Introduction to Multiple Sclerosis
Causes of multiple sclerosis
Geographic factors
Lifestyle
Genetics
Haplotypes
Infections
Epstein-Barr virus (EBV)
References
Further reading
Introduction to Multiple Sclerosis
Multiple sclerosis (MS) is a disease caused by damage to the nerve fibers in the central nervous system. This damage disrupts the signals sent to and from the brain. MS is a progressive disease that worsens over time, eventually leading to death.
The central nervous system comprises the brain, spinal cord, and a network of nerves that conduct messages across the body for controlling movements and actions. These nerve fibers are covered by an insulating substance called myelin that protects the nerve and aids the transport of impulses to and from the brain. In MS, this myelin becomes damaged, which interferes with the conduction of nerve signals, which may be slowed or not transported at all.
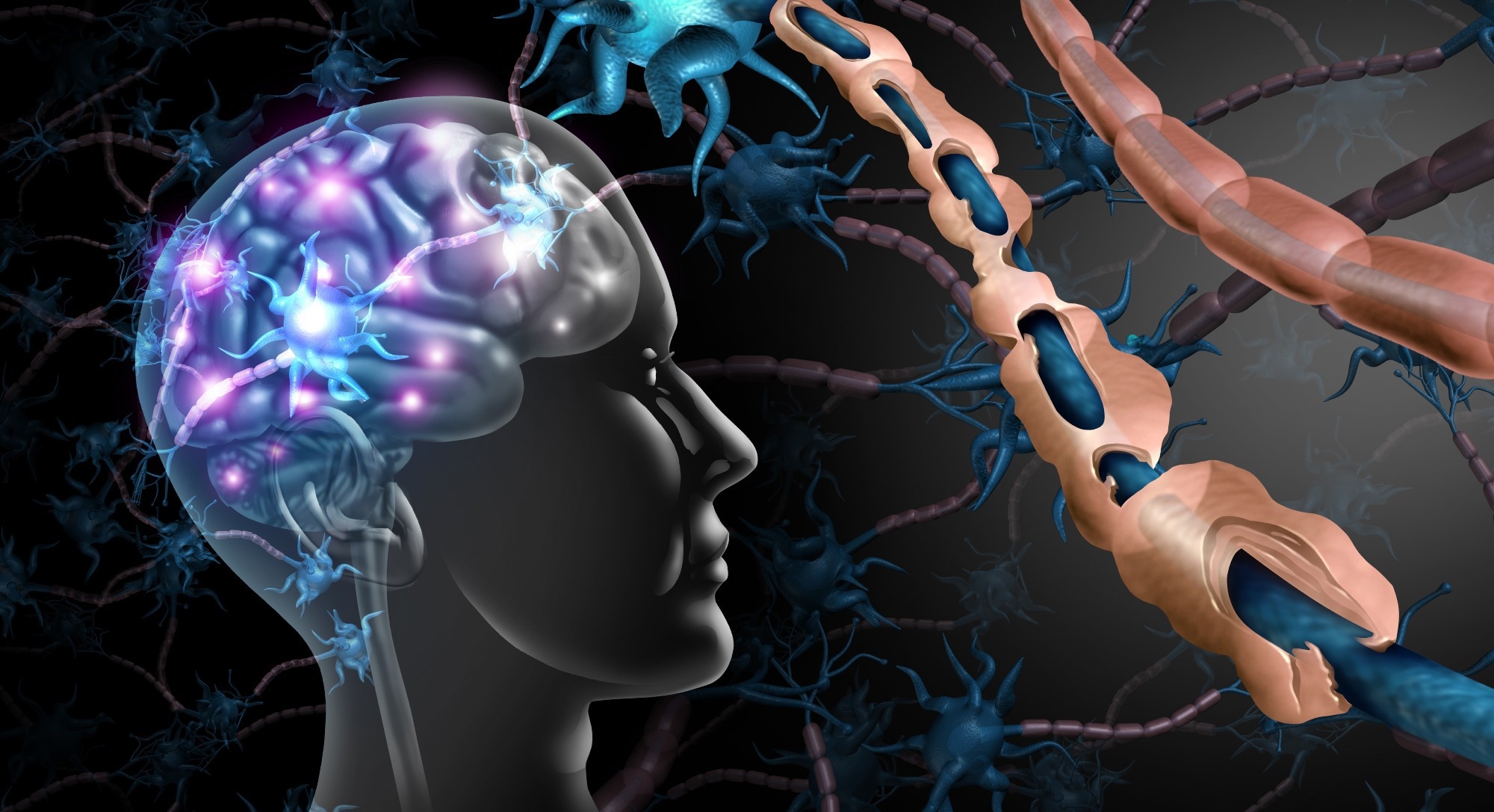
In multiple sclerosis, the immune system mistakes the protective myelin sheath for a foreign body and mounts an attack against it. Image Credit: Lightspring / Shutterstock.com
Causes of multiple sclerosis
Multiple sclerosis is an autoimmune disease. Usually, the immune system protects the body against invading microbes or foreign bodies. Autoimmune diseases, on the other hand, occur when the immune system mistakes healthy body tissue for foreign or damaged tissue.
In MS, the immune system mistakes the protective myelin sheath for a foreign body and mounts an attack against it. This destroys the myelin, which becomes inflamed in small areas called plaques or lesions of demyelination. As the inflammation subsides, the myelin left behind may be scarred (sclerosis), and the nerve fiber underneath may be damaged.
The exact cause of multiple sclerosis is not clearly understood, but genetic and environmental factors seem to play a role in causing the condition.
Geographic factors
Worldwide studies into multiple sclerosis suggest that individuals from countries that lie further north of the equator may be at a greater risk for the condition. Regions such as Canada, USA, UK, Scandinavian countries, southern Australia, and New Zealand have a higher incidence rate of MS than tropical countries.
There is evidence that vitamin D deficiency plays a significant role in the development of MS, which could explain its geographical patterns. Sunlight naturally produces vitamin D in the body, but small amounts can also be obtained from fish and eggs. Therefore, people in countries close to the equator are exposed to direct sunlight for long hours, which results in higher levels of naturally-produced vitamin D, which is believed to play a role in immune function and could provide protection against autoimmune diseases such as MS.
Epidemiologists are also looking for patterns in other environmental factors such as demographics, exposure to environmental agents, and migration patterns to understand the discrepancy in the geographical distribution of MS cases. For example, studies have shown that people who move from high-risk to low-risk areas before puberty has a lower predisposition to MS.
Lifestyle
Studies have also shown certain lifestyle choices to be associated with a higher risk of MS. Smoking is linked to an increased risk of developing MS and increased severity and rapid progression of the disease. The harmful chemicals in cigarette smoke are believed to affect the immune system, and for people with a history of MS in the family, exposure to second-hand smoke can also increase the risk of MS. Fortunately, quitting smoking before or even after the onset of MS is shown to slow down the progression of MS.
Childhood or early adulthood obesity has also been linked to a higher risk of MS. While this does not indicate that all obese people will get MS, obesity is believed to overwork the immune system and trigger inflammation in the body. In addition, vitamin D levels also tend to be lower in overweight people, contributing further to the increased risk of MS.
Genetics
Since no single gene has yet been identified as causing multiple sclerosis, it is not classified as a genetic disease. However, researchers have shown that individuals with a relative who has had MS are more likely to develop it. While it is not strictly hereditary, which means it is not always passed down from one generation to the next, studies have also shown that if an identical twin develops the condition, the risk of the other twin developing MS is one in four. A first-degree relative having MS also increases the risk of MS, although to a lesser degree than an identical twin having MS.
Research into the contribution of specific gene combinations to the risk of developing MS is ongoing. Recent research into genetic susceptibility to MS has revealed that a combination of genetic risk variants in an individual determines the level of risk of MS. One study explored some of the known disease-associated mutations on the genes that code for the major histocompatibility complex system (MHC). Many risk variants are associated with the human leukocyte antigen (HLA), which is responsible for recognizing foreign invading bodies and communicating with the immune cells to launch an immune response.
Haplotypes
Haplotypes are a combination of single nucleotide polymorphisms (one base pair change in a sequence) that occur together and are inherited from a single parent. Researchers studied the association of haplotypes occurring in the regions surrounding the HLA gene to increased risk of MS. The a1 haplotype, which occurs close to the HLA-DRB1 gene, is most significantly associated with MS. Other haplotypes include EOMES, which is involved in T-cell growth, and ZFP36L1 and CLEC16A, which are associated with cell activation.
A collection of such haplotypes, known as conserved extended haplotypes (CEHs), found in the genomic region that houses most of the MHC genes was also studied. The study found that the combination of CEHs in the individual, one inherited from each parent, determined the degree of risk of MS. The H plus haplotype, which carries two of the known MS risk variants, significantly increased the risk of MS susceptibility, with two copies of H plus significantly increasing the risk of MS.
The extended risk CEH (ER), which contains nine disease-associated haplotypes, by itself or in combination with H plus, increases the susceptibility to MS. Women carrying one copy of either H plus or ER have a higher risk of MS than men carrying a single copy of either of those two haplotypes. The study also explored an all-protective CEH (AP) composed of eight disease-protective haplotypes, a neutral CEH (0) without any of the haplotypes from H plus, ER, or AP, and a c1 CEH, which contained a single HLA haplotype.
A combination of the haplotypes inherited from each parent determined the multifold increase or decrease in susceptibility to MS. Various non-HLA haplotypes also increased the risk of MS in conjunction with the HLA CEH pairs. The recent research has improved our understanding of some of the genetic basis of susceptibility to MS. However, the study concluded that while some of these genetic variants can help determine the level of susceptibility to MS, the actual development and progression of MS depends on how these haplotypes interact.
Infections
Some researchers also believe multiple sclerosis may result from a viral infection of the nervous system and/or the immune system. Studies have investigated viral and bacterial diseases such as measles, canine distemper, Chlamydia pneumonia, and mononucleosis for their role in the development of MS. The infectious mononucleosis causing Epstein-Barr virus (EBV) has commonly been implicated as a cause of MS.
Epstein-Barr virus (EBV)
A type of herpes virus, EBV infects about 95% of adults but causes no symptoms in many people. The virus remains latent in most cells post-infection and reactivates in many cases.
A study that looked at blood samples collected every two years over 20 years from more than 10 million active-duty US soldiers as part of routine testing found a much higher rate of EBV infection in people who later developed MS, compared to a control group, which contained people with similar characteristics as the test group who has been infected with EBV but had not developed MS.
 Epstein-Barr virus EBV. Image Credit: Kateryna Kon / Shutterstock
Epstein-Barr virus EBV. Image Credit: Kateryna Kon / Shutterstock
The study calculated that EBV infection made the development of MS 32 times more likely. To bolster the study, the researchers also measured the levels of neurofilament light chain (NfL), a nerve degeneration biomarker, in the blood. They found that the NfL levels in people who developed MS were higher than those without MS, and the increase in NfL levels occurred after the EBV infection and before the MS diagnosis. This proved that MS-associated nerve degeneration had not begun before EBV infection.
While they admit that EBV is not solely responsible for triggering MS, it plays a definite role in the development of MS, along with various unknown factors. The study found no connection between MS and any other human viruses, including cytomegalovirus, which is distantly related to EBV.
The study provides a persuasive line of evidence linking EBV infections to increased risk of MS and signifies a possibly effective way to prevent MS by developing vaccines against EBV. Other studies have shown that preventing EBV infections in people already diagnosed with MS can alter the rate of progression. These new findings linking EBV to increased MS risks have opened up potential avenues to dealing with a debilitating disease.
Multiple Sclerosis in 2022
References
Further Reading
Last Updated: Sep 5, 2022