The human blood consists of liquid called plasma that comprises white and red blood cells, and platelets. The antibodies and antigens present in the blood help to identify one’s blood group. The proteinaceous substance inside the plasma is called antibodies. Antibodies are a part of body's natural defense.
They alert the immune system by identifying foreign substances, such as microorganisms, and destroying them. The protein molecules found on the surface of red blood cells are called antigens.
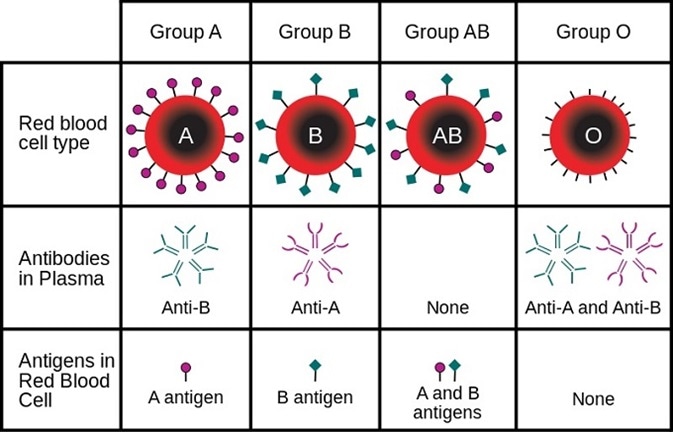
Image author: InvictaHOG / commons.wikimedia.org
Major divisions of blood
ABO system defines four main blood groups.
- Group A: It contains A antigens in the red blood cells with anti-B antibodies in the plasma.
- Group B: It contains B antigens with anti-A antibodies in the plasma.
- Group O: It contains anti-A and anti-B antibodies in the plasma, but antigens are absent.
- Group AB: It contains A and B antigens, but antibodies are absent.
Sub-types of blood group
These main blood groups are sub-divided into eight types and each can be either RhD negative or RhD positive. One can have any one of these eight blood groups:
- A+ (A RhD positive) and A− (A RhD negative)
- B+ (B RhD positive) and B− (B RhD negative)
- O+ (O RhD positive) and O− (O RhD negative)
- AB+ (AB RhD positive) and AB− (AB RhD negative)
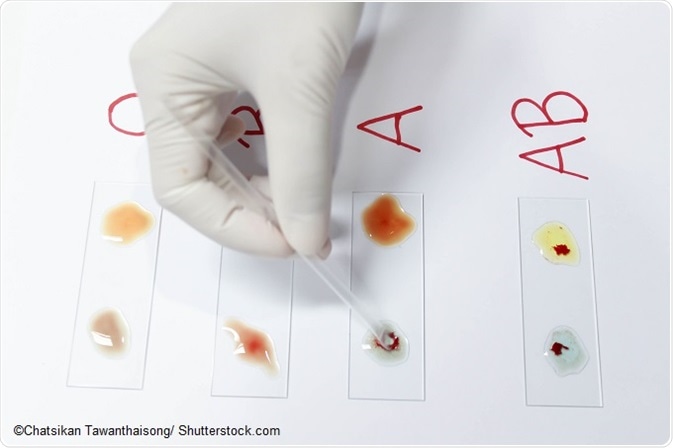
“O” blood group
The most common blood group is “O,” which is found in 48% of the UK population. Hospitals request blood group O very frequently, as half of the donor population has this blood group. The blood group O’s red blood cells are compatible and versatile. They are more compatible with other blood groups of the ABO system, but patients of this group can receive red blood cell transfusions only from their own group.
An important blood group is O negative, which is commonly called “universal.” Red blood cells can be received by patients with blood groups A, B, and O, irrespective of whether they are Rh positive or Rh negative. The O negative red cells are unique and can be safely given to a patient whose blood type is unknown or immediately unavailable.
Therefore, this blood type is necessary in departments such as Emergencies & Accidents; the demand for O negative blood in all hospitals is around 13% but only 7% of the population has this blood.
“AB” blood group
The AB group is the rarest of ABO, because it is found in only 1 in 25 donors. AB red cells can be transfused to patients with AB blood and so this is the rarest of its form. AB is the least requested blood type by hospitals and so it is important to ensure a close balance between collections and hospital requests. Patients with severe blood loss can be treated with the freshly frozen plasma produced by AB blood group. Hence, donors of AB blood group are given high importance.
Sometimes, in a year, the demand for AB positive rises occasionally. The hospitals rely on the female donor's support to receive blood and blood products during the time of demand. Around 1% of the donor population is AB negative, which is the rarest blood type. Since it is rarest, it is hard and difficult to find new donors and collect sufficient amount of blood.
“A” blood group
The second most common blood group found in the donor population is group A. The largest blood group does not mean it is all plain sailing, but it is undoubtedly one of the most requested blood groups by hospitals. Balancing the collections and demand is rigorous. Negative donors have a very important role in making platelets. Platelets are one of the blood components that help prevent bruising and stop bleeding.
Around 60% of platelets are used to help cancer patients. Platelets of group A are constantly in high demand, as they can be given to patients of all ABO groups, making them extremely versatile. A higher priority is given to ensuring a regular and consistent supply of platelets, which can last only up to 7 days (compared to 35 days for red cells).
“B” blood group
Blood group B is found in only 10% of donors. The South Asian (20%) and Black communities (25%) seem to have more group B individuals than the White European communities (9%). To ensure that the patient need for this blood group is met consistently, the clinics encourage new donors from communities such as Black, Asian, and other minorities.
The Black communities are more susceptible to sickle cell anemia and the South Asian communities to thalassemia. During such critical conditions, patients may require multiple transfusions, and sometime throughout their lives. It is important that patients receive blood that is tested extensively to better match their own during regular transfusions.
Around 1 in 7 patients, B negative donors can help Rh positive and negative patients from groups B and AB−. The B negative donors are more in demand, as the hospitals depend heavily on them for the required blood.
Further Reading
Last Updated: Dec 29, 2022