Metformin and its derivatives have been widely used for a long time for the treatment of type 2 diabetes mellitus. It lowers both basal and postprandial (i.e. after eating a meal) plasma glucose and is not chemically or pharmacologically related to any other classes of oral antihyperglycemic agents.
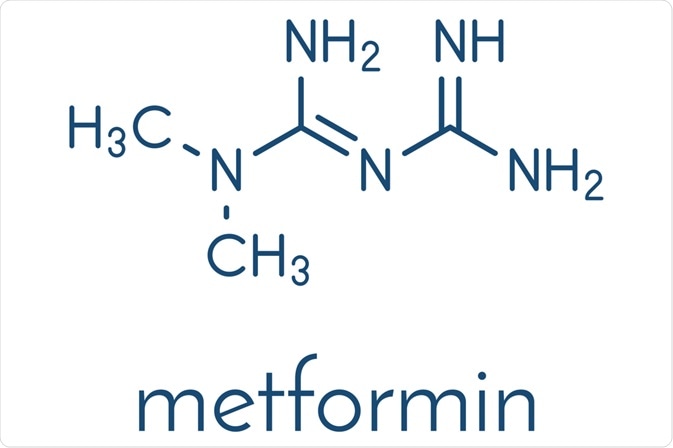
Image Credit: StudioMolekuul / Shutterstock
Structure of metformin and other biguanides
Two guanide molecules joined together are known as biguanides, which is a name that was given by Rathke in 1879 when he obtained a new compound after a condensation reaction of thiourea and phosphorus trichloride with guanidine. The synthesis was henceforth improved by using a condensation reaction at 110 ºC of cyanoguanidine with an ammonia solution of cupric sulfate in a sealed tube.
In 1892 it was discovered that biguanides can be obtained via direct fusion of ammonium chloride with cyanoguanidine at 195 ºC for a couple of minutes. This procedure is still employed in the synthesis of substituted biguanides to detect the presence of biguanides.
To achieve an eco-friendly synthesis of the target molecule, the starting materials are made to react by adjusting the reaction conditions in such a way that the by-products and wastes are eliminated, with minimal use of organic solvents. Thin-layer chromatography has been described as a tool for reaction optimization in microwave-assisted synthesis.
Metformin is a white, hygroscopic crystalline powder with a bitter taste. Chemically it is 1,1 dimethyl-biguanide hydrochloride with a mode of action and uses similar to other biguanides. This small molecule is soluble in water and 95% alcohol; on the other hand, it is practically insoluble in ether or chloroform. Its structure was generally represented in a wrong tautomeric form for several years, but that was corrected in 2005.
When heated to decomposition, metformin emits toxic fumes of nitric oxides. It undergoes negligible hepatic metabolism and is excreted by the kidney with a half-life of approximately two hours. Gas-liquid chromatography, mass fragmentography and high-pressure liquid chromatography are highly specific and most often employed as analytic laboratory methods.
Several studies reported on the crystallographic structure of metformin and its derivates – namely metformin hydrochloride, N, N-dimethylbiguanidium nitrate and metal complexes with metformin. These studies accentuate the importance of π-conjugation (multiple bond systems) and inter-molecular hydrogen bonding.
Four primary end products of oxidation that result from the direct attack of hydroxyl radicals on metformin are a covalent dimer of metformin, hydroperoxide of metformin, methyl-biguanide and 2-amino-4-methylamino-1,3,5-triazine. Under similar conditions, the superoxide radicals are poor initiators of metformin oxidations, suggesting that metformin is not a powerful antioxidant.
Bioavailability and distribution
Metformin is absorbed incompletely and predominantly from the small intestine, with fecal recovery being about 30% of an oral dose. Oral absorption of metformin occurs within 6 hours, with an expected bioavailability of 50 to 60%. The drug is stable, does not bind to plasma proteins and is excreted unchanged in the urine.
The difference between absorbed and available drugs may reflect minor presynaptic clearance of the drug or binding to the intestinal wall. Concomitant food intake may slightly impair metformin absorption. The plasma concentrations are up to 2 µg/ml 1 to 2 hours after an oral dose of 500 to 1000 mg.
Metformin is rapidly eliminated by renal excretion. Although the half-life of metformin is prolonged in patients with kidney impairment, no specific dosage adjustments have been recommended. During controlled clinical trials, maximum metformin plasma levels do not exceed 5 µg/ml – even at maximum doses.
Further Reading
Last Updated: Feb 25, 2023