Amniotic fluid fills the amniotic sac, which is a bag inside a woman’s uterus (womb) where an unborn baby will develop. The amniotic sac provides protection and a constant temperature for the baby to grow in, in addition to providing the baby fluids so that they can breathe, swallow, and develop their musculoskeletal system.
The amniotic sac is sometimes referred to as the membranes, as the sac is made of two membranes; the amnion and the chorion. There are several infections and complications that the amniotic sac is vulnerable to during both pregnancy and birth.
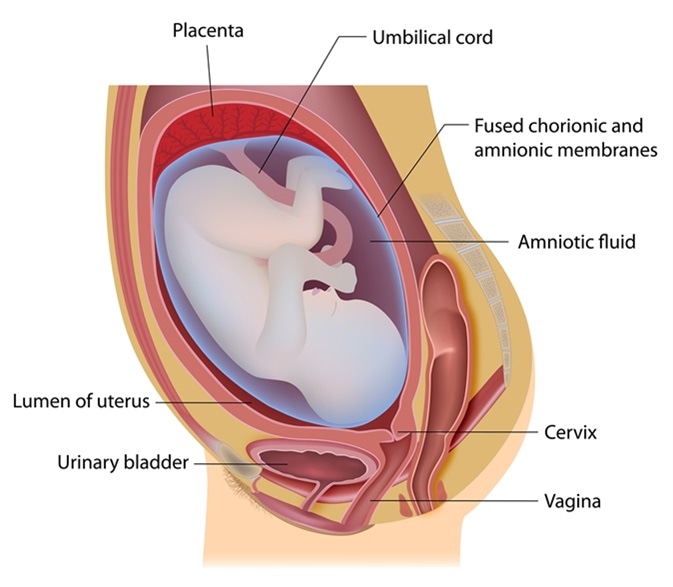
Image Credit: Alila Medical Media / Shutterstock
Composition of amniotic fluid
Within days of conception, the amniotic sac will form and fill with fluid. At the beginning of fetal development, the amniotic fluid will mainly consist of water. As the fetus continues to develop, it will pass small amounts of urine into the fluid from around 10 weeks of pregnancy onwards. Amniotic fluid is a clear, pale straw color.
Where does it go?
Either before or during labor, the amniotic sac will break and the amniotic fluid will drain through the vagina, either gradually or in a sudden rush. This process is commonly known as when a woman's ‘water breaks.’ The risk of infection increases after the amniotic sac breaks; therefore, medical attention should be sought quickly.
What is Amniotic Fluid Made Of?
Medical uses for amniotic fluid
A test called an amniocentesis is offered to some pregnant women if there is a higher chance that their baby might have a genetic condition such as Down’s syndrome, Edwards’ syndrome, or Patau’s syndrome. This test involves taking a small number of cells from the amniotic fluid to test for these conditions.
There are some risks associated with an amniocentesis, including:
- Miscarriage
- Infection
- The need to repeat the test at a later date
Because of these factors, an amniocentesis is carried out after 15 weeks of pregnancy, as the risk of complications is reduced after this point.
The volume of amniotic fluid can also be used to predict adverse pregnancy outcomes; however, this method’s predictive abilities are disputed.
Complications
There are several complications that can occur concerning the amniotic sac, some of which include polyhydramnios, oligohydramnios, amniotic fluid embolism, and chorioamnionitis.
Polyhydramnios
Polyhydramnios is a condition in which there is too much amniotic fluid surrounding the fetus. The symptoms of polyhydramnios include:
- Breathlessness
- Swollen feet
- Heartburn
- Constipation
These symptoms are common problems for many pregnant women and do not always signify polyhydramnios. There is a slightly increased risk of premature birth and problems with the baby’s position or the baby’s umbilical cord in causes of polyhydramnios.
What does it mean if my doctor says I have high amniotic fluid levels?
Oligohydramnios
Oligohydramnios is when there is reduced amniotic fluid surrounding a fetus in the uterus. This condition can affect the baby’s ability to turn to the correct position for birth or cause umbilical cord compression.
The amount of fluid can be increased by increasing liquid consumption; however, the positive results of this treatment are not conclusive. Therefore, controlled clinical trials are required to definitively assess the clinical benefits and risks to both the mother and the baby for increasing liquid consumption to correct oligohydramnios.
Amniotic fluid embolism
Amniotic fluid embolism (AFE) is a sudden cardiorespiratory collapse and, thus, a medical emergency. The cause of AFE is not completely understood.
It is currently estimated that AFE occurs in one case for every 8,000-30,000 pregnancies. Some of the common symptoms of AFE include:
- Agitation
- Hypotension
- Dyspnea
- Evidence of fetal compromise
- Coagulopathy
- Altered mentation
Risk factors of AFE
No specific race or ethnicity is thought to be more susceptible to AFE, although one study has suggested a predilection in non-Hispanic black women. There is a suggestion of increased incidence in women of a higher maternal age, which has been reported in at least two studies.
Other reported risk factors for AFE include:
- Multiparity
- Male fetus
- Trauma
- Medical induction of labor
- Cesarean section
- Placenta previa
- Cervical laceration
- Uterine rupture
Maternal survival of AFE is uncommon; however, successful pregnancies have been reported after pregnancies that have been complicated by AFE. The risk of AFE reoccurrence is currently unknown.
Chorioamnionitis
Chorioamnionitis, or intra-amniotic infection (IAI), is characterized by acute inflammation of the amnion and chorion. This condition is due to a bacterial infection in the fetal membranes, amniotic fluid, and placenta that has ascended from the vagina into the uterus.
For a newborn baby, chorioamnionitis can cause problems such as whole-body inflammation, sepsis, pneumonia, and meningitis. This condition can also present problems for the mother, including pelvic infection, sepsis, postpartum hemorrhage, and an increased risk of cesarean delivery.
Some of the risk factors for chorioamnionitis include:
- Prolonged active labor
- Meconium staining of amniotic fluid (dark green liquid passed by a newborn baby containing mucus, bile, and epithelial cells)
- Various digital vaginal examinations
Research into amniotic fluid stem cells (AFSCs) has continued to increase in the field of regenerative medicine. Some of the potential uses for AFSCs include:
- Tissue reconstruction
- Regeneration of neural tissue
- Cardiac, kidney, and lung epithelial regeneration
- Bone and cartilage engineering
The promise of amniotic fluid in regenerative medicine lies in the cell’s inability to form tumors after in vivo implantation. A better understanding of AFSCs is necessary before research progresses to human trials.
Conclusion
Amniotic fluid is produced to help an unborn baby grow its musculoskeletal system and protect the fetus from injury. Complications concerning the amniotic sac, such as AFE, are not fully understood due to inconsistent reporting in nonfatal cases and inaccurate initial diagnoses. Complications can also arise from bacterial infections.
Promising research is being conducted to investigate how AFSCs can be used in regenerative medicine. While results so far have been positive, further research is necessary to develop a better understanding of its applications in human trials.
References
Further Reading
Last Updated: Apr 8, 2023