022. Image Credit: Paulo Amorim / Shutterstock
Study: A 95% decline in estimated newly acquired HIV infections, Amsterdam, 2010 to 2022. Image Credit: Paulo Amorim / Shutterstock
About the rapid communication
In the current rapid communication, researchers described the H-TEAM approach that contributed to the remarkable decrease in HIV infections in Amsterdam from 2010 to 2022.
The 2010 HIV scenario and H-TEAM
H-TEAM initiative efforts in Amsterdam have attained success due to data availability on HIV transmission, incidence, and prevalence. Stichting HIV Monitoring (SHM) collects data from more than 98% of Dutch individuals seeking care for HIV infections, with care recipients receiving written information regarding the acquired immunodeficiency syndrome (AIDS) Therapy Evaluation in the Netherlands (ATHENA) study participation and being informed by attending physicians of the reason for data collection.
Pseudonymized data is provided to research personnel for scientific reasons, such as HIV incidence calculation. SHM data, including HIV sequencing information, is used to assess HIV transmission among the residents of Amsterdam. A recently published study reported that between 2014 and 2018, 67% of incident infections were among individuals residing in Amsterdam. The findings highlight the potential of city-level HIV-targeted interventions among Amsterdam residents.
In 2010, 300 individuals received an HIV infection diagnosis in Amsterdam, with 78% being males who had sex with males (MSM). Standard HIV care and prevention measures led to a persistent drop in the yearly HIV incidence after 2010. However, the count of newly acquired infections by the virus was lower than that of new diagnoses.
H-TEAM interventions brought together stakeholders from civil society, public health, the main impacted communities, the Patient Association of The Netherlands, HIV physicians, and general practitioners in Amsterdam to develop and execute an interdisciplinary approach to decrease HIV incidence. The initiative comprised combination treatments, including novel test-and-treat plans at general practitioner clinics, pre-exposure prophylaxis (PrEP), hospitals, and CSH, and research on HIV testing barriers and motives.
All treatments were implemented concomitantly, each targeting one aspect of the human immunodeficiency consortium. This coordinated effort was likely to contribute considerably to the remarkable 95% decrease in estimated HIV incidence from 201 to nine between 2010 and 2022, the 79% decrease in incident HIV cases in Amsterdam, and Amsterdam exceeding the 95-95-95 Joint United Nations Programme on HIV/AIDS (UNAIDS) target in 2022.
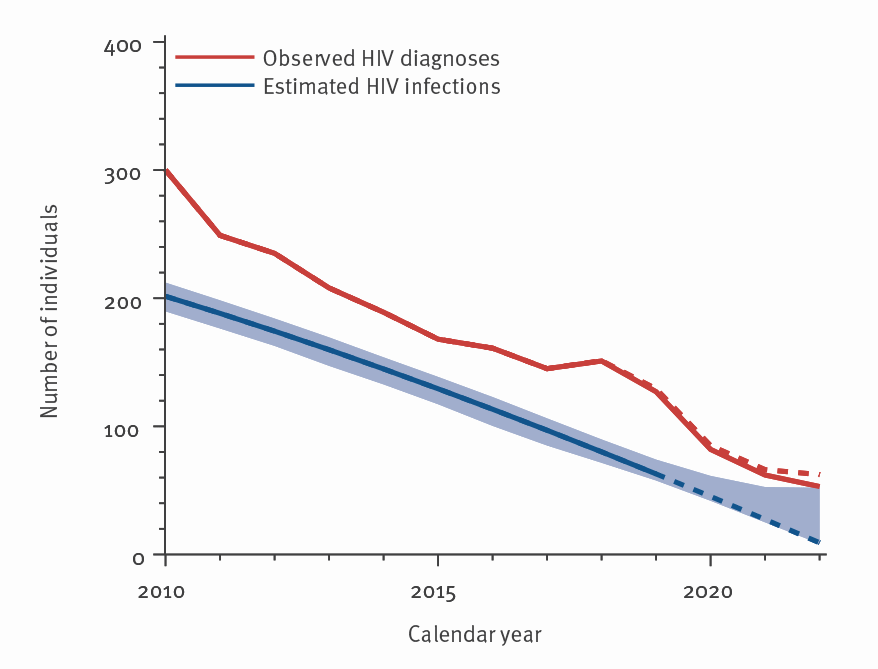
Annual number of observed HIV diagnoses and estimated newly acquired HIV infections, Amsterdam, 1 October 2013: Source for the calculations: European Centre for Disease Prevention and Control HIV Modelling Platform. Red dashed line: number of diagnoses after adjusting for the delay in notification to SHM; blue zone: uncertainty around the estimate; blue dashed line: estimates in 2020 and later, which are still uncertain, as these are sensitive to the observed number of diagnoses in those years.
H-TEAM efforts to prevent HIV infections
PrEP for HIV was introduced in 2015 in Amsterdam, primarily for transgender people (TGP) and MSM individuals. The Amsterdam pre-exposure prophylaxis demonstration project (AMPrEP) showed high uptake and usability, leading the Health Council of the Netherlands to recommend PrEP for the country. Subsidized PrEP and associated care were provided in 2019 to 8,500 people, of which 2,900 resided in Amsterdam.
A study found that over 69% of forward transmissions in the Dutch country occurred among MSM individuals within three months of infection with HIV. This led to the design of the test-and-instantaneous-treat strategy for acutely infected individuals, which allowed TGP and MSM to self-refer via a web-based awareness tool or seek referral by the CSH or general practitioners in Amsterdam.
The strategy used symptom recognition scores, adapted to fit AHI patient characteristics, obtained through point-of-care human immunodeficiency virus ribonucleic acid (RNA) tests and the website’s symptom checker tool. This strategy significantly reduced the duration between the diagnosis of acute HIV infections (AHIs) and suppression of viral load, leading to its adaptation in clinical care at sexual health centers in 2019 in Amsterdam.
Post-implementation, there was a rise in the percentage of newly identified TGP and MSM individuals with recent HIV infections in Amsterdam. However, reducing the percentage of people diagnosed with advanced-stage HIV infections remains challenging. In 2019, indicator-based HIV testing was performed in Amsterdam to enhance compliance with HIV indicator-based testing recommendations in hospitals.
Conclusions
Based on the findings, Amsterdam has achieved a 95% drop in incident HIV infections and a 79% reduction in HIV infection diagnoses through a city-centered approach to HIV prevention and care. However, a few individuals continue to be viraemic due to not being diagnosed or disengaged from care. Data on these individuals is unavailable, possibly due to death or relocation.
H-TEAM initiative stakeholders are investigating new intervention strategies to increase outreach to affected individuals, including tailored healthcare and pre-exposure prophylaxis and providing detailed sociological and epidemiological information on the HIV outbreak using geographical data systems. This data, combined with successful projects on HIV testing, prevention, and therapy, could result in the complete elimination of HIV from Amsterdam in the years to come.